Journal of Traditional Chinese Medicine ›› 2024, Vol. 44 ›› Issue (1): 44-53.DOI: 10.19852/j.cnki.jtcm.20231204.004
• Original articles • Previous Articles Next Articles
Neferine inhibits the progression of diabetic nephropathy by modulating the miR-17-5p/nuclear factor E2-related factor 2 axis
HUANG Hongmei1, YANG Maojun1, LI Ting1, WANG Dandan1, LI Ying1, TANG Xiaochi1, YUAN Lu1, GU Shi1, XU Yong2( )
)
- 1 Department of Endocrinology, Chengdu Shuangliu District First People's Hospital (West China Airport of Sichuan University), Chengdu 610200, China
2 Department of Endocrinology, Affiliated Hospital of Southwest Medical University, Luzhou 646000, China
-
Received:2023-12-12Accepted:2023-03-17Online:2024-02-15Published:2023-12-04 -
Contact:Prof. XU Yong, Department of Endocrinology, Affiliated Hospital of Southwest Medical University, Luzhou 646000, China. zzh1911@sina.com. Telephone: +86-15928418055 -
Supported by:Chengdu Health and Wellness Commission: Exploring the Mechanism of Neferine on Diabetic Nephropathy Based on miR-17/Nrf2 Axis(2021127)
Cite this article
HUANG Hongmei, YANG Maojun, LI Ting, WANG Dandan, LI Ying, TANG Xiaochi, YUAN Lu, GU Shi, XU Yong. Neferine inhibits the progression of diabetic nephropathy by modulating the miR-17-5p/nuclear factor E2-related factor 2 axis[J]. Journal of Traditional Chinese Medicine, 2024, 44(1): 44-53.
share this article
| Group | n | BG (mmol/L) | Crea (μmol/L) | UREA (mmol/L) | ALB (g/L) |
|---|---|---|---|---|---|
| Control | 7 | 7.5±0.6 | 56.1±24.0 | 5.4±1.4 | 30.0±3.0 |
| DN | 7 | 22.2±0.4a | 159.5±24.0a | 18.6±3.2a | 51.3±7.3a |
| DN+RSG | 7 | 13.0±0.7b | 99.7±13.1b | 10.8±1.2b | 35.6±3.9b |
| DN+Nef-L | 7 | 17.2±0.6b | 135.3±19.8 | 16.3±1.2 | 49.8±5.5 |
| DN+Nef-M | 7 | 13.9±1.1b | 111.1±14.1b | 11.2±2.4b | 42.6±4.4 |
| DN+Nef-H | 7 | 11.5±1.1b | 89.2±10.3bc | 9.1±1.4bc | 33.5±3.6b |
Table 1 Blood biochemistry and blood glucose of each group of mice ($\bar{x}±s$)
| Group | n | BG (mmol/L) | Crea (μmol/L) | UREA (mmol/L) | ALB (g/L) |
|---|---|---|---|---|---|
| Control | 7 | 7.5±0.6 | 56.1±24.0 | 5.4±1.4 | 30.0±3.0 |
| DN | 7 | 22.2±0.4a | 159.5±24.0a | 18.6±3.2a | 51.3±7.3a |
| DN+RSG | 7 | 13.0±0.7b | 99.7±13.1b | 10.8±1.2b | 35.6±3.9b |
| DN+Nef-L | 7 | 17.2±0.6b | 135.3±19.8 | 16.3±1.2 | 49.8±5.5 |
| DN+Nef-M | 7 | 13.9±1.1b | 111.1±14.1b | 11.2±2.4b | 42.6±4.4 |
| DN+Nef-H | 7 | 11.5±1.1b | 89.2±10.3bc | 9.1±1.4bc | 33.5±3.6b |

Figure 1 Effect of Nef on the kidney histopathology in mice with DN A: HE staining of kidney tissue (scale bar, 200 μm and 50 μm); A1: control group (×100); A2: DN group (×100); A3: DN + RSG group (×100); A4: control group (×400); A5: DN group (×400); A6: DN + RSG group (×400); A7: DN-Nef-L group (×100); A8: DN-Nef-M group (×100); A9: DN-Nef-H group (×100); A10: DN-Nef-L group (×400); A11: DN-Nef-M group (×400); A12: DN-Nef-H group (×400). B: Masson staining of kidney tissue (×400, scale bar, 50 μm); B1: control group; B2: DN group; B3: DN + RSG group; B4: DN-Nef-L group; B5: DN-Nef-M group; B6: DN-Nef-H group. C: percentage of positive collagen fiber area (%); D: kidney weight index of the mice. DN: diabetic nephropathy; HE: hematoxylin and eosin; RSG: rosiglitazone (4 mg/kg); Nef-L: neferine low dose (60 mg/kg); Nef-M: neferine medium dose (120 mg/kg); Nef-H: neferine high dose (240 mg/kg). Data were statistically analyzed by least significant difference. Data were expressed as mean ± standard deviation (n =3). aP < 0.05, compared with the control group; bP < 0.05, compared with the DN group; cP < 0.05, compared with the DN + RSG group.
