Journal of Traditional Chinese Medicine ›› 2022, Vol. 42 ›› Issue (3): 364-371.DOI: 10.19852/j.cnki.jtcm.20220225.002
• Research Article • Previous Articles Next Articles
Efficacy of Kushen decoction (苦参汤) on high-fat-diet-induced hyperlipidemia in rats
ZHANG Jiri Mutu1,2, LIANG Shilong1, NIE Peng1, LIAO Yong’an1, AI Qinying1, YAN Xiaojun1, LIU Hongning1, JI Yanhua1( ), ZENG Zhijun1(
), ZENG Zhijun1( )
)
- 1 Research Center for Differention and Development of TCM Basic Theory, Jiangxi Province Key Laboratory of TCM Etiopathogenisis, Jiangxi University of Chinese Medicine, Nanchang, Jiangxi 330006, China
2 Mongolian Medical College, Inner Mongolia Minzu Uaniversity, Tongliao 028000, China
-
Accepted:2021-11-17Online:2022-06-15Published:2022-02-25 -
Contact:JI Yanhua,ZENG Zhijun -
About author:JI Yanhua and ZENG Zhijun, Research Center for Differention and Development of TCM Basic Theory, Jiangxi Province Key Laboratory of TCM Etiopathogenisis, Jiangxi University of Chinese Medicine, Nanchang, Jiangxi 330006, China. 20162018@jxutcm.edu.cn and zhijunzeng@aliyun.com
-
Supported by:Supported by National Natural Science Foundation of China(81760787);China Postdoctoral Science Foundation(2017M622101);Scientific Foundation of the Education Department of Jiangxi Province(GJJ190643);Traditional Chinese Medicine Scientific Research Subject of Jiangxi Province(2019A111);Traditional Chinese Medicine Scientific Research Subject of Jiangxi Province(2019B110);Health and Family Planning Commission of Jiangxi Province(20195651);Health and Family Planning Commission of Jiangxi Province(20203766);Health and Family Planning Commission of Jiangxi Province(20203773);Health and Family Planning Commission of Jiangxi Province(202131047);Health and Family Planning Commission of Jiangxi Province(202131054);Collaborative Innovation of Modern Science and Technology and Industrial Development of Jiangxi National Traditional Medicine(Gan Jiao Gao Zi, [2013] No. 109);Jiangxi middle-aged and young backbone Talents Project of traditional Chinese medicine(Gan TCM Ke Jiao Zi [2021] No. 2);Specialized Research Fund for the First-Class Discipline of Chinese Herb from Jiangxi Province(JXSYLXK-ZHYAO111);Key Discipline Project of Jiangxi University of Chinese Medicine(2013jzzdxk069)
Cite this article
ZHANG Jiri Mutu, LIANG Shilong, NIE Peng, LIAO Yong’an, AI Qinying, YAN Xiaojun, LIU Hongning, JI Yanhua, ZENG Zhijun. Efficacy of Kushen decoction (苦参汤) on high-fat-diet-induced hyperlipidemia in rats[J]. Journal of Traditional Chinese Medicine, 2022, 42(3): 364-371.
