Journal of Traditional Chinese Medicine ›› 2022, Vol. 42 ›› Issue (5): 715-722.DOI: 10.19852/j.cnki.jtcm.20220707.003
• Research Articles • Previous Articles Next Articles
Antihepatofibrotic effect of Guizhifuling pill (桂枝茯苓丸) on carbon tetrachloride-induced liver fibrosis in mice
XU Baogui1, ZHENG Jiawen1, TIAN Xiaoxiao1, YUAN Falei1, LIU Zhongliang2, YANG Zuisu1( ), DING Xianjun3(
), DING Xianjun3( )
)
- 1 School of Food and Pharmacy, Zhejiang Ocean University; Zhejiang Provincial Engineering Technology Research Center of Marine Biomedical Products, Zhoushan 316022, China
2 Department of Oncology, Zhoushan Hospital of Traditional Chinese Medicine, Zhoushan 316000, China
3 Department of Infectious Diseases, Zhoushan Hospital of Traditional Chinese Medicine, Zhoushan 316000, China
-
Received:2021-07-18Accepted:2021-10-11Online:2022-10-15Published:2022-07-07 -
Contact:YANG Zuisu,DING Xianjun -
About author:Dr. DING Xianjun, Department of Infectious Diseases, Zhoushan Hospital of Traditional Chinese Medicine, Zhoushan 316000, China. d.xj@163.com Telephone: +86-580-2260600
Prof. YANG Zuisu, School of Food and Pharmacy, Zhejiang Ocean University; Zhejiang Provincial Engineering Technology Research Center of Marine Biomedical Products, Zhoushan 316022, China. abc1967@126.com;
-
Supported by:Zhejiang Provincial Key Research Project of Traditional Chinese Medicine Science and Technology Plan: Guizhi Fuling Pill Up-regulates MiR-29b-3p and Inhibits CUGBP1-mediated Study on the Mechanism of Liver Fibrosis(2019ZZ017)
Cite this article
XU Baogui, ZHENG Jiawen, TIAN Xiaoxiao, YUAN Falei, LIU Zhongliang, YANG Zuisu, DING Xianjun. Antihepatofibrotic effect of Guizhifuling pill (桂枝茯苓丸) on carbon tetrachloride-induced liver fibrosis in mice[J]. Journal of Traditional Chinese Medicine, 2022, 42(5): 715-722.
share this article
| Time (weeks) | Control | Model | Colchicine | L-GZFL | H-GZFL |
|---|---|---|---|---|---|
| Week 1 | 24.12±0.15 | 23.92±0.13 | 23.77±0.07 | 23.65±0.06 | 23.92±0.24 |
| Week 2 | 29.84±0.34 | 28.65±0.41 | 27.89±0.64 | 28.42±0.55 | 28.32±0.30 |
| Week 3 | 32.07±0.20 | 29.90±0.76 | 30.04±0.83 | 28.96±0.17 | 29.75±0.45 |
| Week 4 | 34.01±0.52 | 29.59±0.56 | 30.05±0.62 | 29.78±1.10 | 29.76±0.64 |
| Week 5 | 34.73±0.70 | 30.98±1.08 | 31.64±1.14 | 31.38±0.71 | 31.07±0.78 |
| Week 6 | 35.32±0.41 | 31.66±0.56 | 32.52±0.98 | 33.27±0.72 | 33.28±1.45 |
| Week 7 | 35.81±0.89 | 32.18±0.40 | 34.28±0.70 | 35.09±0.12 | 34.26±0.97 |
| Week 8 | 37.56±1.07 | 33.35±0.89 | 36.83±0.89 | 36.08±0.23 | 35.25±0.81 |
| Week 9 | 37.84±0.94 | 33.21±0.43 | 35.68±1.09 | 35.80±1.02 | 35.89±0.52 |
