Journal of Traditional Chinese Medicine ›› 2026, Vol. 46 ›› Issue (2): 480-489.DOI: 10.19852/j.cnki.jtcm.20250821.001
• Original Articles • Previous Articles Next Articles
Tongue color tones in Traditional Chinese Medicine correlate with liver histology of metabolic dysfunction-associated steatohepatitis in morbidly obese patients undergoing metabolic and bariatric surgery
CEN Zhikang1, HUANG Bing1, ZHANG Pengfei1, LIU Dongyang1, MO Yanxin1, ZHU Fei1, FAN Mengqi2, NI Zheng1, XU Ying3, LIU Wei4, WU Shuduo5, XU Aimin6,7, SONG Erfei2,8( ), YE Dewei1(
), YE Dewei1( )
)
- 1
Key Laboratory of Metabolic Phenotyping in Model Animals ,Guangdong Pharmaceutical University Guangzhou 510006, China
2Institute of Metabolic Science ,Science and Technology Innovation Center, Guangzhou University of Chinese Medicine Guangzhou 510006, China
3School of Chinese Medicine ,Guangdong Pharmaceutical University Guangzhou 510006, China
4the First Affiliated Hospital of Guangzhou University of Chinese Medicine Guangzhou 510400, China
5Division of Hepatology ,the Second Affiliated Hospital of Guangzhou University of Chinese Medicine Guangzhou 510120, China
6State Key Laboratory of Pharmaceutical Biotechnology ,the University of Hong Kong Hong Kong, China
7Department of Medicine ,The University of Hong Kong Hong Kong 999077, China
8Department of Bariatric Surgery ,the First Affiliated Hospital of Jinan University Guangzhou 510630, China
-
Received:2025-03-31Accepted:2025-06-21Online:2026-04-15Published:2025-08-21 -
Contact:YE Dewei, Key Laboratory of Metabolic Phenotyping in Model Animals, Guangdong Pharmaceutical University, Guangzhou 510006, China. dewei.ye@foxmail.com; Telephone: +86-20-39353115; SONG Erfei, Department of Bariatric Surgery, the First Affiliated Hospital of Jinan University, Guangzhou 510630, China. songerfei@jnu.edu.cn; Telephone: +86-20-38688610 -
Supported by:Immunometabolism Mechanisms Underlying the Development of Chronic Diseases and Therapeutic Benefits of Traditional Chinese Medicine(2024ZD0521005);Functional Investigation of Proteinase 3 in the Development of Diabetic Kidney Diseases and Mechanistic Insights into Therapeutic Benefits of Traditional Chinese Medicine Formula(82374171);Exploration of Pathogenic Role of Neutrophil Extracellular Traps in Increased Susceptibility to Drug-induced Liver Injury under Co-existing Metabolic Dysfunction-associated Steatohepatitis(2024A1515012945);Basic and Translational Investigation of Immunometabolism in Metabolic Diseases(SL2023A04-J01031);Key Laboratory of Model Animal Phenotyping and Basic Research in Metabolic Diseases(2018KSYS003)
Cite this article
CEN Zhikang, HUANG Bing, ZHANG Pengfei, LIU Dongyang, MO Yanxin, ZHU Fei, FAN Mengqi, NI Zheng, XU Ying, LIU Wei, WU Shuduo, XU Aimin, SONG Erfei, YE Dewei. Tongue color tones in Traditional Chinese Medicine correlate with liver histology of metabolic dysfunction-associated steatohepatitis in morbidly obese patients undergoing metabolic and bariatric surgery[J]. Journal of Traditional Chinese Medicine, 2026, 46(2): 480-489.
share this article
| Characteristic | All subjects | Steatosis | Lobular inflammation | |||