share this article
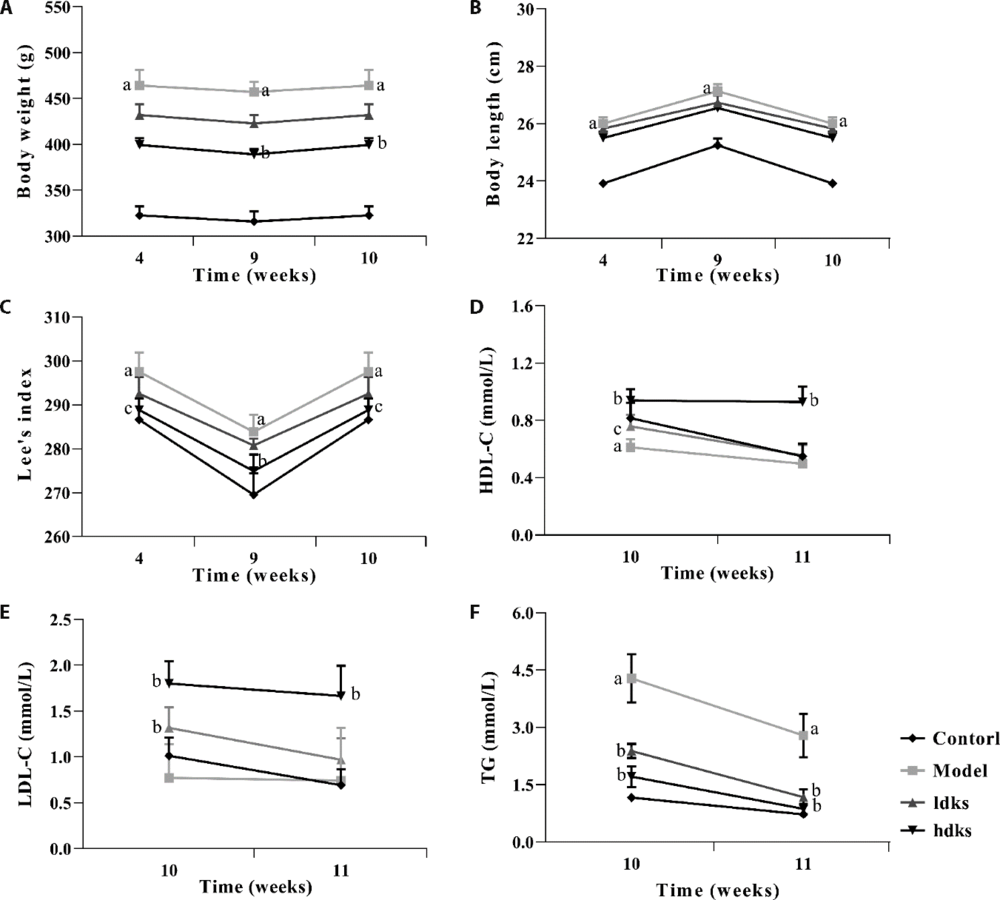
Figure 1 Effect of high-fat diet and treatment with low- or high-dose Kushen (A-F) Different parameters were compared between the control group, the untreated model group (high-fat diet), the model group treated with low-dose Kushen decoction (LDKS), and the model group treated with high-dose decoction (HDKS). (A) body weight; (B) body length; (C) Lee’s index; (D) serum high-density lipoprotein cholesterol (HDL-C); (E) serum low-density lipoprotein cholesterol (LDL-C); and (F) serum triglycerides (TG). Compared with the control group, a high-fat diet significantly increased body weight, body length, Lee’s index, and serum TG (aP < 0.01). Compared with the model group, low-dose Kushen decoction (LDKS group) tended to decrease body weight, body length, and Lee’s index, but the differences were not significant (P > 0.05), while the levels of serum HDL-C (cP < 0.05) and serum LDL-C (bP < 0.01) increased significantly, and the level of serum TG decreases significantly (bP < 0.01). Compared with the model group, high-dose Kushen decoction (HDKS group) decreased significantly body weight, Lee’s index, and serum TG (bP < 0.01), while serum HDL-C and serum LDL-C increased significantly (bP < 0.01).
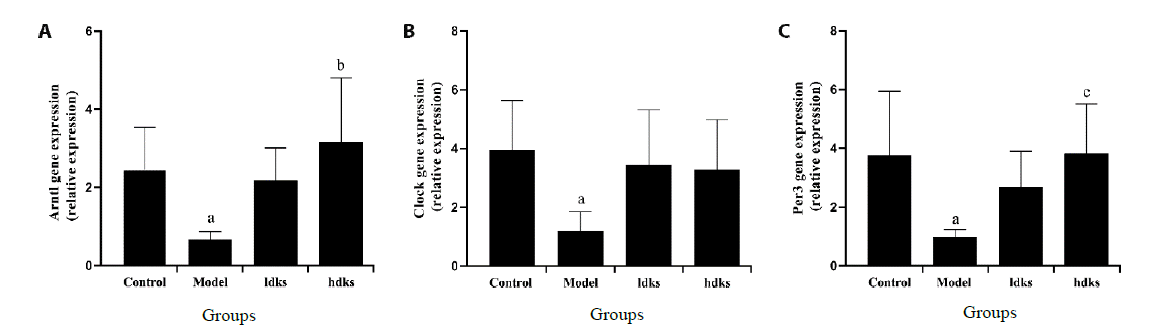
Figure 2 Analysis of ARNTL, CLOCK, and PER3 mRNAs by real-time fluorescent quantitative polymerase chain reaction Bar graphs showing ARNTL (A), CLOCK (B), and PER3 (C) mRNA levels in the different groups. Model group compare with the control group, aP < 0.05; LDKS group and HDKS group compare with the model group, bP < 0.01 or cP < 0.05.