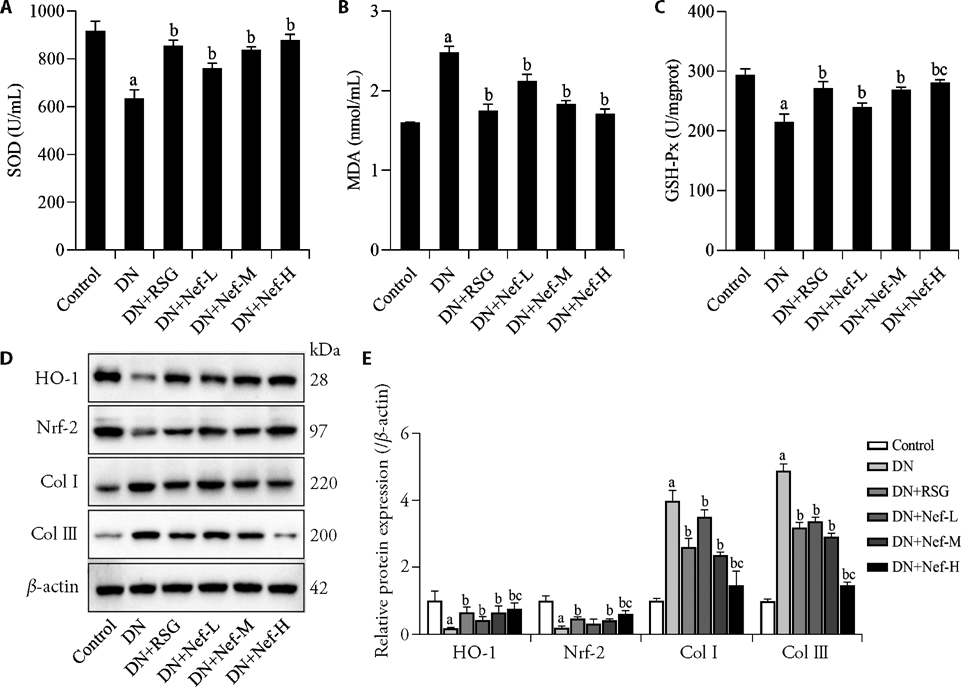
Figure 2 Effect of Nef on renal oxidative stress indicators in mice with DN A: levels of SOD in the kidney tissues of mice. B: levels of MDA in the kidney tissues of mice. C: levels of GSH-Px in the kidney tissues of mice. D: representative blot images of HO-1, Nrf2, Col I, and Col III measured by western blot. E: protein expression of HO-1, Nrf2, Col I, and Col III in the kidney tissues of mice was detected by Western blotting. DN: diabetic nephropathy; RSG: rosiglitazone (4 mg/kg); Nef-L: neferine low dose (60 mg/kg); Nef-M: neferine medium dose (120 mg/kg); Nef-H: neferine high dose (240 mg/kg); SOD: superoxide dismutase; MDA: malondialdehyde; GSH-Px: glutathione peroxidase; HO-1: heme oxygenase 1; Nrf2: nuclear factor E2-related factor 2; Col I: collagen I; Col III: collagen III. Data were statistically analyzed by least significant difference-t. Data were expressed as mean ± standard deviation (n = 3). aP < 0.05, compared with the control group, bP < 0.05, compared with the DN group, cP < 0.05, compared with the DN + RSG group.
