Journal of Traditional Chinese Medicine ›› 2022, Vol. 42 ›› Issue (6): 988-996.DOI: 10.19852/j.cnki.jtcm.20220902.002
• Research Articles • Previous Articles Next Articles
Effectiveness of Jiedu granule (解毒颗粒) on gut microbiota in patients with advanced hepatocellular carcinoma: a randomized controlled trial
FAN Yifu, ZHAO Hetong, ZHANG Yani, Yani Zifei, DU Juan( ), LING Changquan(
), LING Changquan( )
)
- School of Traditional Chinese Medicine, Navy Medical University, Shanghai 200433, China
-
Received:2021-10-18Accepted:2022-01-05Online:2022-12-15Published:2022-09-02 -
Contact:DU Juan,LING Changquan -
About author:Prof. Du Juan, School of Traditional Chinese Medicine, Navy Medical University, Shanghai 200433, China. dujuan714@163.com, Telephone: +86-21-81873143; +86-21-81873145
Prof. LING Changquan, School of Traditional Chinese Medicine, Navy Medical University, Shanghai 200433, China. changquanling@smmu.edu.cn;
-
Supported by:Value of Heat Clearing and Detoxification in the Treatment of Primary Liver Cancer from the Perspective of Tumor Inflammatory Microenvironment(81430101);Explore the Mechanism of Sanshimao Granule on Anti-recurrence and Metastasis of Liver Cancer from the Perspective of Sec62 Regulating ER Stress(81473487);Molecular Mechanism of Aconitum Decoction in Interfering with Immune Escape of Hepatocellular Carcinoma via Regulating the Spectrum Shift of NK Cell Receptor/Ligand(81774244)
Cite this article
FAN Yifu, ZHAO Hetong, ZHANG Yani, Yani Zifei, DU Juan, LING Changquan. Effectiveness of Jiedu granule (解毒颗粒) on gut microbiota in patients with advanced hepatocellular carcinoma: a randomized controlled trial[J]. Journal of Traditional Chinese Medicine, 2022, 42(6): 988-996.
share this article
| Characteristic | JDG group (n = 10) | Control group (n = 10) | P value |
|---|---|---|---|
| Age | 53±12 | 49±8 | 0.43 |
| Sex [n (%)] | > 0.05 | ||
| Male | 10 (100) | 9 (90) | |
| Female | 0 | 1 (10) | |
| Tumor size | 6±5 | 7±4 | 0.84 |
| AFP | 581±783 | 589±760 | 0.98 |
| Infected with HBV [n (%)] | > 0.05 | ||
| Yes | 9 (90) | 9 (90) | |
| No | 1 (10) | 1 (10) |
Table 1 Characteristics of HCC patients in JDG group and control group
| Characteristic | JDG group (n = 10) | Control group (n = 10) | P value |
|---|---|---|---|
| Age | 53±12 | 49±8 | 0.43 |
| Sex [n (%)] | > 0.05 | ||
| Male | 10 (100) | 9 (90) | |
| Female | 0 | 1 (10) | |
| Tumor size | 6±5 | 7±4 | 0.84 |
| AFP | 581±783 | 589±760 | 0.98 |
| Infected with HBV [n (%)] | > 0.05 | ||
| Yes | 9 (90) | 9 (90) | |
| No | 1 (10) | 1 (10) |
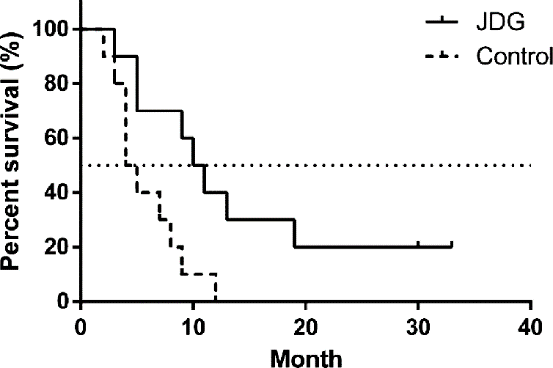
Figure 2 OS of the patients in JDG and control group In JDG group, the patients would be treated with JDG twice a day for two months while the patients in control group would not take any JDG. JDG: Jiedu granule; OS: overall survival.