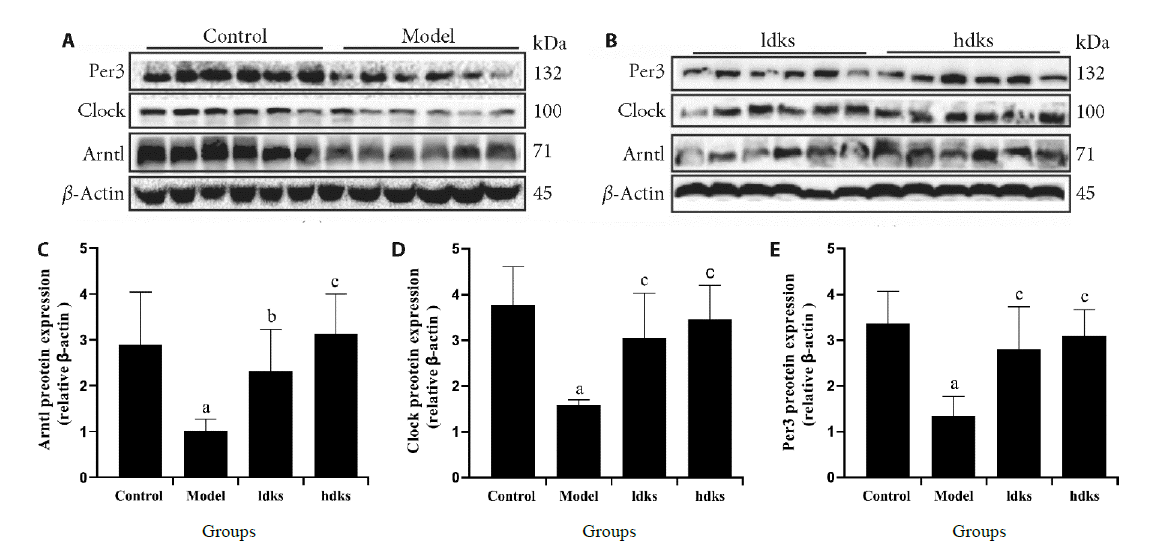
Figure 3 Quantification of the proteins encoded by the DEGs in livers from the different experimental groups Representative immunoblots assessing the target proteins are shown. Molecular weight markers are indicated in kilodaltons (kDa). Protein levels were normalized to internal controls. β-actin was used as a loading control. Bar charts showing ARNTL (C), CLOCK (D), and PER3 (E) protein expression in the different groups. DEGs: differentially expressed genes; LDKS: low-dose Kushen decoction; HDKS: high-dose decoction. Compared with the control group, the expression of ARNTL, PER3, and CLOCK in the model group was decreased significantly (aP < 0.01 versus control group). It can be noted that the expression of ARNTL, PER3, and CLOCK was increased significantly in the LDKS or HDKS group (bP < 0.05 and cP < 0.01 versus model group).
| 1 |
Pan L, Yang ZH, Wu Y, et al. The prevalence, awareness, treatment and control of dyslipidemia among adults in China. Atherosclerosis 2016; 248:2-9.
DOI URL |
| 2 | Writing Group M, Mozaffarian D, Benjamin EJ, et al. Heart Disease and Stroke Statistics-2016 Update: A Report From the American Heart Association. Circulation 2016; 133:e38-360. |
| 3 |
Matsuura E, Kobayashi K, Tabuchi M, et al. Oxidative modification of low-density lipoprotein and immune regulation of atherosclerosis. Progress in Lipid Research 2006; 45:466-86.