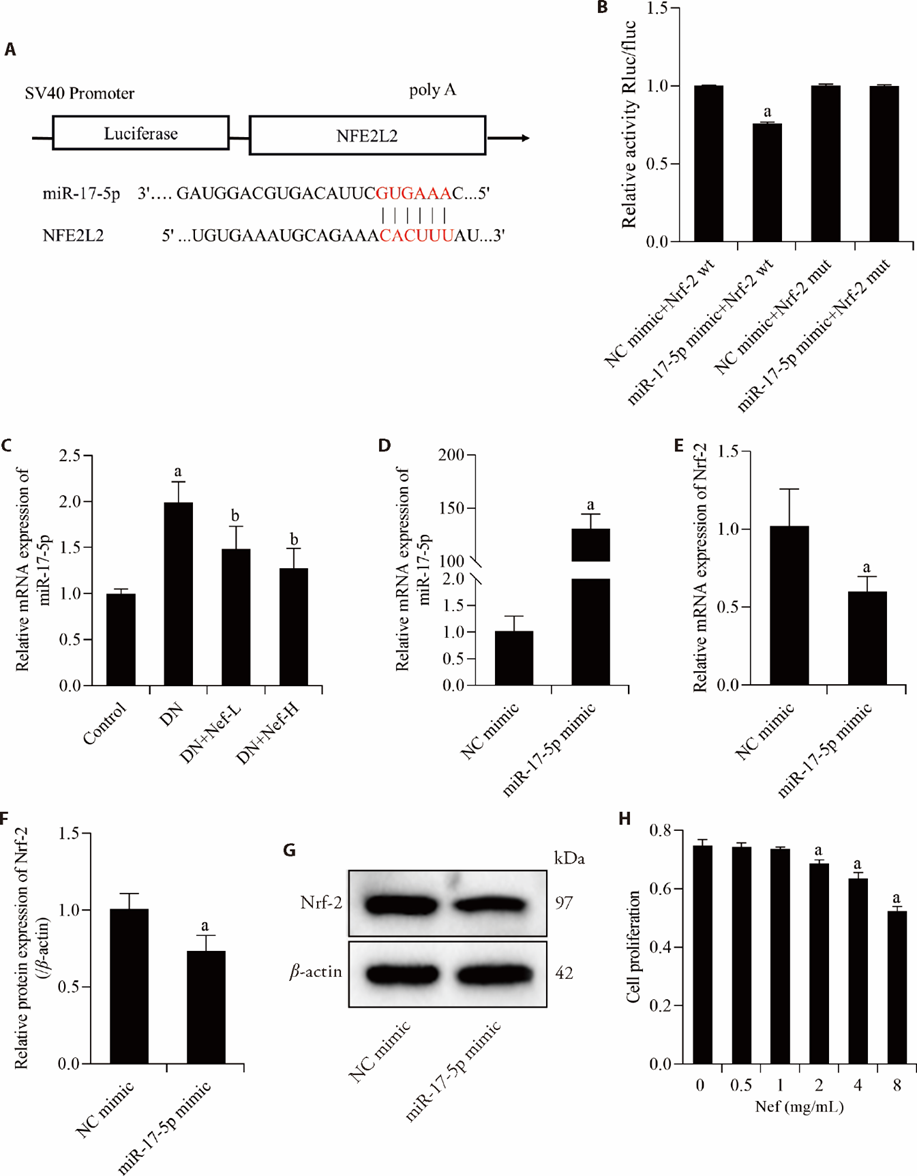
Figure 3 Targeting relationship between Nrf2 and miR-17-5p and the effect of Nef on renal miR-17-5p expression in the mice with DN A: TargetScan (http://www.targetscan.org) prediction showing potential miR-17-5p binding sites for the Nrf2 3'-UTR, complementary pairing of target genes is indicated in red. B: miR-17-5p target sequences were fused with a luciferase reporter and transfected with miR-17-5p mimic or NC mimic into HEK-293T cells, and miR-17-5p significantly restrained the luciferase activity of the Nrf2 3'-UTR. C: mRNA level of miR-17-5p in the kidney tissues of mice. D: mRNA levels of miR-17-5p in HMCs. E: mRNA levels of Nrf2 in HMCs. F: protein expression of Nrf2 in HMCs. G: representative blot images of Nrf2. H: detection of the proliferation of HMCs treated with different concentrations of Nef. The data in qRT-PCR analysis were expressed after normalization to U6 or β-actin, while those in Western blot assays were expressed after normalization to β-actin. DN: diabetic nephropathy; Nef-L: neferine low dose (60 mg/kg); Nef-H: neferine high dose (240 mg/kg). Nrf2: nuclear factor E2-related factor 2. NC: negative control; HMCs: human mesangial cells; qRT-PCR: quantitative reverse transcription-polymerase chain reaction. Data were statistically analyzed by least significant difference-t. Data were expressed as mean ± standard deviation (n = 3). aP < 0.05, compared with the control or NC mimic group; bP < 0.05, compared with the DN group.
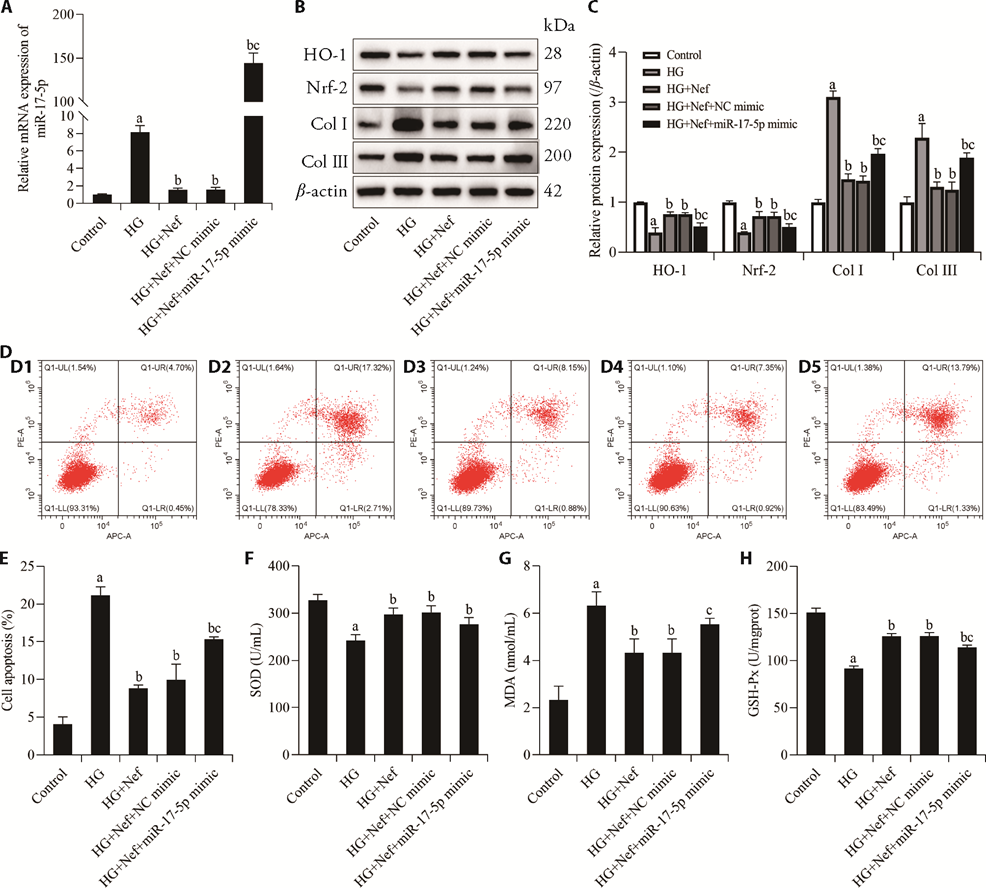
