Journal of Traditional Chinese Medicine ›› 2026, Vol. 46 ›› Issue (2): 501-508.DOI: 10.19852/j.cnki.jtcm.2026.02.021
• Reviews • Previous Articles Next Articles
Tongue-coating microbiome as a predictor of solid tumors: an updated scoping review of clinical studies
LI Kexin1, YANG Jinzu2, XIAO Kunlin3, DUAN Shaojie4( ), XIAO Kunmin2(
), XIAO Kunmin2( )
)
- 1
Department of Traditional Chinese Medicine ,Peking Union Medical College Hospital, Peking Union Medical College, Chinese Academy of Medical Sciences Beijing 100730, China
2Department of Oncology ,Longhua Hospital, Shanghai University of Traditional Chinese Medicine Shanghai 200032, China
3Department of Emergency ,Zhongshan Hospital, Fudan University Shanghai 200030, China
4Department of Geriatrics ,Taizhou Central Hospital Taizhou 318000, China
-
Received:2024-12-25Accepted:2025-06-20Online:2026-04-15Published:2026-04-04 -
Contact:XIAO Kunmin, Department of Oncology, Longhua Hospital, Shanghai University of Traditional Chinese Medicine, Shanghai 200032, China. 20170931602@bucm.edu.cn; DUAN Shaojie, Department of Geriatrics, Taizhou Central Hospital, Taizhou 318000, China. 1782802171@qq.com; Telephone: +86-18801020572 -
About author:LI Kexin and YANG Jinzu are co-first authors and contributed equally to this work
Cite this article
LI Kexin, YANG Jinzu, XIAO Kunlin, DUAN Shaojie, XIAO Kunmin. Tongue-coating microbiome as a predictor of solid tumors: an updated scoping review of clinical studies[J]. Journal of Traditional Chinese Medicine, 2026, 46(2): 501-508.
share this article

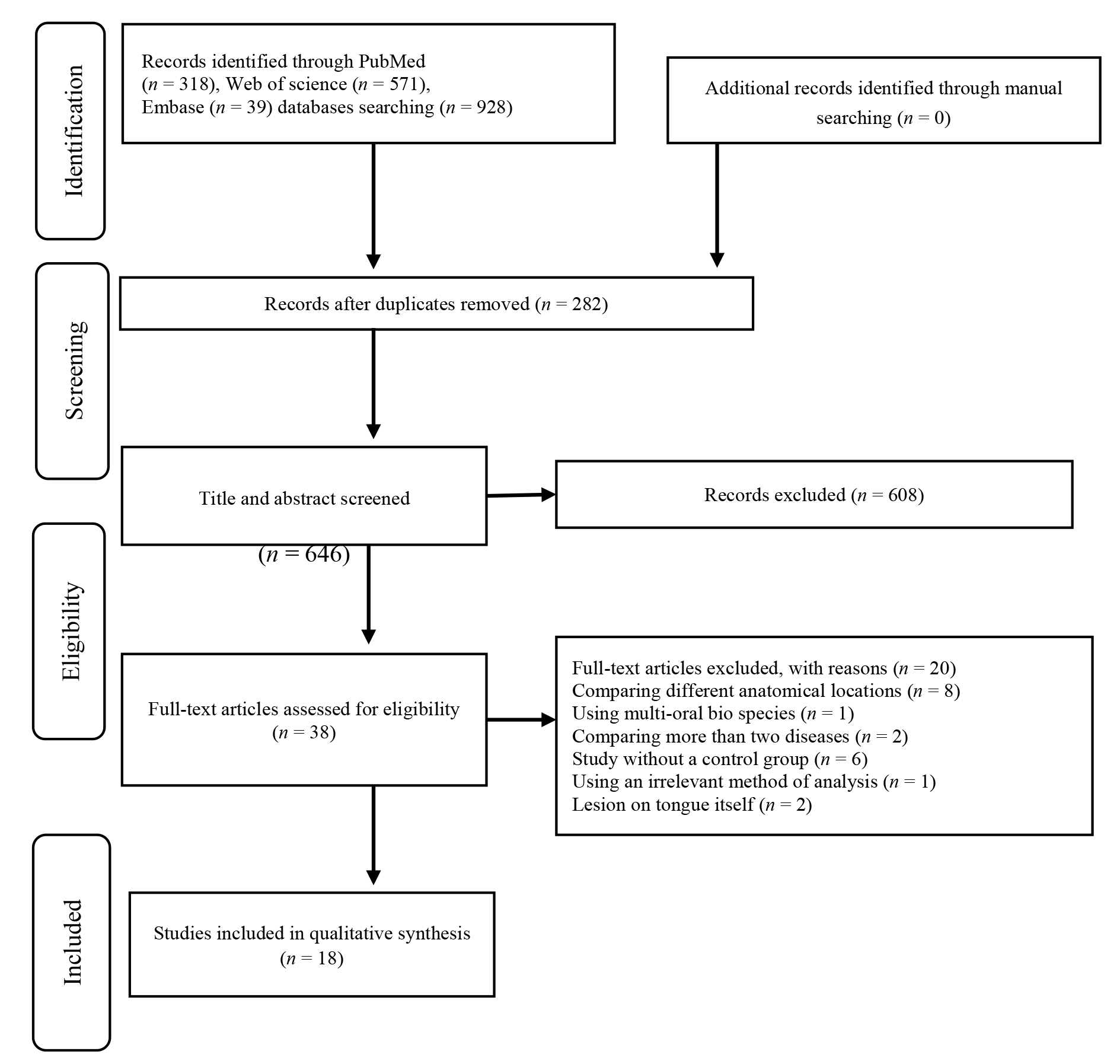