Table 1 Changes of body weight in each group (g)
| Time (weeks) | Control | Model | Colchicine | L-GZFL | H-GZFL |
|---|---|---|---|---|---|
| Week 1 | 24.12±0.15 | 23.92±0.13 | 23.77±0.07 | 23.65±0.06 | 23.92±0.24 |
| Week 2 | 29.84±0.34 | 28.65±0.41 | 27.89±0.64 | 28.42±0.55 | 28.32±0.30 |
| Week 3 | 32.07±0.20 | 29.90±0.76 | 30.04±0.83 | 28.96±0.17 | 29.75±0.45 |
| Week 4 | 34.01±0.52 | 29.59±0.56 | 30.05±0.62 | 29.78±1.10 | 29.76±0.64 |
| Week 5 | 34.73±0.70 | 30.98±1.08 | 31.64±1.14 | 31.38±0.71 | 31.07±0.78 |
| Week 6 | 35.32±0.41 | 31.66±0.56 | 32.52±0.98 | 33.27±0.72 | 33.28±1.45 |
| Week 7 | 35.81±0.89 | 32.18±0.40 | 34.28±0.70 | 35.09±0.12 | 34.26±0.97 |
| Week 8 | 37.56±1.07 | 33.35±0.89 | 36.83±0.89 | 36.08±0.23 | 35.25±0.81 |
| Week 9 | 37.84±0.94 | 33.21±0.43 | 35.68±1.09 | 35.80±1.02 | 35.89±0.52 |
| Item | Control | Model | Colchicine | L-GZFL | H-GZFL |
|---|---|---|---|---|---|
| Liver index | 3.793±0.181 | 5.416±0.093a | 4.163±0.216b | 4.220±0.082b | 4.357±0.195ab |
| Hyp (μg/mg) | 0.064±0.003 | 0.329±0.004a | 0.174±0.005ab | 0.179±0.007ab | 0.089±0.004ab |
Table 2 Change in liver index and the expression of hydroxyproline of mice
| Item | Control | Model | Colchicine | L-GZFL | H-GZFL |
|---|---|---|---|---|---|
| Liver index | 3.793±0.181 | 5.416±0.093a | 4.163±0.216b | 4.220±0.082b | 4.357±0.195ab |
| Hyp (μg/mg) | 0.064±0.003 | 0.329±0.004a | 0.174±0.005ab | 0.179±0.007ab | 0.089±0.004ab |

Figure 1 GZFL attenuates CCl4-induced liver injury and fibrosis in mice A: representative livers at the time of sacrifice; B: HE staining of representative liver tissues (B1-B5:original magnification ×100; B6-B10: partially enlarged pictures × 400); C: Masson's trichrome staining of liver sections (C1-C5:original magnification ×100; C6-C10: partially enlarged pictures × 400). Vacuoles (), hepatic sinusoids (), inflammatory cells (), necrotic hepatocytes (), and connective tissue hyperplasia () in the HE staining figure. Control: intraperitoneal injection with normal saline, twice a week for 4 weeks; gavaged with normal saline daily, 4 weeks. Model: intraperitoneal injection with CCl4, twice a week for 4 weeks; gavaged with normal saline daily, 4 weeks. Colchicine: positive group, intraperitoneal injection with CCl4, twice a week for 4 weeks; gavaged with colchicine (0.1 mg/kg) daily, 4 weeks. L-GZFL: intraperitoneal injection with CCl4, twice a week for 4 weeks; gavaged with GZFL (150 mg/kg) daily, 4 weeks. H-GZFL: intraperitoneal injection with CCl4, twice a week for 4 weeks; gavaged with GZFL (300 mg/kg) daily, 4 weeks. GZFL: Guizhifuling pill; CCl4: carbon tetrachloride; HE: hematoxylin and eosin.