PMID |
| 4 | Karr S. Epidemiology and management of hyperlipidemia. Am J Manag Care 2017; 23:S139-48. |
| 5 | Stone NJ, Robinson JG. 2013 ACC/AHA guideline on the treatment of blood cholesterol to-reduce atherosclerotic cardiovascular'risk in adults a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation 2014; 129:S1-45. |
| 6 |
Walsh JME, Pignone M. Drug treatment of hyperlipidemia in women. JAMA 2004; 291:2243-52.
DOI URL |
| 7 |
Pearlman M, Covin Y, Schmidt R, et al. Statins and lower gastrointestinal conditions: a retrospective cohort study. J Clin Pharmacol 2017; 57:1053-63.
DOI URL |
| 8 |
Parker BA, Capizzi JA, Grimaldi AS, et al. Effect of statins on skeletal muscle function. Circulation 2013; 127:96-103.
DOI PMID |
| 9 |
Pedro-Botet J, Climent E, Benaiges D. Muscle and statins: from toxicity to the nocebo effect. Expert Opin Drug Saf 2019; 18:573-9.
DOI PMID |
| 10 |
Chiu HT, Shen LJ, Chen YC. Effect of statin use on the risk of medically attended acute respiratory illness among influenza vaccinated elderly. Vaccine 2018; 36:6133-7.
DOI URL |
| 11 | Lei Q, Peng WN, You H, et al. Statins in nervous system-associated diseases: angels or devils? Die Pharmazie 2014; 69:448-54. |
| 12 | Shah RV, Goldfine AB. Statins and risk of new-onset diabetes mellitus. Circulation 2012; 126:282-4. |
| 13 |
Skoumas J, Liontou C, Chrysohoo C, et al. Statin therapy and risk of diabetes in patients with heterozygous familial hyper-cholesterolemia or familial combined hyperlipidemia. Atherosclerosis 2014; 237:140-5.
DOI PMID |
| 14 |
Zaharan NL, Williams D, Bennett K. Statins and risk of treated incident diabetes in a primary care population. Brit J Clin Pharmaco 2013; 75:1118-24.
DOI URL |
| 15 |
Vera MAD, Bhole V, Burns LC, et al. Impact of statin adherence on cardiovascular disease and mortality outcomes: a systematic review. Brit J Clin Pharmaco 2014; 78:684-98.
DOI URL |
| 16 |
Kim H, Lee MR, Lee GS, et al. Effect of Sophora flavescens Aiton extract on degranulation of mast cells and contact dermatitis induced by dinitrofluorobenzene in mice. J Ethnopharmaco 2012; 142:253-8.
DOI URL |
| 17 |
Yang N, Liang B, Srivastava K, et al. The Sophora flavescens flavonoid compound trifolirhizin inhibits acetylcholine induced airway smooth muscle contraction. Phytochemistry 2013; 95:259-67.
DOI PMID |
| 18 |
Jin SN, Wen JF, Li X, et al. The mechanism of vasorelaxation induced by ethanol extract of Sophora flavescens in rat aorta. J Ethnopharmaco 2011; 137:547-52.
DOI URL |
| 19 |
Bai L, Zhu LY, Yang BS, et al. Antitumor and immunomodulating activity of a polysaccharide from Sophora flavescens Ait. Int J Biol Macromol 2012; 51:705-9.
DOI PMID |
| 20 |
Kim HY, Jeong DM, Jung HJ, et al. Hypolipidemic effects of Sophora flavescens and its constituents in poloxamer 407-induced hyperlipidemic and cholesterol-fed rats. Biol Pharm Bull 2008; 31:73-8.
DOI URL |
| 21 |
He X, Fang J, Huang L, et al. Sophora flavescens Ait: traditional usage, phytochemistry and pharmacology of an important Traditional Chinese Medicine. J Ethnopharmaco 2015; 172:10-29.
DOI URL |
| 22 |
Wu KC, Cui JY, Liu J, et al. RNA-Seq provides new insights on the relative mRNA abundance of antioxidant components during mouse liver development. Free Radical Bio Med 2019; 134:335-42.