|---|---|---|---|---|---|---|
| No | Yes | No | Yes | |||
| Female [n (%)] | 39 (65) | 13 (92.86) | 26 (56.52) | 13 (86.67) | 26 (57.78) | |
| Male [n (%)] | 21 (35) | 1 (7.14) | 20 (43.48) | 2 (13.33) | 19 (42.22) | |
| Age [years, median (IQR)] | 31 (26, 36) | 31.5 (26.75, 33.75) | 31 (25.25, 37.5) | 32 (26, 34.5) | 31 (26, 36) | |
| Weight [kg, median (IQR)] | 113.15 (90.68, 127.58) | 91.25 (72.58, 101.23) | 116.85 (99.7, 131.78) | 95 (76.7, 106.25) | 116.5 (99.5, 131.4) | |
| BMI [kg/m2, median (IQR)] | 38.8 (33.5, 43.6) | 32.65 (30.3, 40.62) | 39.81 (36.34, 44.38) | 33.12 (31.12, 40.45) | 39.93 (36.1, 44.12) | |
| Waist circumference [cm, median (IQR)] | 119.5 (107.63, 131.88) | 106.1 (100.25, 110) | 124 (116.13, 135) | 108 (101, 114) | 124 (116, 135) | |
| ALT [U/L, median (IQR)] | 39 (20.25, 68.25) | 18.5 (16, 27) | 47.5 (32, 75.75) | 19 (16.5, 26) | 47 (32, 76) | |
| AST [U/L, median (IQR)] | 22 (17, 33) | 17 (13.25, 18.75) | 27 (20.25, 38) | 17 (14, 18.5) | 28 (21, 38) | |
| ALP [U/L, median (IQR)] | 80 (64.25, 96.75) | 64.5 (57.25, 85.5) | 83.5 (68.25, 99.5) | 63 (56, 82) | 84 (72, 98) | |
| γ-GT [U/L, median (IQR)] | 37 (23.25, 54) | 25 (17.25, 35.5) | 42 (25.5, 57.25) | 24 (16.5, 29) | 41 (27, 58) | |
| ADA [U/L, median (IQR)] | 12 (10, 14.75) | 10.5 (10, 12) | 12 (10.25, 15) | 10 (9, 12) | 12 (11, 15) | |
| Diabetes [n (%)] | 7 (11.67) | 1 (7.14) | 6 (13.04) | 1 (6.67) | 6 (13.33) | |
| Hypertension [n (%)] | 5 (8.33) | 0 (0) | 5 (10.87) | 0 (0) | 5 (11.11) | |
| TCHOL [mmol/L, median (IQR)] | 5.14 (4.56, 5.94) | 5.62 (4.28, 5.79) | 5.1 (4.8, 6.13) | 5.64 (4.21, 5.88) | 5.08 (4.78, 5.94) | |
| HDL-C [mmol/L, median (IQR)] | 1.02 (0.92, 1.21) | 1.31 (1.03, 1.43) | 0.99 (0.9, 1.12) | 1.3 (1.1, 1.4) | 0.99 (0.89, 1.09) | |
| LDL-C [mmol/L, median (IQR)] | 3.16 (2.7, 3.59) | 3.21 (2.48, 3.43) | 3.12 (2.79, 3.62) | 3.28 (2.54, 3.46) | 3.09 (2.75, 3.6) | |
| TG [mmol/L, median (IQR)] | 1.77 (1.11, 2.48) | 1.2 (1.04, 1.59) | 1.88 (1.38, 2.82) | 1.15 (1.05, 1.65) | 1.89 (1.34, 2.87) | |
| LDH [U/L, median (IQR)] | 201.5 (180.25, 231.5) | 188.5 (166.75, 197.25) | 210.5 (183.25, 238.75) | 193 (165.5, 205.5) | 206 (183, 235) | |
| Uric acid [μmol/L, median (IQR)] | 450.35 (387, 508.23) | 396 (363.75, 444.4) | 468.25 (422.25, 547.98) | 383.7 (364.5, 448.6) | 462.5 (426, 548) | |
| APOA [g/L, median (IQR)] | 1.3 (1.2, 1.39) | 1.37 (1.31, 1.47) | 1.27 (1.19, 1.36) | 1.36 (1.31, 1.44) | 1.26 (1.18, 1.36) | |
| APOB [g/L, median (IQR)] | 0.97 (0.8, 1.2) | 0.93 (0.75, 1.02) | 0.97 (0.83, 1.2) | 0.97 (0.78, 1.15) | 0.97 (0.83, 1.18) | |
| Fasting glucose [mmol/L, median (IQR)] | 5.58 (5.03, 7.02) | 5.1 (4.87, 6.06) | 5.67 (5.24, 7.78) | 5.1 (4.73, 5.92) | 5.68 (5.25, 8.02) | |
| HbA1c [%, median (IQR)] | 5.85 (5.5, 6.88) | 5.6 (5.33, 5.85) | 5.9 (5.6, 7.2) | 5.6 (5.25, 5.85) | 5.9 (5.6, 7.3) | |
| Insulin [mIU/L, median (IQR)] | 22.92 (12.72, 31.76) | 12.36 (10.42, 20.24) | 26.27 (15.77, 31.99) | 12.56 (10.88, 19.42) | 26.39 (15.58, 32.83) | |
| C-peptide [ng/mL, median (IQR)] | 3.68 (2.76, 4.87) | 2.81 (2.45, 3.15) | 4.06 (3.07, 5.12) | 2.77 (2.48, 3.12) | 4.2 (3.14, 5.2) | |