| Liver index | Control | Model | Colchicine | L-GZFL | H-GZFL |
|---|---|---|---|---|---|
| ALT (U/L) | 27.05±4.64 | 48.75±3.04a | 34.60±3.88b | 39.23±1.59ab | 43.02±4.02a |
| AST (U/L) | 35.02±5.78 | 59.23±3.26a | 42.23±2.64b | 49.85±4.24a | 55.30±3.59a |
| γ-GT (U/L) | 5.01±0.17 | 6.49±0.33a | 5.13±0.34b | 5.60±0.55 | 5.95±0.31 |
| ALB (g/L) | 70.89±5.04 | 54.02±3.12 | 66.64±5.77 | 62.02±2.14 | 61.24±6.88 |
Table 3 Effect of GZFL on liver indices in mice
| Liver index | Control | Model | Colchicine | L-GZFL | H-GZFL |
|---|---|---|---|---|---|
| ALT (U/L) | 27.05±4.64 | 48.75±3.04a | 34.60±3.88b | 39.23±1.59ab | 43.02±4.02a |
| AST (U/L) | 35.02±5.78 | 59.23±3.26a | 42.23±2.64b | 49.85±4.24a | 55.30±3.59a |
| γ-GT (U/L) | 5.01±0.17 | 6.49±0.33a | 5.13±0.34b | 5.60±0.55 | 5.95±0.31 |
| ALB (g/L) | 70.89±5.04 | 54.02±3.12 | 66.64±5.77 | 62.02±2.14 | 61.24±6.88 |
| Antioxidants marker | Control | Model | Colchicine | L-GZFL | H-GZFL |
|---|---|---|---|---|---|
| MDA | 2.52±0.08 | 3.32±0.16a | 2.66±0.24b | 2.82±0.08ab | 2.95±0.16ab |
| SOD | 208.53±15.13 | 172.36±18.60a | 197.53±11.62 | 194.12±9.82 | 185.82±22.23 |
| GSH-Px | 106.87±2.38 | 79.63±3.43a | 100.95±6.63b | 97.26±5.01b | 99.64±8.16b |
| T-AOC | 6.87±0.42 | 3.45±0.20a | 5.96±0.20b | 4.94±0.53ab | 4.18±0.13a |
| CAT | 6.12±0.63 | 4.40±0.31a | 5.27±0.52 | 5.23±0.30 | 5.20±0.21 |
Table 4 Effect of GZFL on antioxidant capacities and MDA levels in liver tissues
| Antioxidants marker | Control | Model | Colchicine | L-GZFL | H-GZFL |
|---|---|---|---|---|---|
| MDA | 2.52±0.08 | 3.32±0.16a | 2.66±0.24b | 2.82±0.08ab | 2.95±0.16ab |
| SOD | 208.53±15.13 | 172.36±18.60a | 197.53±11.62 | 194.12±9.82 | 185.82±22.23 |
| GSH-Px | 106.87±2.38 | 79.63±3.43a | 100.95±6.63b | 97.26±5.01b | 99.64±8.16b |
| T-AOC | 6.87±0.42 | 3.45±0.20a | 5.96±0.20b | 4.94±0.53ab | 4.18±0.13a |
| CAT | 6.12±0.63 | 4.40±0.31a | 5.27±0.52 | 5.23±0.30 | 5.20±0.21 |
| Proinflammatory cytokine | Control | Model | Colchicine | L-GZFL | H-GZFL |