| Time | JDG group (n = 10) | Control group (n = 10) | F value | P value | ||||
|---|---|---|---|---|---|---|---|---|
| Time | Time × group | Time | Time × group | |||||
| Day 0 | 0.17±0.22 | 0.12±0.19 | 3.726 | 4.232 | 0.034 | 0.303 | ||
| Day 30 | 0.09±0.16 | 0.11±0.20 | ||||||
| Day 60 | 0.02±0.04 | 0.08±0.10 | ||||||
Table 2 Variation tendency of Clostridium XI
| Time | JDG group (n = 10) | Control group (n = 10) | F value | P value | ||||
|---|---|---|---|---|---|---|---|---|
| Time | Time × group | Time | Time × group | |||||
| Day 0 | 0.17±0.22 | 0.12±0.19 | 3.726 | 4.232 | 0.034 | 0.303 | ||
| Day 30 | 0.09±0.16 | 0.11±0.20 | ||||||
| Day 60 | 0.02±0.04 | 0.08±0.10 | ||||||
| Time | JDG group (n = 10) | Control group (n = 10) | F value | P value | ||||
|---|---|---|---|---|---|---|---|---|
| Time | Time × group | Time | Time × group | |||||
| Day 0 | 0.14±0.18 | 0.11±0.18 | 3.423 | 1.225 | 0.044 | 0.306 | ||
| Day 30 | 0.06±0.08 | 0.10±0.19 | ||||||
| Day 60 | 0.02±0.03 | 0.08±0.10 | ||||||
Table 3 Variation tendency of Peptostreptococcaceae
| Time | JDG group (n = 10) | Control group (n = 10) | F value | P value | ||||
|---|---|---|---|---|---|---|---|---|
| Time | Time × group | Time | Time × group | |||||
| Day 0 | 0.14±0.18 | 0.11±0.18 | 3.423 | 1.225 | 0.044 | 0.306 | ||
| Day 30 | 0.06±0.08 | 0.10±0.19 | ||||||
| Day 60 | 0.02±0.03 | 0.08±0.10 | ||||||
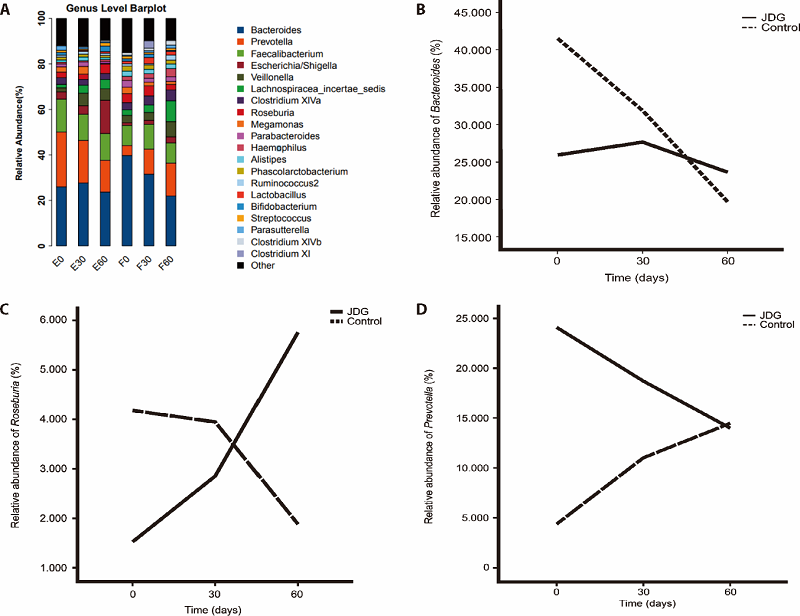
Figure 3 Variation tendency of relative abundance of bacteria on genus level A: genus lever barplot; B-D: the variation tendency of Bacteroides, Roseburia and Prevotella over time in the two groups, respectively. JDG: Jiedu granule.