Figure 4 Effect of Nef-mediated miR-17-5p on oxidative stress injury in high glucose-induced HMCs A: mRNA level of miR-17-5p in HMCs; B: representative blot images of HO-1, Nrf2, Col Ⅰ, and Col Ⅲ; C: protein expression of HO-1, Nrf2, Col Ⅰ, and Col Ⅲ in HMCs; D: detection of cell apoptosis using flow cytometry; D1: control group; D2: HG group; D3: HG + Nef group; D4: HG + Nef + NC mimic group; D5: HG + Nef + miR-17-5p mimic group; E: cell apoptosis; F: levels of SOD in HMCs; G: levels of MDA in HMCs; H: levels of GSH-Px in HMCs. HG: high glucose (25 mmol/L). HG + Nef: high glucose (25 mmol/L) + Nef (1 mg/mL). HG+Nef+NC mimic: high glucose (25 mmol/L) + Nef (1 mg/mL) + NC mimic. HG + Nef + miR-17-5p mimic: high glucose (25 mmol/L) + Nef (1 mg/mL) + miR-17-5p mimic. The data from the qRT-PCR analysis were normalized with U6, while those from Western blot assays were normalized with β-actin. HG: high glucose; Nef: neferine; HO-1: heme oxygenase 1; Nrf2: nuclear factor E2-related factor 2; ColⅠ: collagenⅠ; Col Ⅲ: collagen Ⅲ; SOD: superoxide dismutase; MDA: malondialdehyde; GSH-Px: glutathione peroxidase; HMCs: human mesangial cells; NC: negative control; qRT-PCR: quantitative reverse transcription-polymerase chain reaction. Data were statistically analyzed by least significant difference-t. Data were expressed as mean ± standard deviation (n = 3). aP < 0.05, compared with the control group; bP < 0.05, compared with the HG group; cP < 0.05, compared with the HG + Nef group.
| 1. | Samsu N. Diabetic nephropathy: challenges in pathogenesis, diagnosis, and treatment. Biomed Res Int 2021; 2021: 1497449. |
| 2. |
Dai X, Liao R, Liu C, et al. Epigenetic regulation of TXNIP-mediated oxidative stress and NLRP 3 inflammasome activation contributes to SAHH inhibition-aggravated diabetic nephropathy. Redox Biol 2021; 45: 102033.