Figure 2 Tongue coating microbiome and metabolic dysregulation in gastric and colorectal tumor progression DCD: dermcidin; KRT2: keratin 2; KRT9: keratin 9; IFN-γ: interferon-γ; IL-1α: interleukin-1α; IL-5: interleukin-5; IL-10: interleukin-10; IL-12: interleukin-12; IL-17α: interleukin-17α; IL-23P40: interleukin-23 subunit p40; TNF-β: tumor necrosis factor-β; VEGF: vascular endothelial growth factor. Red arrows denote disease progression, and black arrows indicate the release of cytokine or lipid release.
| 1. |
He C, Liao Q, Fu P, et al. Microbiological characteristics of different tongue coatings in adults. BMC Microbiol 2022; 22: 214.
DOI PMID |
| 2. |
Zhang Y, Zhao H, Guo Y, et al. Relationship between thick or greasy tongue-coating microbiota and tongue diagnosis in patients with primary liver cancer. Front Microbiol 2022; 13: 903616.
DOI URL |
| 3. | du Toit DF. The tongue: structure and function relevant to disease and oral health. SADJ 2003; 58: 375-76, 380-3. |
| 4. |
Bernardi S, Zeka K, Mummolo S, et al. Development of a new protocol: a macroscopic study of the tongue dorsal surface. Ital J Anat Embryol 2013; 118: 1.
DOI URL |
| 5. |
Seerangaiyan K, Juch F, Winkel E. Tongue coating: Its characteristics and role in intra-oral halitosis and general health: a review. J Breath Res 2017; 12: 034001.
DOI URL |
| 6. |
Liu M, Wang X, Wu F, et al. Variations of oral microbiome in chronic insomnia patients with different tongue features. Am J Chin Med 2020; 48: 923-44.
DOI URL |
| 7. |
Liu Q, Shi K, Bai Y, et al. Biology of tongue coating in different disease stages of RA and its value in disease progression. Microb Pathog 2024; 191: 106644.