| Time | JDG group (n = 10) | Control group (n = 10) | F value | P value | ||||
|---|---|---|---|---|---|---|---|---|
| Time | Time × group | Time | Time × group | |||||
| Day 0 | 24±25 | 4±8 | 0.014 | 2.893 | 0.986 | 0.068 | ||
| Day 30 | 19±28 | 11±18 | ||||||
| Day 60 | 14±22 | 14±21 | ||||||
Table 4 Variation tendency of Provotella
| Time | JDG group (n = 10) | Control group (n = 10) | F value | P value | ||||
|---|---|---|---|---|---|---|---|---|
| Time | Time × group | Time | Time × group | |||||
| Day 0 | 24±25 | 4±8 | 0.014 | 2.893 | 0.986 | 0.068 | ||
| Day 30 | 19±28 | 11±18 | ||||||
| Day 60 | 14±22 | 14±21 | ||||||
| Time | JDG group (n = 10) | Control group (n = 10) | F value | P value | ||||
|---|---|---|---|---|---|---|---|---|
| Time | Time × group | Time | Time × group | |||||
| Day 0 | 26±17 | 42±23 | 12.397 | 4.232 | < 0.001 | 0.032 | ||
| Day 30 | 28±22 | 32±19 | ||||||
| Day 60 | 24±21 | 20±16 | ||||||
Table 5 Variation tendency of Bacteroides
| Time | JDG group (n = 10) | Control group (n = 10) | F value | P value | ||||
|---|---|---|---|---|---|---|---|---|
| Time | Time × group | Time | Time × group | |||||
| Day 0 | 26±17 | 42±23 | 12.397 | 4.232 | < 0.001 | 0.032 | ||
| Day 30 | 28±22 | 32±19 | ||||||
| Day 60 | 24±21 | 20±16 | ||||||
| Time | JDG group (n = 10) | Control group (n = 10) | F value | P value | ||||
|---|---|---|---|---|---|---|---|---|
| Time | Time × group | Time | Time × group | |||||
| Day 0 | 1.5±1.7 | 4.2±5.0 | 0.326 | 4.024 | 0.725 | 0.029 | ||
| Day 30 | 2.8±2.4 | 4.0±5.4 | ||||||
| Day 60 | 5.8±5.5 | 1.9±1.5 | ||||||
Table 6 Variation tendency of Roseburia
| Time | JDG group (n = 10) | Control group (n = 10) | F value | P value | ||||
|---|---|---|---|---|---|---|---|---|
| Time | Time × group | Time | Time × group | |||||
| Day 0 | 1.5±1.7 | 4.2±5.0 | 0.326 | 4.024 | 0.725 | 0.029 | ||
| Day 30 | 2.8±2.4 | 4.0±5.4 | ||||||
| Day 60 | 5.8±5.5 | 1.9±1.5 | ||||||

Figure 4 Variation tendency of relative abundance of bacteria on family level A: family lever barplot; B represents the variation tendency of Lachnospiraceae over time in the two groups. JDG: Jiedu granule.
| Time | JDG group (n = 10) | Control group (n = 10) | F value | P value | ||||
|---|---|---|---|---|---|---|---|---|
| Time | Time × group | Time | Time × group | |||||
| Day 0 | 18±18 | 17±6 | 0.360 | 3.508 | 0.701 | 0.044 | ||
| Day 30 | 14±8 | 23±12 | ||||||
| Day 60 | 11±9 | 31±20 | ||||||
Table 7 Variation tendency of Lachnospiraceae
| Time | JDG group (n = 10) | Control group (n = 10) | F value | P value | ||||
|---|---|---|---|---|---|---|---|---|
| Time | Time × group | Time | Time × group | |||||
| Day 0 | 18±18 | 17±6 | 0.360 | 3.508 | 0.701 | 0.044 | ||
| Day 30 | 14±8 | 23±12 | ||||||
| Day 60 | 11±9 | 31±20 | ||||||
| [1] |
Chen W, Zheng R, Baade PD, et al. Cancer statistics in China, 2015. CA Cancer J Clin, 2016; 66: 115-32.