DOI URL |
| 23 | Fan JQ, Weng XQ, Xu GQ, et al. Effects of hypoxic exercise on Nesfatin-1 and Ghrelin in hypothalamus of rats with alimentary obesity. J Clin Rehabilitative Tissue Eng Res 2020; 24:3202-8. |
| 24 |
Dewey CN, Bo L. RSEM: accurate transcript quantification from RNA-Seq data with or without a reference genome. BMC Bioinformatics 2011; 12:323-39.
DOI PMID |
| 25 |
Tarazona S, Garcia-Alcalde F, Dopazo J, et al. Differential expression in RNA-seq: a matter of depth. Genome Res 2011; 21:2213-23.
DOI PMID |
| 26 | Benjamini Y, Hochberg Y. Controlling the false discovery rate: a practical and powerful approach to multiple testing. J R Stat Soc 1995; 57:289-300. |
| 27 |
Kanehisa M, Araki M, Goto S, et al. KEGG for linking genomes to life and the environment. Nucleic Acids Res 2008; 36:D480-4.
DOI PMID |
| 28 |
Hanahan D, Weinberg RA. Hallmarks of cancer: the next generation. Cell 2011; 144:646-74.
DOI URL |
| 29 |
Mardinoglu A, Nielsen J. New paradigms for metabolic modeling of human cells. Curr Opin Biotechnol 2015; 34:91-7.
DOI URL |
| 30 | Zeng ZJ, Ji YH, Huang X, et al. Integrating the metpa and ipa to verify the biological function of the potential biomarkers from plasma metabonomics in diabetic rats. Acta Medica Mediterranea 2019; 35:1627-31. |
| 31 | Zeng ZJ, Gao Y, Liu LY, et al. Quickly evaluating the synergistic effects of top anti-cancer drugs by the computer high performance computing power and complex network visualization. J Intell Fuzzy Syst 2020; 38:277-81. |
| 32 |
Otto TC, Lane MD. Adipose development: from stem cell to adipocyte. Crit Rev Biochem Mol 2005; 40:229-42.
DOI URL |
| 33 |
Chen H, Mo D, Li M, et al. miR-709 inhibits 3T3-L1 cell differentiation by targeting GSK3β of Wnt/β-catenin signaling. Cell Signal 2014; 26:2583-9.
DOI PMID |
| 34 |
Wu Z, Rosen ED, Brun R, et al. Cross-regulation of C/EBP alpha and PPAR gamma controls the transcriptional pathway of adipogenesis and insulin sensitivity. Mol Cell 1999; 3:151-8.
PMID |
| 35 |
Chaix A, Zarrinpar A, Panda S. The circadian coordination of cell biology. J Cell Biol 2016; 215:15-25.
DOI URL |
| 36 | Liu YL, Su D, Zhang L, et al. Endogenous L-carnosine level in diabetes rat cardiac muscle. Evid-Based Compl Alt 2016; 2016:6230825. |
| 37 |
Rudic RD, McNamara P, Curtis AM, et al. BMAL1 and CLOCK, two essential components of the circadian clock, are involved in glucose homeostasis. PLoS Biol 2004; 2:e377.
DOI URL |
| 38 |
Yoo SH, Yamazaki S, Lowrey PL, et al. PERIOD2: LUCIFERASE real-time reporting of circadian dynamics reveals persistent circadian oscillations in mouse peripheral tissues. Proc Natl Acad Sci USA 2004; 101:5339-46.
DOI URL |
| 39 |
Turek FW, Joshu C, Kohsaka A, et al. Obesity and metabolic syndrome in circadian CLOCK mutant mice. Science 2005; 308:1043-5.
DOI PMID |
| 40 | Shi XB, Mackie B, Zhang G, et al. Identification of the metabolic enzyme involved morusin metabolism and characterization of its metabolites by ultraperformance liquid chromatography quadrupole time-of-flight mass spectrometry (UPLC/Q-TOF-MS/MS). Evid-Based Compl Alt 2016; 2016:9240103. |
| 41 |
Shimba S, Ishii N, Ohta Y, et al. Brain and muscle Arnt-like protein-1 (BMAL1), a component of the molecular clock, regulates adipogenesis. Proc Natl Acad Sci USA 2005; 102:12071-6.
DOI URL |
| 42 |
Curtis AM, Cheng Y, Kapoor S, et al. Circadian variation of blood pressure and the vascular response to asynchronous stress. Proc Natl Acad Sci USA 2007; 104:3450-5.