DOI URL |
| 8. | Zhao Y, Gou XJ, Dai JY, et al. Differences in metabolites of different tongue coatings in patients with chronic hepatitis B. Evid Based Complement Alternat Med 2013; 2013: 204908. |
| 9. |
Chen J, Sun Y, Li J, et al. In-depth metaproteomics analysis of tongue coating for gastric cancer: A multicenter diagnostic research study. Microbiome 2024; 12: 6.
DOI PMID |
| 10. |
Xu S, Xiang C, Wu J, et al. Tongue coating bacteria as a potential stable biomarker for gastric cancer independent of lifestyle. Dig Dis Sci 2021; 66: 2964-80.
DOI |
| 11. |
Xu J, Xiang C, Zhang C, et al. Microbial biomarkers of common tongue coatings in patients with gastric cancer. Microb Pathog 2019; 127: 97-105.
DOI URL |
| 12. |
Wu J, Xu S, Xiang C, et al. Tongue coating microbiota community and risk effect on gastric cancer. J Cancer 2018; 9: 4039-48.
DOI PMID |
| 13. | Hu J, Han S, Chen Y, et al. Variations of tongue coating microbiota in patients with gastric cancer. Biomed Res Int 2015; 2015: 173729. |
| 14. |
Chen Q, Lin F, Li W, et al. Distinctive lipid characteristics of colorectal cancer revealed through non-targeted lipidomics analysis of tongue coating. J Proteome Res 2024; 23: 2054-66.
DOI PMID |
| 15. |
Chen Q, Huang X, Zhang H, et al. Characterization of tongue coating microbiome from patients with colorectal cancer. J Oral Microbiol 2024; 16: 2344278.
DOI URL |
| 16. |
Han S, Chen Y, Hu J, et al. Tongue images and tongue coating microbiome in patients with colorectal cancer. Microb Pathog 2014; 77: 1-6.
DOI URL |
| 17. |
Ali Mohammed MM, Al Kawas S, Al-Qadhi G. Tongue-coating microbiome as a cancer predictor: a scoping review. Arch Oral Biol 2021; 132: 105271.
DOI URL |
| 18. |
Hao Y, Zhang R, Morris R, et al. Metabolome and microbiome alterations in tongue coating of gastric precancerous lesion patients. Expert Rev Gastroenterol Hepatol 2021; 15: 949-63.
DOI URL |
| 19. | Moher D, Liberati A, Tetzlaff J, et al. Preferred reporting items for systematic reviews and Meta-analyses: the PRISMA statement. PLoS Med 2009; 6: b2535. |
| 20. |
Arksey H, O'Malley L. Scoping studies: towards a methodological framework. Int J Soc Res Methodol 2005; 8: 19-32.
DOI URL |
| 21. |
Chen Y, Li C, Wang X, et al. Oral microbiota distinguishes patients with osteosarcoma from healthy controls. Front Cell Infect Microbiol 2024; 14: 1383878.
DOI URL |
| 22. |
Cui J, Cui H, Yang M, et al. Tongue coating microbiome as a potential biomarker for gastritis including precancerous cascade. Protein Cell 2019; 10: 496-509.
DOI PMID |
| 23. |
He S, Sun Y, Sun W, et al. Oral microbiota disorder in GC patients revealed by 2b-RAD-M. J Transl Med 2023; 21: 831.
DOI PMID |
| 24. |
Lu H, Ren Z, Li A, et al. Tongue coating microbiome data distinguish patients with pancreatic head cancer from healthy controls. J Oral Microbiol 2019; 11: 1563409.
DOI URL |
| 25. |
Lu H, Ren Z, Li A, et al. Deep sequencing reveals microbiota dysbiosis of tongue coat in patients with liver carcinoma. Sci Rep 2016; 6: 33142.
DOI PMID |
| 26. |
Jiang Z, Wang J, Qian X, Zhang Z, Wang S. Oral microbiota may predict the presence of esophageal squamous cell carcinoma. J Cancer Res Clin Oncol 2023; 149: 4731-9.