| Transferrin [g/L, median (IQR)] | 2.56 (2.24, 2.94) | 2.74 (2.27, 2.98) | 2.51 (2.24, 2.86) | 2.94 (2.29, 2.99) | 2.47 (2.24, 2.83) | |
| Hepatic steatosis ≥ 1 [n (%)] | 46 (76.67) | - | - | - | - | |
| Hepatocyte ballooning ≥ 1 [n (%)] | 20 (33.33) | - | - | - | - | |
| Lobular inflammation ≥ 1 [n (%)] | 45 (75) | - | - | - | - | |
| Fibrosis [n (%)] | 28 (46.67) | - | - | - | - | |
Table 1 Clinical and histological characteristics of participants
| Characteristic | All subjects | Steatosis | Lobular inflammation | |||
|---|---|---|---|---|---|---|
| No | Yes | No | Yes | |||
| Female [n (%)] | 39 (65) | 13 (92.86) | 26 (56.52) | 13 (86.67) | 26 (57.78) | |
| Male [n (%)] | 21 (35) | 1 (7.14) | 20 (43.48) | 2 (13.33) | 19 (42.22) | |
| Age [years, median (IQR)] | 31 (26, 36) | 31.5 (26.75, 33.75) | 31 (25.25, 37.5) | 32 (26, 34.5) | 31 (26, 36) | |
| Weight [kg, median (IQR)] | 113.15 (90.68, 127.58) | 91.25 (72.58, 101.23) | 116.85 (99.7, 131.78) | 95 (76.7, 106.25) | 116.5 (99.5, 131.4) | |
| BMI [kg/m2, median (IQR)] | 38.8 (33.5, 43.6) | 32.65 (30.3, 40.62) | 39.81 (36.34, 44.38) | 33.12 (31.12, 40.45) | 39.93 (36.1, 44.12) | |
| Waist circumference [cm, median (IQR)] | 119.5 (107.63, 131.88) | 106.1 (100.25, 110) | 124 (116.13, 135) | 108 (101, 114) | 124 (116, 135) | |
| ALT [U/L, median (IQR)] | 39 (20.25, 68.25) | 18.5 (16, 27) | 47.5 (32, 75.75) | 19 (16.5, 26) | 47 (32, 76) | |
| AST [U/L, median (IQR)] | 22 (17, 33) | 17 (13.25, 18.75) | 27 (20.25, 38) | 17 (14, 18.5) | 28 (21, 38) | |
| ALP [U/L, median (IQR)] | 80 (64.25, 96.75) | 64.5 (57.25, 85.5) | 83.5 (68.25, 99.5) | 63 (56, 82) | 84 (72, 98) | |
| γ-GT [U/L, median (IQR)] | 37 (23.25, 54) | 25 (17.25, 35.5) | 42 (25.5, 57.25) | 24 (16.5, 29) | 41 (27, 58) | |
| ADA [U/L, median (IQR)] | 12 (10, 14.75) | 10.5 (10, 12) | 12 (10.25, 15) | 10 (9, 12) | 12 (11, 15) | |
| Diabetes [n (%)] | 7 (11.67) | 1 (7.14) | 6 (13.04) | 1 (6.67) | 6 (13.33) | |
| Hypertension [n (%)] | 5 (8.33) | 0 (0) | 5 (10.87) | 0 (0) | 5 (11.11) | |
| TCHOL [mmol/L, median (IQR)] | 5.14 (4.56, 5.94) | 5.62 (4.28, 5.79) | 5.1 (4.8, 6.13) | 5.64 (4.21, 5.88) | 5.08 (4.78, 5.94) | |
| HDL-C [mmol/L, median (IQR)] | 1.02 (0.92, 1.21) | 1.31 (1.03, 1.43) | 0.99 (0.9, 1.12) | 1.3 (1.1, 1.4) | 0.99 (0.89, 1.09) | |
| LDL-C [mmol/L, median (IQR)] | 3.16 (2.7, 3.59) | 3.21 (2.48, 3.43) | 3.12 (2.79, 3.62) | 3.28 (2.54, 3.46) | 3.09 (2.75, 3.6) | |
| TG [mmol/L, median (IQR)] | 1.77 (1.11, 2.48) | 1.2 (1.04, 1.59) | 1.88 (1.38, 2.82) | 1.15 (1.05, 1.65) | 1.89 (1.34, 2.87) | |
| LDH [U/L, median (IQR)] | 201.5 (180.25, 231.5) | 188.5 (166.75, 197.25) | 210.5 (183.25, 238.75) | 193 (165.5, 205.5) | 206 (183, 235) | |
| Uric acid [μmol/L, median (IQR)] | 450.35 (387, 508.23) | 396 (363.75, 444.4) | 468.25 (422.25, 547.98) | 383.7 (364.5, 448.6) | 462.5 (426, 548) | |
| APOA [g/L, median (IQR)] | 1.3 (1.2, 1.39) | 1.37 (1.31, 1.47) | 1.27 (1.19, 1.36) | 1.36 (1.31, 1.44) | 1.26 (1.18, 1.36) | |
| APOB [g/L, median (IQR)] | 0.97 (0.8, 1.2) | 0.93 (0.75, 1.02) | 0.97 (0.83, 1.2) | 0.97 (0.78, 1.15) | 0.97 (0.83, 1.18) | |