DOI URL |
| 3. |
Gerardo Yanowsky-Escatell F, Andrade-Sierra J, Pazarín-Villaseñor L, et al. The role of dietary antioxidants on oxidative stress in diabetic nephropathy. Iran J Kidney Dis 2020; 14: 81-94.
PMID |
| 4. |
Sagoo MK, Gnudi L. Diabetic nephropathy: is there a role for oxidative stress? Free Radic Biol Med 2018; 116: 50-63.
DOI URL |
| 5. |
Tang YS, Zhao YH, Zhong Y, et al. Neferine inhibits LPS-ATP-induced endothelial cell pyroptosis via regulation of ROS/NLRP3/Caspase-1 signaling pathway. Inflamm Res 2019; 68: 727-38.
DOI |
| 6. | Bharathi Priya L, Huang CY. An updated review on pharmacological properties of neferine-A bisbenzylisoquinoline alkaloid from Nelumbo nucifera. J Food Biochem 2021; 45: e13986. |
| 7. | Wang Y, Wang S, Wang R, et al. Neferine exerts antioxidant and anti-inflammatory effects on carbon tetrachloride-induced liver fibrosis by inhibiting the MAPK and NF-κB/IκBα pathways. Evid Based Complement Alternat Med 2021; 2021: 4136019. |
| 8. | Li S, Zhang Y, Zhang J, et al. Neferine exerts ferroptosis-inducing effect and antitumor effect on thyroid cancer through Nrf2/HO-1/NQO1 inhibition. J Oncol 2022; 2022: 7933775. |
| 9. | Liu Y, Wang J, Zhang X, Wang L, Hao T, Cheng Y. Scutellarin exerts hypoglycemic and renal protective effects in db/db mice via the Nrf2/HO-1 signaling pathway. Oxid Med Cell Longev 2019; 2019: 1354345. |
| 10. |
Xing L, Guo H, Meng S, et al. Klotho ameliorates diabetic nephropathy by activating Nrf2 signaling pathway in podocytes. Biochem Biophys Res Commun 2021; 534: 450-56.