|---|---|---|---|---|---|
| IL-1β | 36.8±1.1 | 61.7±1.5a | 41.8±1.6b | 49.7±2.5 | 55.8±2.4a |
| IL-6 | 73.7±3.1 | 111.0±1.8a | 84.7±3.4 | 88.8±2.5 | 97.6±2.4 |
| TNF-α | 61.8±3.5 | 98.0±4.0a | 66.0±4.2a | 72.4±2.7a | 81.3±3.9a |
Table 5 Effect of GZFL on the levels of proinflammatory cytokines in liver tissue (pg/mL)
| Proinflammatory cytokine | Control | Model | Colchicine | L-GZFL | H-GZFL |
|---|---|---|---|---|---|
| IL-1β | 36.8±1.1 | 61.7±1.5a | 41.8±1.6b | 49.7±2.5 | 55.8±2.4a |
| IL-6 | 73.7±3.1 | 111.0±1.8a | 84.7±3.4 | 88.8±2.5 | 97.6±2.4 |
| TNF-α | 61.8±3.5 | 98.0±4.0a | 66.0±4.2a | 72.4±2.7a | 81.3±3.9a |
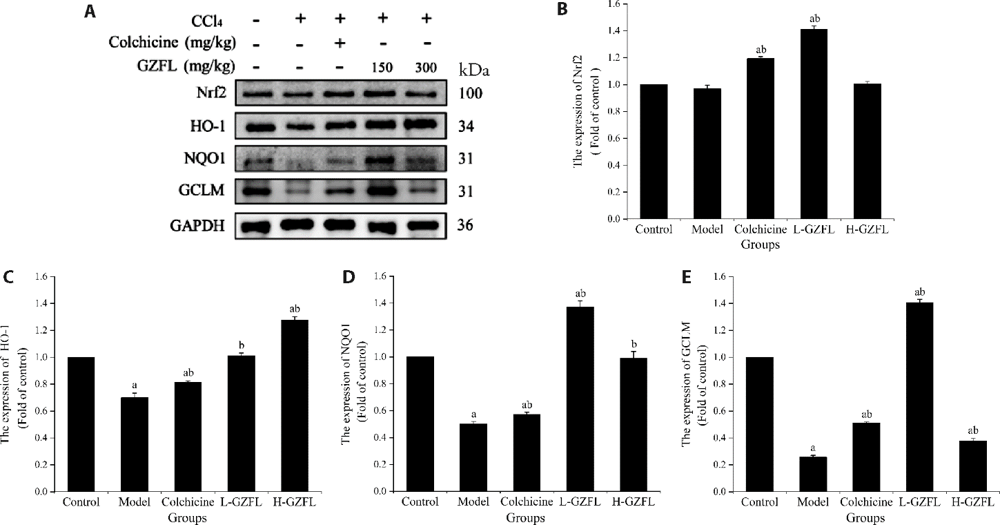
Figure 2 Western blotting to determine the protein expression of Nrf2-mediated antioxidant signaling A: Western blotting to determine the expression of Nrf2, NQO1, HO-1, and GCLM in mouse liver; B: Nrf2 protein expression; C: HO-1 protein expression; D: NQO1 protein expression; E: GCLM protein expression. Control: intraperitoneal injection with normal saline, twice a week for 4 weeks; gavaged with normal saline daily, 4 weeks. Model: intraperitoneal injection with CCl4, twice a week for 4 weeks; gavaged with normal saline daily, 4 weeks. Colchicine: positive group, intraperitoneal injection with CCl4, twice a week for 4 weeks; gavaged with colchicine (0.1 mg/kg) daily, 4 weeks. L-GZFL: intraperitoneal injection with CCl4, twice a week for 4 weeks; gavaged with GZFL (150 mg/kg) daily, 4 weeks. H-GZFL: intraperitoneal injection with CCl4, twice a week for 4 weeks; gavaged with GZFL (300 mg/kg) daily, 4 weeks. Data are presented as mean ± standard deviation (n = 10). GZFL: Guizhifuling pill; CCl4: carbon tetrachloride; Nrf2: nuclear factor-erythroid 2-related factor 2; NQO1: nicotinamide quinone oxidoreductase 1; HO-1: heme oxygenase-1; GCLM: glutamate-cysteine ligase modifier subunit; GAPDH: glyceraldehyde-3-phosphate. a P < 0.01 vs Control; b P < 0.01 vs Model.