DOI URL |
| [2] |
Zheng R, Qu C, Zhang S, et al. Liver cancer incidence and mortality in China: temporal trends and projections to 2030. Chin J Cancer Res 2018; 30: 571-9.
DOI URL |
| [3] | Li N, Zhu Y. Targeting liver cancer stem cells for the treatment of hepatocellular carcinoma. Therap Adv Gastroenterol 2019; 12: 1756284818821560. |
| [4] |
Caussy C, Tripathi A, Humphrey G, et al. A gut microbiome signature for cirrhosis due to nonalcoholic fatty liver disease. Nat Commun 2019; 10: 1406.
DOI PMID |
| [5] |
Loomba R, Seguritan V, Li W, et al. Gut microbiome-based metagenomic signature for non-invasive detection of advanced fibrosis in human nonalcoholic fatty liver disease. Cell Metab 2019; 30: 607.
DOI PMID |
| [6] |
Oh TG, Kim SM, Caussy C, et al. A universal gut-microbiome-derived signature predicts cirrhosis. Cell Metab 2020; 32: 878-88.
DOI PMID |
| [7] |
Loomba R, Seguritan V, Li W, et al. Gut microbiome-based metagenomic signature for non-invasive detection of advanced fibrosis in human nonalcoholic fatty liver disease. Cell Metab 2017; 25: 1054-62.
DOI PMID |
| [8] |
Ponziani FR, Bhoori S, Castelli C, et al. Hepatocellular carcinoma is associated with gut microbiota profile and inflammation in nonalcoholic fatty liver disease. Hepatology 2019; 69: 107-20.
DOI PMID |
| [9] |
Ren Z, Li A, Jiang J, et al. Gut microbiome analysis as a tool towards targeted non-invasive biomarkers for early hepatocellular carcinoma. Gut 2019; 68: 1014-23.
DOI PMID |
| [10] |
Loo TM, Kamachi F, Watanabe Y, et al. Gut microbiota promotes obesity-associated liver cancer through PGE2-mediated suppression of antitumor immunity. Cancer Discov 2017; 7: 522-38.
DOI URL |
| [11] |
Yoshimoto S, Loo TM, Atarashi K, et al. Obesity-induced gut microbial metabolite promotes liver cancer through senescence secretome. Nature 2013; 499: 97-101.
DOI URL |
| [12] |
Ma C, Han M, Heinrich B, et al. Gut microbiome-mediated bile acid metabolism regulates liver cancer via NKT cells. Science 2018; 360: eaan5931.
DOI URL |
| [13] |
Gao L, Wang KX, Zhou YZ, Fang JS, Qin XM, Du GH. Uncovering the anticancer mechanism of compound Kushen Injection against HCC by integrating quantitative analysis, network analysis and experimental validation. Sci Rep 2018; 8: 624.
DOI PMID |
| [14] |
Bao Y, Wang S, Yang X, Li T, Xia Y, Meng X. Metabolomic study of the intervention effects of Shuihonghuazi formula, a traditional Chinese medicinal formulae, on hepatocellular carcinoma (HCC) rats using performance HPLC/ESI-TOF-MS. J Ethnopharmacol 2017; 198: 468-78.
DOI PMID |
| [15] |
Abou-Hashem MMM, Abo-elmatty DM, Mesbah NM, El-Mawgoud AMA. Induction of sub-G0 arrest and apoptosis by seed extract of Moringa peregrina (Forssk.) Fiori in cervical and prostate cancer cell lines. J Integr Med 2019; 17: 410-22.