DOI URL |
| 11. | He M, Wang J, Yin Z, et al. MiR-320a induces diabetic nephropathy via inhibiting MafB. Aging (Albany NY) 2019; 11: 3055-79. |
| 12. |
Guo Y, Du F, Tan YL, Luo J, Xiong D, Song WT. VEGF-mediated angiogenesis in retinopathy of prematurity is co-regulated by miR-17-5p and miR-20a-5p. Biochem Cell Biol 2021; 99: 414-23.
DOI URL |
| 13. |
Wei J, Hao Q, Chen C, et al. Epigenetic repression of miR-17 contributed to di (2-ethylhexyl) phthalate-triggered insulin resistance by targeting Keap1-Nrf2/miR-200a axis in skeletal muscle. Theranostics 2020; 10: 9230-48.
DOI URL |
| 14. |
Du KY, Qadir J, Yang BB, Yee AJ, Yang W. Tracking miR-17-5p levels following expression of seven reported target mRNAs. Cancers (Basel) 2022; 14: 2585.
DOI URL |
| 15. |
Cai TT, Ye XL, Li RR, et al. Resveratrol modulates the gut microbiota and inflammation to protect against diabetic nephropathy in mice. Front Pharmacol 2020; 11: 1249.
DOI URL |
| 16. |
Wu F, Ji A, Zhang Z, Li J, Li P. miR-491-5p inhibits the proliferation and migration of A549 cells by FOXP4. Exp Ther Med 2021; 21: 622.
DOI PMID |
| 17. |
Duan YR, Chen BP, Chen F, et al. LncRNA lnc-ISG20 promotes renal fibrosis in diabetic nephropathy by inducing AKT phosphorylation through miR-486-5p/NFAT5. J Cell Mol Med 2021; 25: 4922-37.
DOI URL |
| 18. |
Shen Y, Chen W, Han L, et al. VEGF-B antibody and interleukin-22 fusion protein ameliorates diabetic nephropathy through inhibiting lipid accumulation and inflammatory responses. Acta Pharm Sin B 2021; 11: 127-42.
DOI PMID |
| 19. |
Lee SY, An HJ, Kim JM, et al. PINK1 deficiency impairs osteoblast differentiation through aberrant mitochondrial homeostasis. Stem Cell Res Ther 2021; 12: 589.
DOI |
| 20. |
Ma H, Bell KN, Loker RN. qPCR and qRT-PCR analysis: Regulatory points to consider when conducting biodistribution and vector shedding studies. Mol Ther Methods Clin Dev 2021; 20: 152-68.
DOI URL |
| 21. |
Pillai-Kastoori L, Schutz-Geschwender AR, Harford JA. A systematic approach to quantitative Western blot analysis. Anal Biochem 2020; 593: 113608.
DOI URL |
| 22. |
Xian Y, Gao Y, Lü W, et al. Resveratrol prevents diabetic nephropathy by reducing chronic inflammation and improving the blood glucose memory effect in non-obese diabetic mice. Naunyn Schmiedebergs Arch Pharmacol 2020; 393: 2009-17.
DOI |
| 23. |
Zheng C, Huang L, Luo W, et al. Inhibition of STAT3 in tubular epithelial cells prevents kidney fibrosis and nephropathy in STZ-induced diabetic mice. Cell Death Dis 2019; 10: 848.
DOI PMID |
| 24. |
Bai L, Li A, Gong C, Ning X, Wang Z. Protective effect of rutin against bleomycin induced lung fibrosis: involvement of TGF-β1/α-SMA/Col Ⅰ and Ⅲ pathway. Biofactors 2020; 46: 637-44.