DOI URL |
| 43 |
Kohsaka A, Laposky AD, Ramsey KM, et al. High-fat diet disrupts behavioral and molecular circadian rhythms in mice. Cell Metab 2007; 6:414-21.
PMID |
| 44 |
Hatori M, Vollmers C, Zarrinpar A, et al. Time-restricted feeding without reducing caloric intake prevents metabolic diseases in mice fed a high-fat diet. Cell Metab 2012; 15:848-60.
DOI URL |
| 45 |
Potter GD, Cade JE, Grant PJ, et al. Nutrition and the circadian system. Br J Nutr 2016; 116:434-42.
DOI URL |
| 46 |
Scott EM, Carter AM, Grant PJ. Association between polymorphisms in the CLOCK gene, obesity and the metabolic syndrome in man. Int J Obes (Lond) 2008; 32:658-62.
DOI URL |
| 47 |
Sookoian S, Gemma C, Gianotti TF, et al. Genetic variants of CLOCK transcription factor are associated with individual susceptibility to obesity. Am J Clin Nutr 2008; 87:1606-15.
DOI PMID |
| 48 | Gao BZ, Chen JC, Liao LH, et al. Erchen decoction prevents high-fat diet induced metabolic disorders in C57BL/6 mice. Evid Based Complement Alternat Med 2015; 2015:501272. |
| 49 |
You DY, Wu ZY, Wan JX, et al. Analysis of renal functions and proteinuria in young obese adults. J Endocrinol Invest 2015; 38:901-8.
DOI PMID |
| 50 |
Aggarwal A, Costa MJ, Rivero-Gutierrez B, et al. The circadian clock regulates adipogenesis by a PER3 crosstalk pathway to Klf15. Cell Rep 2017; 21:2367-75.
DOI URL |
| 51 | Ji YH, Luo KX, Zhang JM, et al. Obese rats intervened with Rhizoma coptidis revealed differential gene expression and microbiota by serum metabolomics. BMC Complement Med 2021; 21:208. |
| [1] | ZHI Guoguo, SHAO Bingjie, ZHENG Tianyan, JI Shaoxiu, LI Jingwei, DANG Yanni, LIU Feng, WANG Dong. Efficacy of Ganshuang granules (肝爽颗粒) on non-alcoholic fatty liver and underlying mechanism: a network pharmacology and experimental verification [J]. Journal of Traditional Chinese Medicine, 2024, 44(1): 122-130. |
| [2] | ZHANG Qi, CHEN Dexuan, ZHU Guixiang, ZHANG Shihu, FENG Xiao, MA Chaoqun, ZHANG Yi. Efficacy of Tounongsan decoction (透脓散方) on pyogenic liver abscess: network pharmacology and clinical trial validation [J]. Journal of Traditional Chinese Medicine, 2024, 44(1): 145-155. |
| [3] | YANG Shaojun, MA Yanhua, BAI Zhouxia, YU Ye, FANG Buwu, ZHANG Li, WANG Li. Intervention effect of Cigu Xiaozhi prescription (慈菇消脂方) on ceramide lipoapoptosis in non-alcoholic fatty liver disease [J]. Journal of Traditional Chinese Medicine, 2024, 44(1): 63-69. |
| [4] | YIN Yixiao, TANG Hao, FANG Yi, LIU Wei, WANG Jun, HU Yiyang, PENG Jinghua. Hepatic transcriptome delineates the therapeutic effects of Sanren Tang (三仁汤) on high-fat diet-induced non-alcoholic fatty liver disease [J]. Journal of Traditional Chinese Medicine, 2023, 43(6): 1092-1102. |
| [5] | ZHANG Junli, HE Ying, ZHANG Xia, FU Hongfang, HU Xiaoyu. Fuzheng Huayu preparation (扶正化瘀胶囊/片) combined with tenofovir disoproxil fumarate on hepatitis B: a systematic review and Meta-analysis [J]. Journal of Traditional Chinese Medicine, 2023, 43(2): 221-230. |