DOI PMID |
| [16] |
Oliveira CR, Spindola DG, Garcia DM, et al. Medicinal properties of Angelica archangelica root extract: cytotoxicity in breast cancer cells and its protective effects against in vivo tumor development. J Integr Med 2019; 17: 132-40.
DOI PMID |
| [17] | Ministry of Health of the People’s Republic of China. Standards for diagnosis and treatment of primary liver cancer. Lin Chuang Gan Dan Bing Za Zhi 2011; 27: 1141-56. |
| [18] |
Yu Y, Lang Q, Chen Z, et al. The efficacy for unresectable hepatocellular carcinoma may be improved by transcatheter arterial chemoembolization in combination with a traditional Chinese herbal medicine formula: a retrospective study. Cancer 2009; 115: 5132-8.
DOI PMID |
| [19] |
Zhai XF, Chen Z, Li B, et al. Traditional herbal medicine in preventing recurrence after resection of small hepatocellular carcinoma: a multicenter randomized controlled trial. J Integr Med 2013; 11: 90-100.
DOI URL |
| [20] |
Ticinesi A, Lauretani F, Tana C, Nouvenne A, Ridolo E, Meschi T. Exercise and immune system as modulators of intestinal microbiome implications for the gut-muscle axis hypothesis. Exerc Immunol Rev 2019; 25: 84-95.
PMID |
| [21] |
Yu LX, Schwabe RF. The gut microbiome and liver cancer: mechanisms and clinical translation. Nat Rev Gastroenterol Hepatol 2017; 14: 527-39.
DOI URL |
| [22] |
Wan MLY, El-Nezami H. Targeting gut microbiota in hepatocellular carcinoma: probiotics as a novel therapy. Hepatobiliary Surg Nutr 2018; 7: 11-20.
DOI URL |
| [23] |
Ezzaidi N, Zhang X, Coker OO, Yu J. New insights and therapeutic implication of gut microbiota in non-alcoholic fatty liver disease and its associated liver cancer. Cancer Lett 2019; 459: 186-91.
DOI PMID |
| [24] |
Xu J, Chen HB, Li SL. Understanding the molecular mechanisms of the interplay between herbal medicines and gut microbiota. Med Res Rev 2017; 37: 1140-85.
DOI PMID |
| [25] | Bureau of Medical Administration, National Health and Family Planning Comission of the People’s Republic of China. Standards for diagnosis and treatment of primary liver cancer. Zhong Hua Gan Zang Bing Za Zhi 2017; 25: 886-95. |
| [26] |
Doig GS, Simpson F. Randomization and allocation concealment: a practical guide for researchers. J Crit Care 2005; 20: 187-91.
PMID |
| [27] |
Amato KR, Yeoman CJ, Kent A, et al. Habitat degradation impacts black howler monkey (Alouatta pigra) gastrointestinal microbiomes. ISME J 2013; 7: 1344-53.
DOI PMID |
| [28] |
Ren W, Xun Z, Wang Z, et al. Tongue coating and the salivary microbial communities vary in children with halitosis. Sci Rep 2016; 6: 24481.
DOI PMID |
| [29] |
Xu Y, Wang XS, Chen Y, Shi Q, Chen TH, Li P. A phase II randomized controlled trial of Renshen Yangrong Tang herbal extract granules for fatigue reduction in cancer survivors. J Pain Symptom Manage 2020; 59: 966-73.
DOI URL |
| [30] |
Pan B, Zang J, He J, Wang Z, Liu L. Add-On therapy with Chinese herb medicine Bo-Er-Ning capsule (BENC) improves outcomes of gastric cancer patients: a randomized clinical trial followed with bioinformatics-assisted mechanism study. Am J Cancer Res 2018; 8: 1090-105.