DOI URL |
| 25. | Huang W, Man Y. Short-chain fatty acids ameliorate diabetic nephropathy via GPR43-mediated inhibition of oxidative stress and NF-κB signaling. Oxid Med Cell Longev 2020; 2020: 4074832. |
| 26. |
Qiao S, Liu R, Lv C, et al. Bergenin impedes the generation of extracellular matrix in glomerular mesangial cells and ameliorates diabetic nephropathy in mice by inhibiting oxidative stress via the mTOR/β-TrcP/Nrf2 pathway. Free Radic Biol Med 2019; 145: 118-35.
DOI URL |
| 27. |
Bellezza I, Giambanco I, Minelli A, Donato R. Nrf2-Keap1 signaling in oxidative and reductive stress. Biochim Biophys Acta Mol Cell Res 2018; 1865: 721-33.
DOI URL |
| 28. |
Zhang H, Qi S, Song Y, Ling C. Artemisinin attenuates early renal damage on diabetic nephropathy rats through suppressing TGF-β1 regulator and activating the Nrf2 signaling pathway. Life Sci 2020; 256: 117966.
DOI URL |
| 29. |
Conti I, Varano G, Simioni C, et al. miRNAs as influencers of cell-cell communication in tumor microenvironment. Cells 2020; 9: 220.
DOI URL |
| 30. | Shen Y, Tong ZW, Zhou Y, et al. Inhibition of lncRNA-PAX8-AS1-N directly associated with VEGF/TGF-β1/8-OhdG enhances podocyte apoptosis in diabetic nephropathy. Eur Rev Med Pharmacol Sci 2020; 24: 6864-72. |
| 31. | Dong H, Qiang Z, Chai D, et al. Nrf2 inhibits ferroptosis and protects against acute lung injury due to intestinal ischemia reperfusion via regulating SLC7A11 and HO-1. Aging (Albany NY) 2020; 12: 12943-59. |
| [1] | ZHANG Xiaoying, WANG Ruixuan, WANG Yiqing, XU Fanxing, YAN Tingxu, WU Bo, ZHANG Ming, JIA Ying. Spinosin protects Neuro-2a/APP695 cells from oxidative stress damage by inactivating p38 [J]. Journal of Traditional Chinese Medicine, 2023, 43(5): 868-875. |
| [2] | LIU Bingbing, LI Jieru, SI Jianchao, CHEN Qi, YANG Shengchang, JI Ensheng. Ginsenoside Rb1 alleviates chronic intermittent hypoxia-induced diabetic cardiomyopathy in db/db mice by regulating the adenosine monophosphate-activated protein kinase/Nrf2/heme oxygenase-1 signaling pathway [J]. Journal of Traditional Chinese Medicine, 2023, 43(5): 906-914. |
| [3] | ZHOU Hua, LI Hui, WANG Haihua. Potential protective effects of the water-soluble Chinese propolis on experimental ulcerative colitis [J]. Journal of Traditional Chinese Medicine, 2023, 43(5): 925-933. |
| [4] | QU Yilun, CHENG Haimei, WANG Qian, LI Shuang, DUAN Shuwei, FENG Zhe, LI Weizhen, JIANG Shuangshuang, YANG Hongtao, MAO Yonghui, GENG Yanqiu, LI Jijun, LIU Yuning, TIAN Jinzhou, LIU Hongfang, DONG Zheyi, CHEN Xiangmei. Noninvasive identificational diagnosis of diabetic nephropathy and non-diabetic renal disease based on clinical characteristics of Traditional Chinese Medicine symptom pattern and conventional medicine [J]. Journal of Traditional Chinese Medicine, 2023, 43(3): 588-593. |
| [5] | XIE Jing, BI Zheng, WANG Sihai, SHEN Guoming, FANG Zhaohui. Danzhi Jiangtang capsule (丹蛭降糖胶囊) reduces renal injury in rats with diabetes induced by high fat diet and streptozotocin via downregulating toll-like receptor 4-nuclear factor-κB pathway and apoptosis [J]. Journal of Traditional Chinese Medicine, 2023, 43(2): 312-321. |