| [6] | QU Dongxiao, GE Yiqin, ZHUO Limin, CHEN Liji, XUE Yonghua, CHENG Jiwei, TAO Jie, LI Guoyi, ZHU Yudan, XIAO Qian. Efficacy and mechanisms of Dingxian pill (定痫丸) combined with valproic acid on pentylenetetrazol-induced chronic epilepsy in rats [J]. Journal of Traditional Chinese Medicine, 2023, 43(2): 286-294. |
| [7] | WANG Bochuan, ZHANG Yong, ZHANG Qiuyun, ZHANG Zhiqiang, LUO Changyong, WANG Zhendong, BAI Chen, WANG Yuhan, GE Xueyi, QIAN Ying, YU He, GU Xiaohong. Reveal the mechanisms of prescriptions for liver cancer' treatment based on two illustrious senior TCM physicians [J]. Journal of Traditional Chinese Medicine, 2023, 43(1): 188-197. |
| [8] | DING Yanping, DONG Xiaoqing, MA Yifan, CHEN Lili, ZHOU Jie, LI Xinyan, SHAO Baoping. Astragaloside IV plays a role in reducing radiation-induced liver inflammation in mice by inhibiting thioredoxin-interacting protein/nod-like receptor protein 3 signaling pathway [J]. Journal of Traditional Chinese Medicine, 2023, 43(1): 87-94. |
| [9] | FAN Xiaoyan, LI Mingzhe, CHEN Long, LIANG Chao, LU Wenli, PAN Zhiqiang, JIA Dongwei, PENG Peike, FANG Zhaoqin, LIU Xiaomei. Transcriptome profile and its partly verification of human hepatocellular carcinoma cells exposed to Yuzhizi (Fructus Akebiae Quinatae) seed extract [J]. Journal of Traditional Chinese Medicine, 2022, 42(6): 922-931. |
| [10] | LI Xiaoling, SUN Fengxia, SHANG Zimeng, ZHANG Yingxue, LI Jie, ZHANG Qiuxiang. Effect of Dangfei Liganning capsule (当飞利肝宁胶囊) on liver X receptor α/steroid regulatory element binding protein-1/fatty acid synthase signal pathway in rats with metabolic- associated fatty liver disease [J]. Journal of Traditional Chinese Medicine, 2022, 42(6): 940-947. |
| [11] | XU Baogui, ZHENG Jiawen, TIAN Xiaoxiao, YUAN Falei, LIU Zhongliang, YANG Zuisu, DING Xianjun. Antihepatofibrotic effect of Guizhifuling pill (桂枝茯苓丸) on carbon tetrachloride-induced liver fibrosis in mice [J]. Journal of Traditional Chinese Medicine, 2022, 42(5): 715-722. |
| [12] | YANG Jiayao, TAO Dongqing, MA Wei, LIU Song, LIAO Yan, SHU Lei, ZHANG Shu, LI Chenyu, DU Nianlong. Protective effects and mechanisms of Lizhong decoction (理中汤) against non-alcoholic fatty liver disease in a rat model [J]. Journal of Traditional Chinese Medicine, 2022, 42(5): 773-780. |
| [13] | ZHOU Kaixuan, ZHANG Dong, BAO Huiwei, LI Lijing. Network pharmacology and molecular docking study on the effect of Kaempferol in treatment of metabolic associated fatty liver disease [J]. Journal of Traditional Chinese Medicine, 2022, 42(5): 788-794. |
| [14] | ZHANG Di, WEI Muyun, CHEN Luan, WU Hao, WANG Ting, ZHANG Zhiruo, ZHANG Ying, YU Juan, HUANG Jinming, ZHU Jinhang, QIN Shengying. Drug response biomarkers of Pien Tze Huang (片仔癀) treatment for hepatic fibrosis induced by carbon tetrachloride [J]. Journal of Traditional Chinese Medicine, 2022, 42(4): 530-538. |
| [15] | WU Tong, YANG Zhiyun, YANG Yuying, JIANG Yuyong, MENG Peipei, LIU Huimin, TIAN Yehong, ZHANG Qiaoli. Effect of decoction of Fuzheng Jiedu Xiaoji formula (扶正解毒消积方) plus chemoembolization on primary liver cancer in patients [J]. Journal of Traditional Chinese Medicine, 2022, 42(3): 446-450. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||