DOI PMID |
| [31] |
Bhargava A, Pathak N, Seshadri S, et al. Pre-clinical validation of mito-targeted nano-engineered flavonoids isolated from Selaginella bryopteris (Sanjeevani) as a novel cancer prevention strategy. Anticancer Agents Med Chem 2018; 18: 1860-74.
DOI URL |
| [32] | Newman TM, Vitolins MZ, Cook KL. From the table to the tumor: the role of mediterranean and Western dietary patterns in shifting microbial-mediated signaling to impact breast cancer risk. Nutrients 2019; 11: E2565. |
| [33] |
Liu D, Jiang XY, Zhou LS. Enriched environment on the intestinal mucosal barrier and brain-gut axis in rats with colorectal cancer. Exp Biol Med (Maywood) 2018; 243: 1185-98.
DOI PMID |
| [34] |
Yoshimoto S, Loo TM, Atarashi K, et al. Obesity-induced gut microbial metabolite promotes liver cancer through senescence secretome. Nature 2013; 499: 97-101.
DOI URL |
| [35] |
Jung MJ, Lee J, Shin NR, et al. Chronic repression of mTOR complex 2 induces changes in the gut microbiota of diet-induced obese mice. Sci Rep 2016; 6: 30887.
DOI URL |
| [36] |
Centuori SM, Martinez JD. Differential regulation of EGFR-MAPK signaling by deoxycholic acid (DCA) and ursodeoxycholic acid (UDCA) in colon cancer. Dig Dis Sci 2014; 59: 2367-80.
DOI URL |
| [37] |
Ahn J, Sinha R, Pei Z, et al. Human gut microbiome and risk for colorectal cancer. J Natl Cancer Inst 2013; 105: 1907-11.
DOI PMID |
| [38] | Galperin MY, Brover V, Tolstoy I, Yutin N. Phylogenomic analysis of the family Peptostreptococcaceae (Clostridium cluster XI) and proposal for reclassification of Clostridium litorale (Fendrich et al. 1991) and Eubacterium acidaminophilum (Zindel et al. 1989) as Peptoclostridium litorale gen. nov. comb. nov. and Peptoclostridium acidaminophilum comb. nov. Int J Syst Evol Microbiol 2016; 66: 5506-13. |
| [39] |
Sobhani I, Tap J, Roudot-Thoraval F, et al. Microbial dysbiosis in colorectal cancer (CRC) patients. PLoS One 2011; 6: e16393.
DOI URL |
| [40] |
Akin H, Tözün N. Diet, microbiota, and colorectal cancer. J Clin Gastroenterol 2014; 48: S67-9.
DOI URL |
| [41] |
Vétizou M, Pitt JM, Daillère R, et al. Anticancer immunotherapy by CTLA-4 blockade relies on the gut microbiota. Science 2015; 350: 1079-84.
DOI URL |
| [42] |
Sivan A, Corrales L, Hubert N, et al. Commensal bifidobacterium promotes antitumor immunity and facilitates anti PD-L1 efficacy. Science 2015; 350: 1084-9.
DOI URL |
| [43] |
Machiels K, Joossens M, Sabino J, et al. A decrease of the butyrate-producing species Roseburia hominis and Faecalibacterium prausnitzii defines dysbiosis in patients with ulcerative colitis. Gut 2014; 63: 1275-83.
DOI PMID |
| [44] |
Jiang S, Xie S, Lv D, et al. A reduction in the butyrate producing species Roseburia spp. and Faecalibacterium prausnitzii is associated with chronic kidney disease progression. Antonie Van Leeuwenhoek 2016; 109: 1389-96.
DOI PMID |
| [45] |
Wu YN, Zhang L, Chen T, Li X, He LH, Liu GX. Granulocyte-macrophage colony-stimulating factor protects mice against hepatocellular carcinoma by ameliorating intestinal dysbiosis and attenuating inflammation. World J Gastroenterol 2020; 26: 5420-36.