| [6] | ZHENG Wei, WANG Mingxing, LIU Shanxue, LUAN Chao, ZHANG Yanqiu, XU Duoduo, WANG Jian. Buyang Huanwu Tang (补阳还五汤) protects H2O2-induced RGC-5 cell against oxidative stress and apoptosis via reactive oxygen species-mitogen-activated protein kinase signaling pathway [J]. Journal of Traditional Chinese Medicine, 2022, 42(6): 885-891. |
| [7] | HENG Xianpei, LI Liang, YANG Liuqin, WANG Zhita. Efficacy of Dangua Fang (丹瓜方) on endothelial cells damaged by oxidative stress [J]. Journal of Traditional Chinese Medicine, 2022, 42(6): 900-907. |
| [8] | HUANG Qiuyue, YE Hui, SHI Zongming, JIA Xiaofen, LIN Miaomiao, CHU Yingming, YU Jing, ZHANG Xuezhi. Efficacy of Qingre Huashi decoction (清热化湿方) on infection of Helicobacter pylori: inhibiting adhesion, antioxidant, and anti-inflammation [J]. Journal of Traditional Chinese Medicine, 2022, 42(6): 915-921. |
| [9] | XU Baogui, ZHENG Jiawen, TIAN Xiaoxiao, YUAN Falei, LIU Zhongliang, YANG Zuisu, DING Xianjun. Antihepatofibrotic effect of Guizhifuling pill (桂枝茯苓丸) on carbon tetrachloride-induced liver fibrosis in mice [J]. Journal of Traditional Chinese Medicine, 2022, 42(5): 715-722. |
| [10] | Xing DU, Tianlong LIU, Wendi TAO, Maoxing LI, Xiaolin LI, Lan YAN. Effect of aqueous extract of Astragalus membranaceus on behavioral cognition of rats living at high altitude [J]. Journal of Traditional Chinese Medicine, 2022, 42(1): 58-64. |
| [11] | GUO Yangzhi, DU Juan, JIANG Min, GUO Wei. Full composition granules of Huanglian (Rhizoma Coptidis) decrease the serum monocyte chemotactic protein-1 and connective tissue growth factor levels and inhibit kidney nuclear factor-κB expression in rats with high-fat diet-induced diabetes [J]. Journal of Traditional Chinese Medicine, 2021, 41(3): 424-431. |
| [12] | CAI Liang, ZONG Daokuan, TONG Guoqing, LI Li. Apoptotic mechanism of premature ovarian failure and rescue effect of Traditional Chinese Medicine: a review [J]. Journal of Traditional Chinese Medicine, 2021, 41(3): 491-498. |
| [13] | LIU Chunhua, LU Dingyan, YOU Jingrui, LU Yuan, SUN Jia, PAN Jie, WANG Yonglin, WANG Aimin, LAN Yanyu, LI Yongjun, LIU Ting. Efficacy of water fraction from Dioscorea cirrhosa on oxidative stress and apoptosis in H9c2 cardiomyocytes induced by H_2O_2 [J]. Journal of Traditional Chinese Medicine, 2021, 41(1): 51-58. |
| [14] | LIU Huahua, ZHAO Jingjing, PAN Sunlei, ZHU Yeke, FU Guosheng, TANG Weiliang, PENG Fang. Shexiang Tongxin dropping pill(麝香通心滴丸) protects against sodium laurate-induced coronary microcirculatory dysfunction in rats [J]. Journal of Traditional Chinese Medicine, 2021, 41(1): 89-97. |
| [15] | CHEN Xiaoqing, ZHANG Yong, HUANG Chunlai, FU Tingting, TAO Qinghua, MA Liqiang, WANG Liping. Efficacy of Huanglian root decoction(黄连煎剂) on kidney injury in rat's model of metabolic syndrome [J]. Journal of Traditional Chinese Medicine, 2021, 41(1): 117-124. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||