DOI |
| 27. |
Xiao P, Hua Z, Kang X, et al. Influence of oral intaking habit on tongue coating microbiota in patients with esophageal precancerous lesions. J Cancer 2022; 13: 1168-80.
DOI PMID |
| 28. |
Jain V, Baraniya D, El-Hadedy DE, et al. Integrative metatranscriptomic analysis reveals disease-specific microbiome-host interactions in oral squamous cell carcinoma. Cancer Res Commun 2023; 3: 807-20.
DOI URL |
| 29. |
Gordon DF Jr, Gibbons RJ. Studies of the predominant cultivable micro-organisms from the human tongue. Arch Oral Biol 1966; 11: 627-32.
PMID |
| 30. |
Yokoi A, Maruyama T, Yamanaka R, et al. Relationship between acetaldehyde concentration in mouth air and tongue coating volume. J Appl Oral Sci 2015; 23: 64-70.
DOI PMID |
| 31. |
Jo R, Nishimoto Y, Umezawa K, et al. Comparison of oral microbiome profiles in stimulated and unstimulated saliva, tongue, and mouth-rinsed water. Sci Rep 2019; 9: 16124.
DOI PMID |
| 32. |
Guo XJ, Jiang T, Ma XX, et al. Relationships between diurnal changes of tongue coating microbiota and intestinal microbiota. Front Cell Infect Microbiol 2022; 12: 813790.
DOI URL |
| 33. |
Zeng X, Jin H, Wang C, et al. Establishment of a standard tongue coating collection method for microbiome studies. Biopreserv Biobank 2023; 21: 599-609.
DOI PMID |
| 34. |
Browne HP, Forster SC, Anonye BO, et al. Culturing of 'unculturable' human microbiota reveals novel taxa and extensive sporulation. Nature 2016; 533: 543-6.
DOI |
| 35. |
Forster SC, Kumar N, Anonye BO, et al. A human gut bacterial genome and culture collection for improved metagenomic analyses. Nat Biotechnol 2019; 37: 186-92.
DOI PMID |
| 36. |
Chen Z, Trivedi HM, Chhun N, et al. Using DGGE and 16S rRNA gene sequence analysis to evaluate changes in oral bacterial composition. Chin J Dent Res 2011; 14: 95-103.
PMID |
| 37. |
Sano H, Wakui A, Kawachi M, et al. Profiling system of oral microbiota utilizing polymerase chain reaction-restriction fragment length polymorphism analysis. J Oral Biosci 2021; 63: 292-97.
DOI PMID |
| 38. | Henriques AC, De Marco P. Simple protocol for molecular fingerprinting of human oral microbiota samples in lab classes. J Microbiol Biol Educ 2018; 19: 19.1.1. |
| 39. |
Huang Y, Sheth RU, Zhao S, et al. High-throughput microbial culturomics using automation and machine learning. Nat Biotechnol 2023; 41: 1424-33.
DOI PMID |
| 40. |
Wang X, Howe S, Deng F, Zhao J. Current applications of absolute bacterial quantification in microbiome studies and decision-making regarding different biological questions. Microorganisms 2021; 9: 1797.
DOI URL |
| 41. |
Galazzo G, van Best N, Benedikter BJ, et al. How to count our microbes? The effect of different quantitative microbiome profiling approaches. Front Cell Infect Microbiol 2020; 10: 403.
DOI URL |
| 42. | Zhang J, Su L, Wang Y, Deng S. Improved high-throughput sequencing of the human oral microbiome: from illumina to PacBio. Can J Infect Dis Med Microbiol 2020; 2020: 6678872. |
| 43. |
Li Y, Cui J, Liu Y, Chen K, Huang L, Liu Y. Oral, tongue-coating microbiota, and metabolic disorders: a novel area of interactive research. Front Cardiovasc Med 2021; 8: 730203.