| Fasting glucose [mmol/L, median (IQR)] | 5.58 (5.03, 7.02) | 5.1 (4.87, 6.06) | 5.67 (5.24, 7.78) | 5.1 (4.73, 5.92) | 5.68 (5.25, 8.02) | |
| HbA1c [%, median (IQR)] | 5.85 (5.5, 6.88) | 5.6 (5.33, 5.85) | 5.9 (5.6, 7.2) | 5.6 (5.25, 5.85) | 5.9 (5.6, 7.3) | |
| Insulin [mIU/L, median (IQR)] | 22.92 (12.72, 31.76) | 12.36 (10.42, 20.24) | 26.27 (15.77, 31.99) | 12.56 (10.88, 19.42) | 26.39 (15.58, 32.83) | |
| C-peptide [ng/mL, median (IQR)] | 3.68 (2.76, 4.87) | 2.81 (2.45, 3.15) | 4.06 (3.07, 5.12) | 2.77 (2.48, 3.12) | 4.2 (3.14, 5.2) | |
| Transferrin [g/L, median (IQR)] | 2.56 (2.24, 2.94) | 2.74 (2.27, 2.98) | 2.51 (2.24, 2.86) | 2.94 (2.29, 2.99) | 2.47 (2.24, 2.83) | |
| Hepatic steatosis ≥ 1 [n (%)] | 46 (76.67) | - | - | - | - | |
| Hepatocyte ballooning ≥ 1 [n (%)] | 20 (33.33) | - | - | - | - | |
| Lobular inflammation ≥ 1 [n (%)] | 45 (75) | - | - | - | - | |
| Fibrosis [n (%)] | 28 (46.67) | - | - | - | - | |
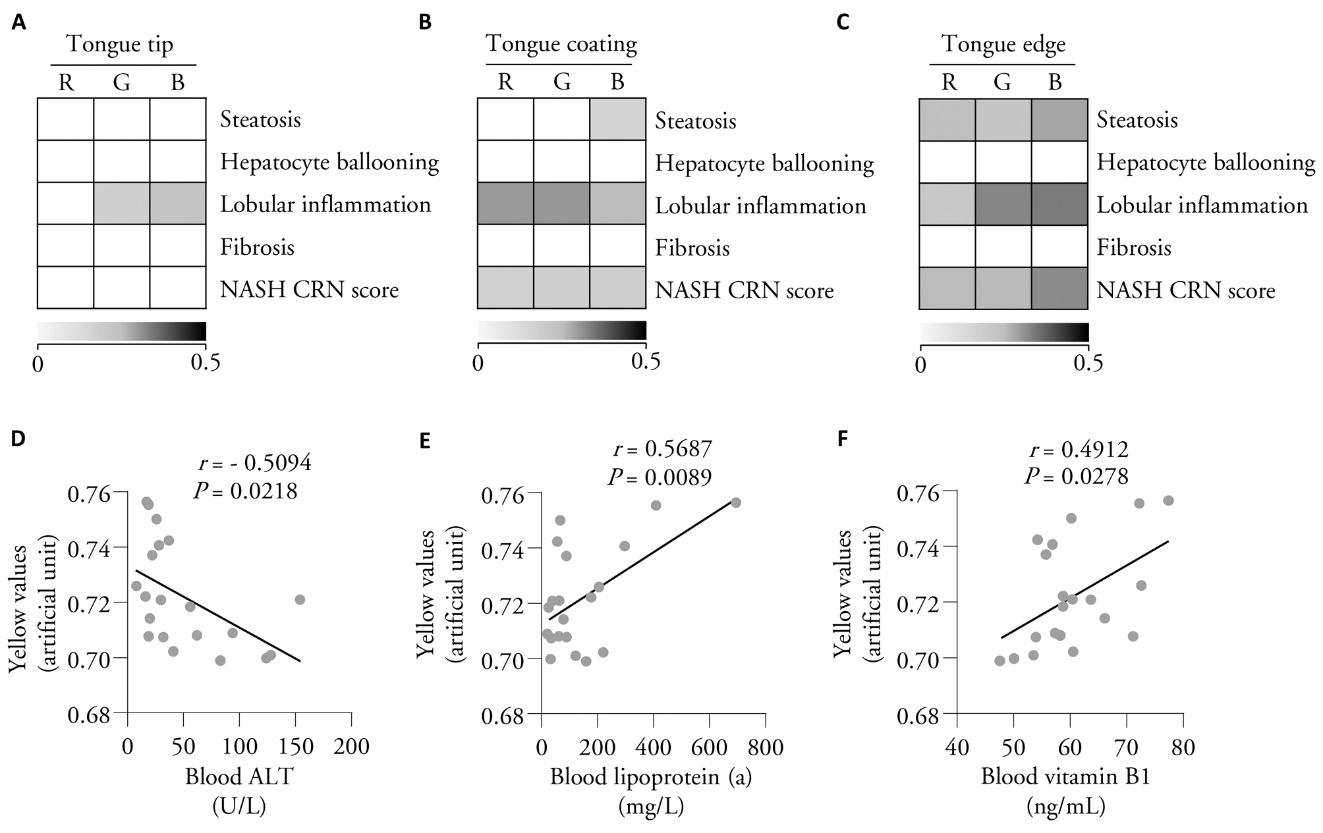
Figure 1 Color tones in distinct zones in the tongue correlated with histological features of MASH in liver biopsy and biochemical parameters A: heat map showing the results of correlation analysis of MASH-specific features (including steatosis, lobular inflammation, hepatocyte ballooning, and NASH CRN scores) with RGB values measured in the tongue tip; B: heat map of MASH-specific features with RGB values measured in tongue coating; C: heat map of correlation analysis of MASH-specific features with RGB values measured in the tongue edge; D: correlation analysis of yellow values in tongue coating with blood levels of ALT in heat-syndrome subgroup; E: correlation analysis of yellow values in tongue coating with blood levels of lipoprotein (a) in heat-syndrome subgroup; F: correlation analysis of yellow values in tongue coating with blood levels of vitamin B1 in heat-syndrome subgroup. NASH CRN: non-alcoholic steatohepatitis clinical research network; ALT: alanine aminotransferase; MASH: metabolic dysfunction-associated steatohepatitis; RGB: red, green, and blue. Statistical analyses were performed using Spearman correlation analysis (panels A-C, n = 60) and Pearson correlation analysis (panels D-F, n = 20).
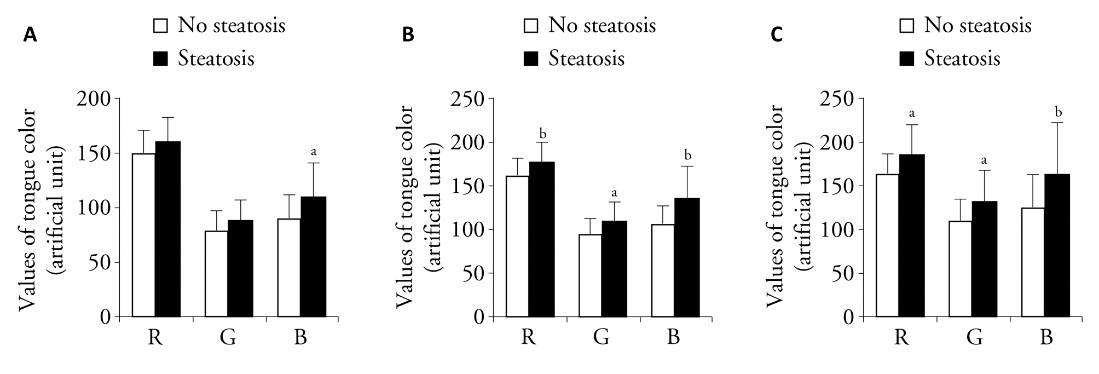
Figure 2 Analysis of RGB values in distinct zones of the tongue in patients with or without histological feature of steatosis in liver biopsies A: values of R, G, and B channels in the zone of tongue tip in subgroup of patients with or without steatosis in liver biopsies; B: values of R, G, and B channels in the zone of tongue coating in subgroup of patients with or without steatosis in liver biopsies; C: values of R, G, and B channels in the zone of tongue edge in subgroup of patients with or without steatosis in liver biopsies. No Steatosis group: absence of significant hepatic steatosis (< 5%) by histology. Steatosis group: presence of ≥ 5% hepatic steatosis by histology. RGB: red, green, and blue. Statistical analyses were measured using one-way analysis of variance for multiple comparisons Data are expressed as mean ± standard deviation (no steatosis: n = 14; steatosis: n = 46). aP < 0.05 and bP < 0.01 vs no steatosis group.