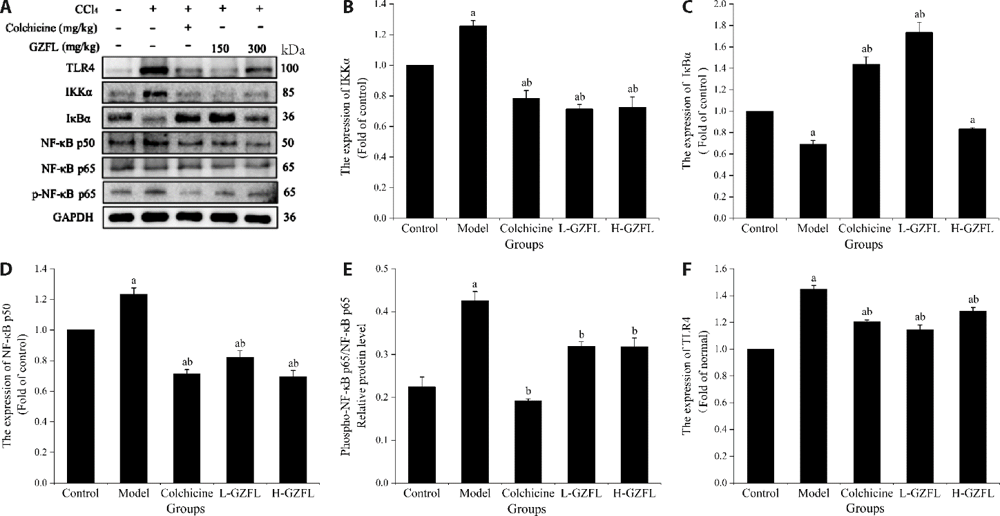
Figure 3 Determination of protein expression in the NF-κB signaling pathway using Western blotting A: Western blotting to determine the expression of IKKα, IκBα, NF-κB p50, NF-κB p65, and p-NF-κB p65 in mouse livers; B: IKKα protein expression; C: IκBα protein expression; D: NF-κB p50 protein expression; E: NF-κB p65 and p-NF-κB p65 protein expression; F: TLR4 protein expression. Control: intraperitoneal injection with normal saline, twice a week for 4 weeks; gavaged with normal saline daily, 4 weeks. Model: intraperitoneal injection with CCl4, twice a week for 4 weeks; gavaged with normal saline daily, 4 weeks. Colchicine: positive group, intraperitoneal injection with CCl4, twice a week for 4 weeks; gavaged with colchicine (0.1 mg/kg) daily, 4 weeks. L-GZFL: intraperitoneal injection with CCl4, twice a week for 4 weeks; gavaged with GZFL (150 mg/kg) daily, 4 weeks. H-GZFL: intraperitoneal injection with CCl4, twice a week for 4 weeks; gavaged with GZFL (300 mg/kg) daily, 4 weeks. Data are presented as mean ± standard deviation (n = 10). GZFL: Guizhifuling pill; CCl4: carbon tetrachloride; TLR4: toll-like receptor 4; NF-κB: nuclear factor-kappa B; IKKα: IKK alpha; p-NF-κB p65: phospho-NF-κB p65; GAPDH: Glyceraldehyde-3-phosphate. a P < 0.01 vs Control; b P < 0.01 vs Model.
| 1. |
Weng TC, Shen CC, Chiu YT, Lin YL, Kuo CD, Huang YT. Inhibitory effects of armepavine against hepatic fibrosis in rats. J Biomed Sci 2009; 16: 78-90.
DOI URL |
| 2. |
Chen Y, Li R, Hu N, et al. Baihe Wuyao decoction ameliorates CCl4-induced chronic liver injury and liver fibrosis in mice through blocking TGF-β1/Smad2/3 signaling, anti-inflammation and anti-oxidation effects. J Ethnopharmacol 2020; 263: 113227-52.
DOI URL |
| 3. |
Tsuchida T. Mechanisms of hepatic stellate cell activation as a therapeutic target for the treatment of non-alcoholic steatohepatitis. Nihon Yakurigaku Zasshi 2019; 154: 203-9.
DOI URL |
| 4. |
Widjaja AA, Singh BK, Adami E, et al. Inhibiting interleukin 11 signaling reduces hepatocyte death and liver fibrosis, inflammation, and steatosis in mouse models of nonalcoholic steatohepatitis. Gastroenterology 2019; 157: 777-92.
DOI PMID |
| 5. |
Campana L, Iredale JP. Regression of liver fibrosis. Semin Liver Dis 2017; 37: 1-10.
DOI PMID |
| 6. |
Xia Y, Yu B, Ma C, et al. Yu Gan Long reduces rat liver fibrosis by blocking TGF-β1/Smad pathway and modulating the immunity. Biomed Pharmacother 2018; 106: 1332-8.
DOI PMID |
| 7. |
Dong S, Cai FF, Chen QL, et al. Chinese herbal formula Fuzheng Huayu alleviates CCl4-induced liver fibrosis in rats: a transcriptomic and proteomic analysis. Acta Pharmacol Sin 2018; 39: 930-41.
DOI PMID |
| 8. |
Li M, Hung A, Li H, Yang AWH. A classic herbal formula Guizhi Fuling Wan for menopausal hot flushes: from experimental findings to clinical applications. Biomedicines 2019; 7: 60-87.