DOI URL |
| 44. |
Vieira AT, Castelo PM, Ribeiro DA, Ferreira CM. Influence of oral and gut microbiota in the health of menopausal women. Front Microbiol 2017; 8: 1884.
DOI PMID |
| 45. | Segata N, Haake SK, Mannon P, et al. Composition of the adult digestive tract bacterial microbiome based on seven mouth surfaces, tonsils, throat and stool samples. Genome Biol 2012; 13: R42. |
| 46. |
Pandey H, Tang DWT, Wong SH, Lal D. Gut microbiota in colorectal cancer: biological role and therapeutic opportunities. Cancers 2023; 15: 866.
DOI URL |
| 47. |
Camañes-Gonzalvo S, Montiel-Company JM, Lobo-de-Mena M, et al. Relationship between oral microbiota and colorectal cancer: a systematic review. J Periodontal Res 2024; 59: 1071-82.
DOI PMID |
| 48. |
Koliarakis I, Messaritakis I, Nikolouzakis TK, Hamilos G, Souglakos J, Tsiaoussis J. Oral bacteria and intestinal dysbiosis in colorectal cancer. Int J Mol Sci 2019; 20: 4146.
DOI URL |
| 49. |
Parhi L, Alon-Maimon T, Sol A, et al. Breast cancer colonization by Fusobacterium nucleatum accelerates tumor growth and metastatic progression. Nat Commun 2020; 11: 3259.
DOI PMID |
| 50. |
Abed J, Emgård JE, Zamir G, et al. Fap2 mediates Fusobacterium nucleatum colorectal adenocarcinoma enrichment by binding to tumor-expressed Gal-GalNAc. Cell Host Microbe 2016; 20: 215-25.
DOI PMID |
| 51. |
Abe K, Fujita M, Hayashi M, Okai K, Takahashi A, Ohira H. Gut and oral microbiota in autoimmune liver disease. Fukushima J Med Sci 2020; 65: 71-5.
DOI PMID |
| 52. |
Kunath BJ, De Rudder C, Laczny CC, Letellier E, Wilmes P. The oral-gut microbiome axis in health and disease. Nat Rev Microbiol 2024; 22: 791-805.
DOI |
| 53. |
Agus A, Clément K, Sokol H. Gut microbiota-derived metabolites as central regulators in metabolic disorders. Gut 2021; 70: 1174-82.
DOI PMID |
| [1] | WANG Xuehui, SUN Yuxin, Birling Yoann, LI Xun, ZHAO Ruotong, ZHENG Youyou, SONG Zhenmei, ZHANG Yanli, DU Hongbo, WANG Jianyun, LI Yinqing, LIU Zhaolan, LIU Jianping. A Meta-analysis of Traditional Chinese Medicine constitution distribution in people with functional constipation [J]. Journal of Traditional Chinese Medicine, 2026, 46(2): 261-273. |
| [2] | Masoumeh Amiri, Mozafar Khazaei, Tayebeh Sadat Tabatabai, Leila Rezakhani. Therapeutic potential of garlic-derived exosome like nanovesicles: challenge and opportunity [J]. Journal of Traditional Chinese Medicine, 2026, 46(2): 509-516. |
| [3] | LIN Lixia, LI Xin, LI Ling, YANG Pu, LU Liming, LIU Buping, SU Shengyong. Multiple acupuncture and moxibustion therapies for allergic rhinitis in adults: a network Meta-analysis of randomized controlled trials [J]. Journal of Traditional Chinese Medicine, 2026, 46(1): 1-13. |
| [4] | YANG Wu, LI Yinghui, LIAO Heng, XIONG Shangbin. Molecular landscape of Berberine's therapeutic potential in gastrointestinal disorders [J]. Journal of Traditional Chinese Medicine, 2026, 46(1): 245-256. |
| [5] | Hyungsun Jun, Nahyun Cho, Wonbae Ha, Junghan Lee, Mi Mi Ko, Young-Eun Kim, Jeeyoun Jung, Jungtae Leem. Key elements for screening kidney deficiency pattern in Traditional Chinese and Korean Medicine: a systematic review and Delphi study [J]. Journal of Traditional Chinese Medicine, 2025, 45(6): 1169-1177. |