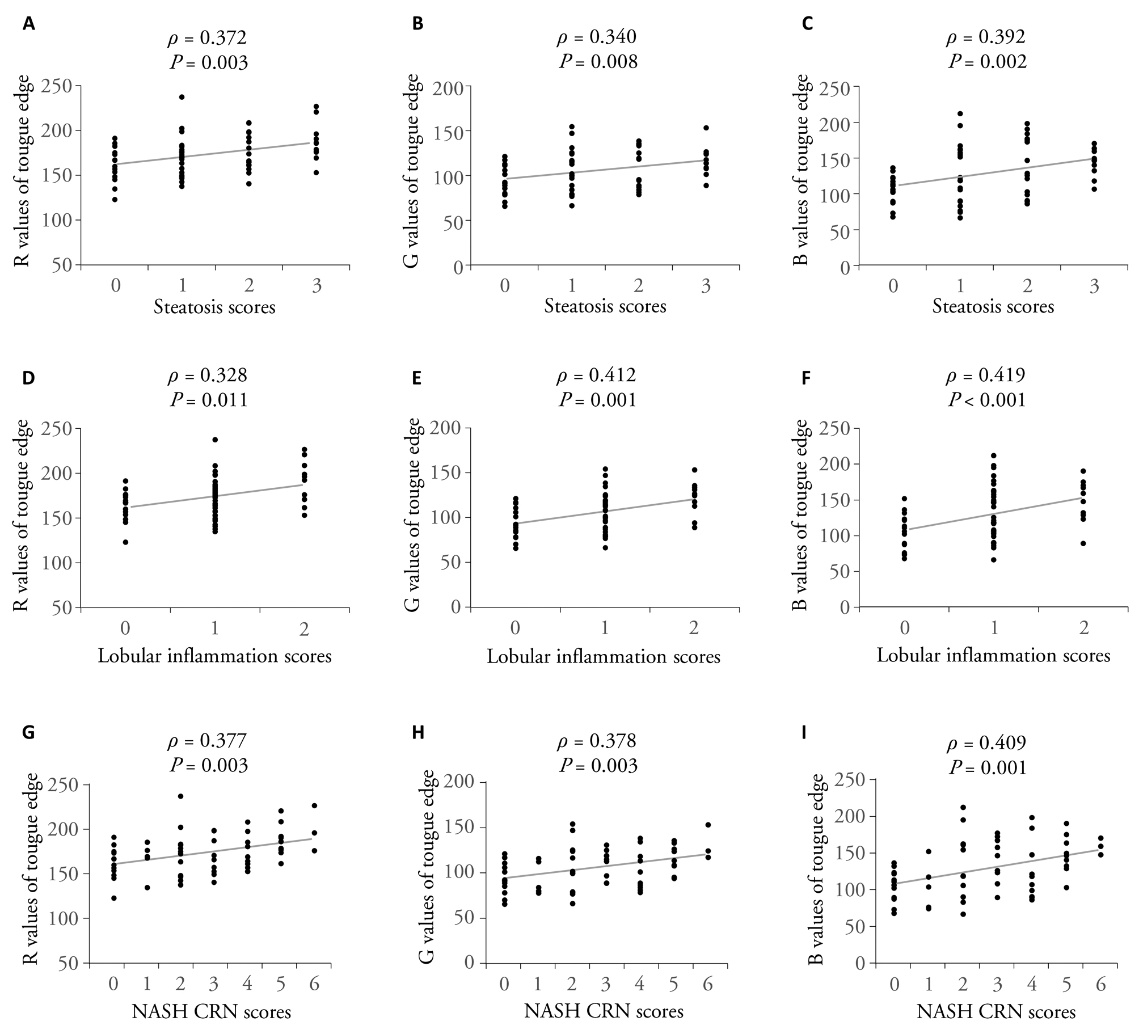
Figure 3 RGB values in tongue edge exhibited a step-wise increase in association with histological grading of MASH in liver biopsies A: values in the channel of R in patients with steatosis score 0, 1, 2, and 3; B: values in the channel of G in patients with steatosis score 0, 1, 2, and 3; C: values in the channel of B in patients with steatosis score 0, 1, 2, and 3; D: values in the channel of R in patients with histological score 0, 1, and 2 of lobular inflammation; E: values in the channel of G in patients with histological score 0, 1, and 2 of lobular inflammation; F: values in the channel of B in patients with histological score 0, 1, and 2 of lobular inflammation; G: values in the channel of R in patients with NASH CRN score 0 to 6; H: values in the channel of G in patients with NASH CRN score 0 to 6; I: values in the channel of B in patients with NASH CRN score 0 to 6. R: red; G: green; B: blue; NASH CRN: non-alcoholic steatohepatitis clinical research network; MASH: metabolic dysfunction-associated steatohepatitis. Statistical analyses were performed using Spearman correlation analysis (n = 60).