DOI URL |
| [46] |
Mondot S, Lepage P, Seksik P, et al. Structural robustness of the gut mucosal microbiota is associated with Crohn’s disease remission after surgery. Gut 2016; 65: 954-62.
DOI PMID |
| [47] |
Vacca M, Celano G, Calabrese FM, Portincasa P, Gobbetti M, De Angelis M. The controversial role of human gut Lachnospiraceae. Microorganisms 2020; 8: 573.
DOI URL |
| [48] |
Meehan CJ, Beiko RG. A phylogenomic view of ecological specialization in the Lachnospiraceae, a family of digestive tract-associated bacteria. Genome Biol Evol 2014; 6: 703-13.
DOI PMID |
| [49] | Dong J, Li W, Dong A, et al. Gene therapy for unresectable hepatocellular carcinoma using recombinant human adenovirus type 5. Med Oncol 2014; 31: 95. |
| [50] |
Fan YF, Zhang HQ, Yang GL, Wu C, Guo YY, Ling CQ. China’s cancer patients’ perceptions, attitudes and participation in clinical trials of complementary and alternative medicine: a multi-center cross-sectional study. Eur J Integr Med 2018; 19: 115-20.
DOI URL |
| [1] | QIN Xiaoyu, WANG Chunai, XUE Jianjun, ZHANG Jie, LU Xiaoting, DING Shengshuang, GE Long, WANG Minzhen. Efficacy of electroacupuncture on myocardial protection and postoperative rehabilitation in patients undergoing cardiac surgery with cardiopulmonary bypass: a systematic review and Meta-analysis [J]. Journal of Traditional Chinese Medicine, 2024, 44(1): 1-15. |
| [2] | DAI Xiaoling, ZHANG Anming, LIN Hui, SHI Bei, REN Yi, WEN Hongzhu, FEI Xiaoyan, LIN Jiang. Qingchang suppositry (清肠栓) induced remission in patients with mild-to-moderate ulcerative proctitis: a multicenter, prospective, randomized, parallel-controlled clinical trial [J]. Journal of Traditional Chinese Medicine, 2024, 44(1): 156-162. |
| [3] | WANG Yichen, WU Shiyi, WANG Zhengyan, CHANG Wenling, XIE Zhihao, TANG Xing, ZHAO Songmei, ZHOU Jing, CHEN Zehong, WANG Chao, YANG Chunxia. Efficacy of Zhumian Tang formula granules (助眠汤配方颗粒) combined with eszopiclone for the treatment of poor sleep quality: a multi-center, randomized controlled, superiority trial [J]. Journal of Traditional Chinese Medicine, 2024, 44(1): 163-171. |
| [4] | YANG Yi, YE Huijun, ZHENG Huiling, JIN Lihua. Clinical observation on 90 cases of primary dysmenorrhea treated by buccal acupuncture therapy: a randomized controlled study [J]. Journal of Traditional Chinese Medicine, 2024, 44(1): 172-181. |
| [5] | WU Jieya, HOU Li, ZHANG Xiaoyuan, Elizabeth Gullen, GAO Chong, WANG Jing. Efficacy of Yisui granule (益髓颗粒) on myelodysplastic syndromes in SKM-1 mouse xenograft model through suppressing Wnt/β-catenin signaling pathway [J]. Journal of Traditional Chinese Medicine, 2024, 44(1): 78-87. |
| [6] | DAI Zeqi, LIAO Xing, GUAN Yueyue, ZENG Zixiu, TANG Jun, HU Jing. Bloodletting puncture in the treatment of acute ischemic stroke: protocol for a mixed-method study of a multi-center randomized controlled trial and focus group [J]. Journal of Traditional Chinese Medicine, 2023, 43(6): 1259-1267. |