| [6] | WANG Ci, CAO Yawen, WANG Jiaying, CHEN Jixin, MA Xue, WANG Xianliang, MAO Jingyuan. Efficacy and safety of acupuncture for arrythmias: an overview of systematic reviews and Meta-analyses [J]. Journal of Traditional Chinese Medicine, 2025, 45(6): 1178-1190. |
| [7] | KONG Lingyao, ZHANG Xiaowen, WANG Xuehui, WANG Zhijie, Robinson Nicola, LIU Jianping. Moxibustion for human immunodeficiency virus and acquired immunodeficiency syndrome and its complications: a systematic review of randomized controlled trials [J]. Journal of Traditional Chinese Medicine, 2025, 45(6): 1201-1214. |
| [8] | ZHANG Gedi, WEN Xiaoli, TAO Tianming, YAN Ziyou, LIU Hongning. Exploration of constructing a relatively comprehensive syndrome differentiation and treatment system based on dialectical materialism principles [J]. Journal of Traditional Chinese Medicine, 2025, 45(5): 1164-1168. |
| [9] | JIANG Jinglei, YU Tao, QIAN Yulin, WANG Meng. Understanding the role of microglia in Alzheimer's disease: insights into mechanisms, acupuncture, and potential therapeutic targets [J]. Journal of Traditional Chinese Medicine, 2025, 45(4): 922-936. |
| [10] | WANG Yiying, DONG Shuai, LI Bo, HAN Mei, CAO Huijuan. Update evidence of effectiveness on pain relieving of cupping therapy: a systematic review and Meta-analysis of randomized controlled trials [J]. Journal of Traditional Chinese Medicine, 2025, 45(2): 234-253. |
| [11] | ZHANG Dingshan, CHEN Li, MARYAM Mazhar, XUE Jinyi, LIU Ping, LIU Mengnan. Application of promoting blood circulation and resolving blood stasis in intracerebral hemorrhage: a traditional method gradually being reconsidered [J]. Journal of Traditional Chinese Medicine, 2025, 45(2): 458-472. |
| [12] | DONG Yingying, GUO Qin, GAO Yuan, WANG Huanhuan, BAI Dong. Revealing the scientific connotation of compatibility of Chinese medicine medica based on self-assembly technology [J]. Journal of Traditional Chinese Medicine, 2024, 44(6): 1288-1295. |
| [13] | XI Hanqing, LI Xia, ZHANG Ziyi, CUI Xiang, JING Xianghong, ZHU Bing, GAO Xinyan. Neuro- and immuno-modulation mediated by the cardiac sympathetic nerve: a novel insight into the anti-ischemic efficacy of acupuncture [J]. Journal of Traditional Chinese Medicine, 2024, 44(5): 1058-1066. |
| [14] | XU Yingshan, WU Chunxiao, YU Wei, GUO Hongji, LU Liming, XU Nenggui, TANG Chunzhi. Systematic review and Meta-analysis of brain plasticity associated with electroacupuncture in experimental ischemic stroke [J]. Journal of Traditional Chinese Medicine, 2024, 44(5): 859-870. |
| [15] | DENG Yasheng, HAN Siyin, XI Lanhua, HUANG Hui, LIANG Tianwei, ZHENG Yiqing, FAN Yanping, LIN Jiang. Traditional Chinese Medicine in the treatment of recurrent respiratory tract infections in children: an overview of systematic reviews and Meta-analyses [J]. Journal of Traditional Chinese Medicine, 2024, 44(5): 871-884. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||