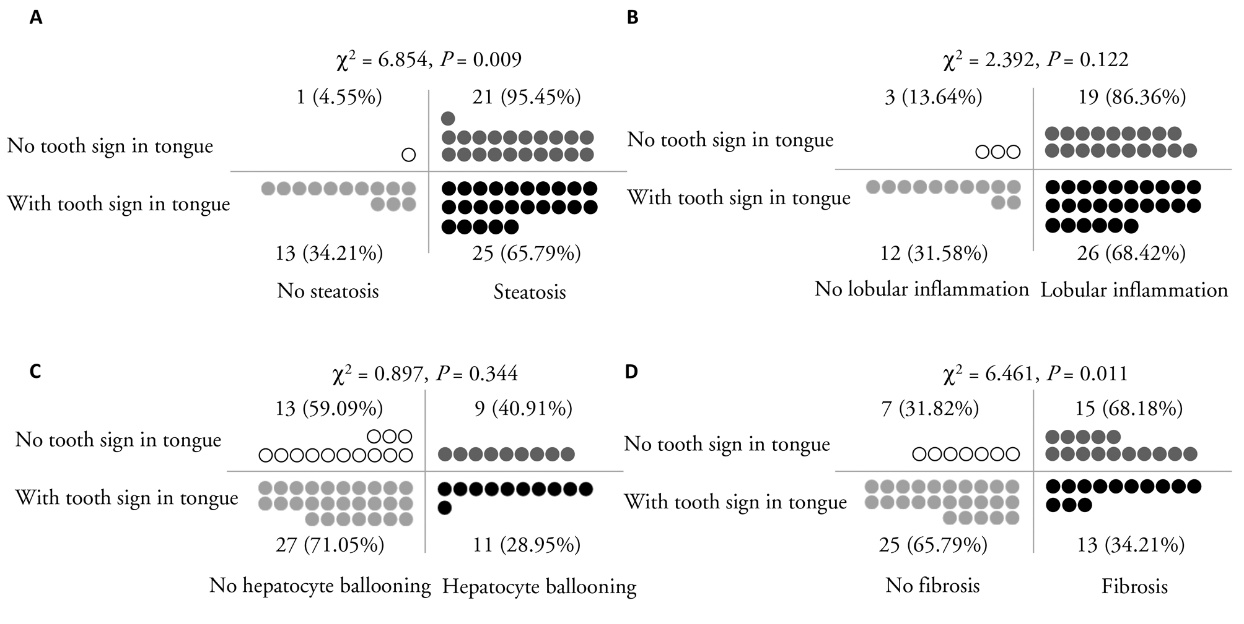
Figure 4 Interaction analysis reveals the distribution of histological features of MASH in patients with or without tooth-sign in tongue A: the distribution and percentage of patients with or without histological feature steatosis in patients with or without tooth-sign in tongue; B: the distribution and percentage of patients with or without histological feature lobular inflammation in patients with or without tooth-sign in tongue; C: the distribution and percentage of patients with or without histological feature hepatocyte ballooning in patients with or without tooth-sign in tongue; D: the distribution and percentage of patients with or without histological feature liver fibrosis in patients with or without tooth-sign in tongue. MASH: metabolic dysfunction-associated steatohepatitis. Statistical analyses were performed using the χ 2 test (n = 60).
| 1. |
Rinella ME, Lazarus JV, Ratziu V, et al. A multisociety Delphi consensus statement on new fatty liver disease nomenclature. J Hepatol 2023; 79: 1542-56.
DOI PMID |
| 2. |
Younossi ZM, Golabi P, Paik JM, Henry A, Van Dongen C, Henry L. The global epidemiology of nonalcoholic fatty liver disease (NAFLD) and nonalcoholic steatohepatitis (NASH): a systematic review. Hepatology 2023; 77: 1335-47.
DOI PMID |
| 3. |
Musso G, Cassader M, Gambino R. Non-alcoholic steatohepatitis: emerging molecular targets and therapeutic strategies. Nat Rev Drug Discov 2016; 15: 249-74.
DOI PMID |
| 4. |
Harrison SA, Bedossa P, Guy CD, et al. A phase 3, randomized, controlled trial of resmetirom in NASH with liver fibrosis. N Engl J Med 2024; 390: 497-509.
DOI URL |
| 5. |
Harrison SA, Allen AM, Dubourg J, Noureddin M, Alkhouri N. Challenges and opportunities in NASH drug development. Nat Med 2023; 29: 562-73.
DOI PMID |
| 6. |
Harrison SA, Dubourg J. Liver biopsy evaluation in MASH drug development: think thrice, act wise. J Hepatol 2024; 81: 886-94.
DOI PMID |
| 7. |
Bedossa P, Patel K. Biopsy and noninvasive methods to assess progression of nonalcoholic fatty liver disease. Gastroenterology 2016; 150: 1811-22.e1814.
DOI PMID |
| 8. | Ji D. Analysis of tongue image in Traditional Chinese Medicine. Tianjin: Tianjin Science & Technology Translation & Publishing Co., Ltd., 2008: 1-9. |
| 9. |
Laskin DM, Giglio JA, Rippert ET. Differential diagnosis of tongue lesions. Quintessence Int 2003; 34: 331-42.
PMID |
| 10. |
Huang DQ, Wong VWS, Rinella ME, et al. Metabolic dysfunction-associated steatotic liver disease in adults. Nat Rev Dis Primers 2025; 11: 14.
DOI PMID |
| 11. |
Wang Y, Fleishman JS, Li T, et al. Pharmacological therapy of metabolic dysfunction-associated steatotic liver disease-driven hepatocellular carcinoma. Front Pharmacol 2023; 14: 1336216.
DOI URL |
| 12. |
Chen M, Xie Y, Gong S, et al. Traditional Chinese Medicine in the treatment of nonalcoholic steatohepatitis. Pharmacol Res 2021; 172: 105849.
DOI URL |
| 13. |
Chalasani N, Younossi Z, Lavine JE, et al. The diagnosis and management of nonalcoholic fatty liver disease: practice guidance from the American Association for the Study of Liver Diseases. Hepatology 2018; 67: 328-57.
DOI PMID |
| 14. |
Fan M, Song E, Zhang Y, et al. Metabolic dysfunction-associated steatohepatitis detected by neutrophilic crown-like structures in morbidly obese patients: a multicenter and clinicopathological study. Research (Wash D C) 2024; 7: 0382.
DOI PMID |
| 15. |
Kleiner DE, Brunt EM, Van Natta M, et al. Design and validation of a histological scoring system for nonalcoholic fatty liver disease. Hepatology 2005; 41: 1313-21.
DOI PMID |
| 16. |
Tincopa MA, Loomba R. Non-invasive diagnosis and monitoring of non-alcoholic fatty liver disease and non-alcoholic steatohepatitis. Lancet Gastroenterol Hepatol 2023; 8: 660-70.