| [7] | XU Yani, ZHANG Yutong, HE Weile, DAI Linglin, TANG Ding, WANG Jialing, ZHANG Xufen, CHEN Qin, CHEN Lifang, WANG Zhanglian, ZHAN Mingjie. Efficiency and safety of acupuncture for women with premature ovarian insufficiency: study protocol for a randomized controlled trial [J]. Journal of Traditional Chinese Medicine, 2023, 43(6): 1268-1274. |
| [8] | XU Xiangru, ZHOU Yi, CHEN Gang, LEI Ming, ZHANG Wen, WU Xinxin, PU Yuting, CHEN Caiyu, SUN Yuting, ZHOU Shuang, FANG Bangjiang. Clinical efficacy of Buzhong Yiqi decoction (补中益气汤) in the treatment of hospital-acquired pneumonia with multi-drug resistant bacteria: a prospective, randomized, multicenter controlled trial [J]. Journal of Traditional Chinese Medicine, 2023, 43(5): 1010-1018. |
| [9] | ZHAO Ming, LUO Yimiao, WANG Huichan, CAO Yu, MA Lina, PEI Hui, LI Hao. Guilingji capsule (龟龄集胶囊) for Alzheimer's disease: secondary analysis of a randomized non-inferiority controlled trial [J]. Journal of Traditional Chinese Medicine, 2023, 43(5): 1019-1025. |
| [10] | ZHANG Meizhen, HAO Xiaohui, TANG Yiting, CHEN Yupeng, HE Puyu, ZHAO Liming, PANG Bing, NI Qing. Efficacy and safety of Buyang Huanwu decoction (补阳还五汤) for diabetic peripheral neuropathy: a systematic review and Meta-analysis [J]. Journal of Traditional Chinese Medicine, 2023, 43(5): 841-850. |
| [11] | YANG Yuqing, CHEN Yuhuan, LI Chunxiao, LING Xiao, WANG Panpan, GUO Jing, ZHANG Yingying. Effectiveness and safety of Pingxiao capsule (平消胶囊) as adjuvant therapy in treatment of breast cancer: a systematic review and Meta-analysis [J]. Journal of Traditional Chinese Medicine, 2023, 43(5): 851-859. |
| [12] | WANG Chao, WU Qiong, LI Ping, WANG Zhigang, LOU Xusheng, LI Yuanyuan, ZHANG Lin. Effect of Traditional Chinese Medicine combined with Western Medicine on blood lipid levels and inflammatory factors in patients with angina pectoris in coronary heart disease identified as intermingled phlegm and blood stasis syndrome: a network Meta-analysis [J]. Journal of Traditional Chinese Medicine, 2023, 43(4): 640-649. |
| [13] | JIANG Li, FU Qiang, WANG Shidong, ZHAO Jinxi, CHEN Yu, LI Jiayue, XIAO Yonghua, HUANG Weijun, SUN Ruixi, XIAO Yao, SHEN Aijia, WANG Junheng, LIU Jiangteng, FU Xiaozhe, LI Yuanyuan, ZHAO Yu, XUE Taiqi. Effects of Shenlian formula (参连方) on microbiota and inflammatory cytokines in adults with type 2 diabetes: a double-blind randomized clinical trial [J]. Journal of Traditional Chinese Medicine, 2023, 43(4): 760-769. |
| [14] | ZHANG Xinghe, LI Qifu, YI Rong, XING Chonghui, JIN Yuhao, MENG Jiangqiong, FENG Jialei, ZHAO Siwen, LIANG Fanrong, GUO Taipin. Effect of catgut embedding at acupoints versus non-acupoints in abdominal obesity: a randomized clinical trial [J]. Journal of Traditional Chinese Medicine, 2023, 43(4): 780-786. |
| [15] | CHEN Wenlin, LIANG Fang, ZHANG Yuncheng, LV Jinzhen, YANG Daguo. Effects of Zhenggan Huayu decoction (正肝化瘀方) combined with entecavir on gut microbiota in patients with chronic hepatitis B fibrosis [J]. Journal of Traditional Chinese Medicine, 2023, 43(3): 559-567. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||