DOI URL |
| 9. | Zhang B. Guizhi Fuling pills inhibit the proliferation, migration and invasion of human cutaneous malignant melanoma cells by regulating the molecular axis of LncRNA TPT1-AS1 / miR-671-5p. Cell Mol Biol (Noisy-le-grand) 2020; 66: 148-54. |
| 10. |
Chen NN, Han M, Yang H, et al. Chinese herbal medicine Guizhi Fuling Formula for treatment of uterine fibroids: a systematic review of randomised clinical trials. BMC Complement Altern Med 2014; 14: 2-11.
DOI URL |
| 11. |
Zhao X, Li R, Liu Y, et al. Polydatin protects against carbon tetrachloride-induced liver fibrosis in mice. Arch Biochem Biophys 2017; 629: 1-7.
DOI URL |
| 12. |
Kong Z, Liu R, Cheng Y. Artesunate alleviates liver fibrosis by regulating ferroptosis signaling pathway. Biomed Pharmacother 2019; 109: 2043-53.
DOI URL |
| 13. |
Wu X, Wu X, Ma Y, et al. CUG-binding protein 1 regulates HSC activation and liver fibrogenesis. Nat Commun 2016; 7: 13498-511.
DOI URL |
| 14. |
Giannini EG, Testa R, Savarino V. Liver enzyme alteration: a guide for clinicians. CMAJ 2005; 172: 367-79.
PMID |
| 15. |
Spinella R, Sawhney R, Jalan R. Albumin in chronic liver disease: structure, functions and therapeutic implications. Hepatol Int 2016; 10: 124-32.
DOI PMID |
| 16. |
Stepien M, Fedirko V, Duarte-Salles T, et al. Prospective association of liver function biomarkers with development of hepatobiliary cancers. Cancer Epidemiol 2016; 40: 179-87.
DOI URL |
| 17. | Hassan B, Tariq IA. Phenolic compounds and hepatoprotective potential of Anastatica hierochuntica ethanolic and aqueous extracts against CCl4-induced hepatotoxicity in rats. J Tradit Chin Med 2020; 40: 947-55. |
| 18. | Sha F, Chang YQ, Ding J. Effects of two cooling modes of low temperature stress on antioxidant enzyme activities and malondiadehyde level in sea cucumber Apostichopu japonicus. J Dalian Ocean Univ 2015; 1: 25-9. |
| 19. |
Klaassen CD, Reisman SA. Nrf2 the rescue: effects of the antioxidative/electrophilic response on the liver. Toxicol Appl Pharmacol 2010; 244: 57-65.
DOI URL |
| 20. |
Anuja GI, Shine VJ, Latha PG, Suja SR. Protective effect of ethyl acetate fraction of Drynaria quercifolia against CCl4 induced rat liver fibrosis via Nrf2/ARE and NFκB signalling pathway. J Ethnopharmacol 2018; 216: 79-88.
DOI PMID |
| 21. |
Maleki SJ, Crespo JF, Cabanillas B. Anti-inflammatory effects of flavonoids. Food Chem 2019; 299: 125124-77.
DOI URL |
| 22. | Mu J, Cheng F, Wang Q, et al. Sini powder ameliorates the inflammatory response in rats with stress-induced non-alcoholic fatty liver disease by inhibiting the nuclear factor kappa-B / pyrin domain-containing protein 3 pathways. J Tradit Chin Med 2020; 40: 253-66. |
| 23. |
Sunami Y, Leithäuser F, Gul S, et al. Hepatic activation of IKK/NFκB signaling induces liver fibrosis via macrophage-mediated chronic inflammation. Hepatology 2012; 56: 1117-28.
DOI URL |
| 24. | Ghosh S, May MJ, Kopp EB. NF-kappa B and Rel proteins: evolutionarily conserved mediators of immune responses. Annu Rev Immunol 1998; 16: 225-60. |
| 25. |
Zheng J, Tian X, Zhang W, et al. Protective effects of fucoxanthin against alcoholic liver injury by activation of Nrf2-mediated antioxidant defense and inhibition of TLR4-mediated inflammation. Mar Drugs 2019; 17: 552-66.
DOI URL |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||