DOI URL |
| 17. | Gao G, Li S, Xue J, et al. Traditional Chinese Medicine syndrome types and syndrome elements of nonalcoholic fatty liver disease. J Clin Hepatol 2021; 37: 89-93. |
| 18. | Zhao M, Peng H, Wang J, et al. Objectified study on tongue image of Traditional Chinese Medicine in patients with different risk stages of chronic atrophic gastritis. Shanxi Zhong Yi 2025; 46: 756-60. |
| 19. |
Sanyal AJ, Brunt EM, Kleiner DE, et al. Endpoints and clinical trial design for nonalcoholic steatohepatitis. Hepatology 2011; 54: 344-53.
DOI PMID |
| 20. |
Brunt EM. Nonalcoholic steatohepatitis. Semin Liver Dis 2004; 24: 3-20.
DOI PMID |
| 21. |
Vali Y, Lee J, Boursier J, et al. Biomarkers for staging fibrosis and non-alcoholic steatohepatitis in non-alcoholic fatty liver disease (the LITMUS project): a comparative diagnostic accuracy study. Lancet Gastroenterol Hepatol 2023; 8: 714-25.
DOI URL |
| 22. |
Harrison SA, Ratziu V, Boursier J, et al. A blood-based biomarker panel (NIS4) for non-invasive diagnosis of non-alcoholic steatohepatitis and liver fibrosis: a prospective derivation and global validation study. Lancet Gastroenterol Hepatol 2020; 5: 970-85.
DOI URL |
| 23. |
Pavlides M, Mózes FE, Akhtar S, et al. Liver Investigation: Testing Marker Utility in Steatohepatitis (LITMUS): assessment & validation of imaging modality performance across the NAFLD spectrum in a prospectively recruited cohort study (the LITMUS imaging study): study protocol. Contemp Clin Trials 2023; 134: 107352.
DOI URL |
| 24. |
Wong VW, Chu WC, Wong GL, et al. Prevalence of non-alcoholic fatty liver disease and advanced fibrosis in Hong Kong Chinese: a population study using proton-magnetic resonance spectroscopy and transient elastography. Gut 2012; 61: 409-15.
DOI PMID |
| 25. |
Tamaki N, Ajmera V, Loomba R. Non-invasive methods for imaging hepatic steatosis and their clinical importance in NAFLD. Nat Rev Endocrinol 2022; 18: 55-66.
DOI |
| 26. |
Castera L, Friedrich-Rust M, Loomba R. Noninvasive assessment of liver disease in patients with nonalcoholic fatty liver disease. Gastroenterology 2019; 156: 1264-81.e1264.
DOI PMID |
| 27. |
Friedman SL, Neuschwander-Tetri BA, Rinella M, Sanyal AJ. Mechanisms of NAFLD development and therapeutic strategies. Nature Medicine 2018; 24: 908-22.
DOI PMID |
| 28. |
Stefan N, Schick F, Birkenfeld AL, Häring HU, White MF. The role of hepatokines in NAFLD. Cell Metab 2023; 35: 236-52.
DOI PMID |
| 29. |
Pal D, Dasgupta S, Kundu R, et al. Fetuin-A acts as an endogenous ligand of TLR4 to promote lipid-induced insulin resistance. Nat Med 2012; 18: 1279-85.
DOI PMID |
| 30. |
Conklin D, Gilbertson D, Taft DW, et al. Identification of a mammalian angiopoietin-related protein expressed specifically in liver. Genomics 1999; 62: 477-82.
DOI PMID |
| 31. |
Geng L, Lam KSL, Xu A. The therapeutic potential of FGF 21 in metabolic diseases: from bench to clinic. Nat Rev Endocrinol 2020; 16: 654-67.
DOI |
| 32. |
Selva DM, Hogeveen KN, Innis SM, Hammond GL. Monosaccharide-induced lipogenesis regulates the human hepatic sex hormone-binding globulin gene. J Clin Invest 2007; 117: 3979-87.
DOI PMID |
| 33. |
Misu H, Takamura T, Takayama H, et al. A liver-derived secretory protein, selenoprotein P, causes insulin resistance. Cell Metab 2010; 12: 483-95.
DOI PMID |
| 34. |
Ye D, Wang Y, Li H, et al. Fibroblast growth factor 21 protects against acetaminophen-induced hepatotoxicity by potentiating peroxisome proliferator-activated receptor coactivator protein-1α-mediated antioxidant capacity in mice. Hepatology 2014; 60: 977-89.
DOI PMID |
| 35. |
Pan X, Shao Y, Wu F, et al. FGF 21 Prevents angiotensin Ⅱ-induced hypertension and vascular dysfunction by activation of ACE2/angiotensin-(1-7) axis in mice. Cell Metab 2018; 27: 1323-37.e1325.
DOI URL |
| 36. | Tilg H, Ianiro G, Gasbarrini A, et al. Adipokines: masterminds of metabolic inflammation. Nat Rev Immunol 2025; 25: 250-65. |
| 37. |
Zhao S, Kusminski CM, Scherer PE. Adiponectin, leptin and cardiovascular disorders. Circ Res 2021; 128: 136-49.
DOI PMID |
| 38. |
He C, Liao Q, Fu P, et al. Microbiological characteristics of different tongue coatings in adults. BMC Microbiol 2022; 22: 214.
DOI PMID |
| 39. |
Yang C, Gai X, Zheng YX, et al. Study on tongue coating microbes of bitter taste, sticky and greasy taste in chronic atrophic gastritis. J Tradit Chin Med 2023; 43: 160-7.
DOI |
| 40. |
Ferguson D, Finck BN. Emerging therapeutic approaches for the treatment of NAFLD and type 2 diabetes mellitus. Nat Rev Endocrinol 2021; 17: 484-95.
DOI PMID |
| 41. |
Yuan L, Yang L, Zhang S, et al. Development of a tongue image-based machine learning tool for the diagnosis of gastric cancer: a prospective multicentre clinical cohort study. EClinicalMedicine 2023; 57: 101834.
DOI URL |
| 42. |
Chen Y, Yin M, Fan L, et al. Mirror-like tongue is an important predictor of acute heart failure: a cohort study of acute heart failure in Chinese patients. J Tradit Chin Med 2023; 43: 1243-51.
DOI |
| 43. |
Liu Y, Fan L, Zhao M, et al. Study on a Traditional Chinese Medicine constitution recognition model using tongue image characteristics and deep learning: a prospective dual-center investigation. Chin Med 2025; 20: 84.
DOI |
| [1] | YUAN Menghua, SHAO Jianbin, YANG Yawei, ZHAO Yan, HU Xingang. Combined acupuncture and herb treatment improves intestinal flora inabdominally obese subjects based on 16s rRNA sequencing: a randomized controlled trial [J]. Journal of Traditional Chinese Medicine, 2026, 46(1): 205-210. |
| [2] | LI Dongqi, WANG Tongxing, WANG Zixuan, YAN Yihui, LI Jie, GU Jiaojiao, LI Cuiru, WANG Aili, SUN Lingling, MENG Yongjie, ZHANG Zeyu, HOU Yunlong, GAO Huailin. Improving glucose tolerance in obese rats: the role of Jinlida granules (津力达颗粒 ) in gut microbiota modulation [J]. Journal of Traditional Chinese Medicine, 2026, 46(1): 62-72. |
| [3] | CHOI You Yeon, JIN Seong chul, KIM Mi Hye, BAEK Hee Kyung, KIM Dong Hyun, OH Sung Hyuk, YANG Woong Mo. Exploring the therapeutic potential of Morus alba Linne extract in targeting localized adiposity [J]. Journal of Traditional Chinese Medicine, 2025, 45(5): 970-978. |
| [4] | YE Wujie, YANG Yawei, ZHANG Da, TANG Ling, CUI Minying, FU Bin, ZHANG Meng, HU Xingang, ZHAO Yan. Effectiveness of combining Qingyanyin formulated granules (轻燕饮配方颗粒) with press needles in treating abdominal obesity: a multicenter randomized controlled trial [J]. Journal of Traditional Chinese Medicine, 2025, 45(1): 107-114. |
| [5] | ZHU Linghui, SUN Ziwei, GUAN Yuanyuan, LIU Meiyi, ZHENG Yi, YU Ruoxi, WANG Qi, LI Lingru. Differences in vascular endothelial function and serum proteome between obese people with phlegm-dampness constitution and balanced constitution [J]. Journal of Traditional Chinese Medicine, 2024, 44(1): 188-196. |
| [6] | QIN Xihui, PANG Jianli, XIONG Guan, FENG Jie. Bo′s abdominal acupuncture improves disordered metabolism in obese type 2 diabetic rats through regulating fibroblast growth factor 21 and its related adipokines [J]. Journal of Traditional Chinese Medicine, 2023, 43(6): 1200-1208. |
| [7] | ZHAO HuiYan, JUN Purumea, LEE Chaewon, HAN Chang-Hyun. Acupoint catgut embedding for simple obesity in animal studies: a systematic review and Meta-analysis [J]. Journal of Traditional Chinese Medicine, 2023, 43(5): 860-867. |
| [8] | ZHANG Xinghe, LI Qifu, YI Rong, XING Chonghui, JIN Yuhao, MENG Jiangqiong, FENG Jialei, ZHAO Siwen, LIANG Fanrong, GUO Taipin. Effect of catgut embedding at acupoints versus non-acupoints in abdominal obesity: a randomized clinical trial [J]. Journal of Traditional Chinese Medicine, 2023, 43(4): 780-786. |
| [9] | YE Wujie, XING Jingyu, YU Zekai, HU Xingang, ZHAO Yan. Systematic review and Meta-analysis of acupuncture and acupoint catgut embedding for the treatment of abdominal obesity [J]. Journal of Traditional Chinese Medicine, 2022, 42(6): 848-857. |
| [10] | WEI Jiali, LAI Lily, LIN Zhechao, LIU Jianping, HAN Mei. Acupoint catgut embedding versus acupuncture for simple obesity: a systematic review and Meta-analysis of randomized controlled trials [J]. Journal of Traditional Chinese Medicine, 2022, 42(6): 839-847. |
| [11] | YAN Shixing, Lü Yi, LIU Ziqing, REN Meng, HE Haiyang, XIAO Li, GUO Feng, PENG Miao, LI Xiaoxia, WANG Yong, XU Xi, YANG Tao, SHAO Zuoyu, HUANG Jingjing, XIAO Mingzhong. Mining intrinsic information of convalescent patients after suffering coronavirus disease 2019 in Wuhan [J]. Journal of Traditional Chinese Medicine, 2022, 42(2): 279-288. |
| [12] | Lakkana Rerksuppaphol, Sanguansak Rerksuppaphol. Efficacy of short duration versus conventional electroacupuncture in the treatment of obesity: a randomized crossover study [J]. Journal of Traditional Chinese Medicine, 2022, 42(2): 256-263. |
| [13] | Se-Eun Lee, Hyungwoo Kim, Chang-Hyun Kim, Chiyeon Lim, Suin Cho. Effect of methanol extract of Schisandrae Fructus on high fat diet induced hyperlipidemic mice [J]. Journal of Traditional Chinese Medicine, 2019, 39(06): 818-825. |
| [14] | Ma Yinlu, Yang Xue, Zhu Cuihong, Cao Rui, Wu Xiongzhi. Lingual flange protrusion: diagnostic marker for metastatic liver cancer [J]. Journal of Traditional Chinese Medicine, 2017, 37(06): 782-788. |
| [15] | Frida Leonetti, Aldo Liguori, Filomena Petti, Susanna Rughini, Laura Silli, Stefano Liguori, Sergio Bangrazi. Effects of basic traditional Chinese diet on body mass index,lean body mass,and eating and hunger behaviours in overweight or obese individuals [J]. Journal of Traditional Chinese Medicine, 2016, 36(04): 456-463. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||

