Journal of Traditional Chinese Medicine ›› 2022, Vol. 42 ›› Issue (5): 773-780.DOI: 10.19852/j.cnki.jtcm.2022.05.009
• Research Articles • Previous Articles Next Articles
Protective effects and mechanisms of Lizhong decoction (理中汤) against non-alcoholic fatty liver disease in a rat model
YANG Jiayao1( ), TAO Dongqing2, MA Wei3(
), TAO Dongqing2, MA Wei3( ), LIU Song1, LIAO Yan1, SHU Lei1, ZHANG Shu1, LI Chenyu4, DU Nianlong1
), LIU Song1, LIAO Yan1, SHU Lei1, ZHANG Shu1, LI Chenyu4, DU Nianlong1
- 1 Department of Gastroenterology, Wuhan Integrated TCM and Western Medicine Hospital, Wuhan 430022, China
2 Department of Endocrinology, The Third People's Hospital of Hubei Province, Wuhan 430033, China
3 Department of Center Laboratory, Wuhan Integrated TCM and Western Medicine Hospital, Wuhan 430022, China
4 Hubei University of Traditional Chinese Medicine, Wuhan 430065, China
-
Received:2020-09-11Accepted:2020-11-22Online:2022-10-15Published:2022-09-02 -
Contact:YANG Jiayao,MA Wei -
About author:Dr. MA Wei, Department of Center Laboratory, Wuhan Integrated TCM and Western Medicine Hospital, Wuhan 430022, China. saturn119@126.com Telephone: +86-27-85332952
Dr. YANG Jiayao, Department of Gastroenterology, Wuhan Integrated TCM and Western Medicine Hospital, Wuhan 430022, China. yjy0813m@sina.com;
-
Supported by:Backbone Talents for TCM Clinical Characteristic Technology Inheritance Foundation of State Administration of Traditional Chinese Medicine: Protective Effects and Mechanisms of Lizhong Decoction Against Non-Alcoholic Fatty Liver Disease in a Rat Model[National Education Letter of Traditional Chinese Medicine (2018) No. 224]
Cite this article
YANG Jiayao, TAO Dongqing, MA Wei, LIU Song, LIAO Yan, SHU Lei, ZHANG Shu, LI Chenyu, DU Nianlong. Protective effects and mechanisms of Lizhong decoction (理中汤) against non-alcoholic fatty liver disease in a rat model[J]. Journal of Traditional Chinese Medicine, 2022, 42(5): 773-780.
share this article
| Description | m.z. | Retention time (min) | LQ.POS.B |
|---|---|---|---|
| (S)-6-Gingerol | 317.1722197 | 10.16476667 | 248213.9369 |
| (S)-10-Gingerol | 373.2348731 | 13.0956 | 17507.8542 |
| Codonopsine | 268.1547642 | 2.000383333 | 258584.092 |
| Ononin | 431.1337274 | 6.9596 | 53658.64084 |
| Glyasperin C | 357.1695767 | 10.57258333 | 23024.92605 |
| Licoisoflavanone | 355.1182044 | 10.89071667 | 20823.99042 |
| Gancaonin B | 369.1332263 | 10.43675 | 11995.62021 |
Table 1 Candidate active substances of LZD
| Description | m.z. | Retention time (min) | LQ.POS.B |
|---|---|---|---|
| (S)-6-Gingerol | 317.1722197 | 10.16476667 | 248213.9369 |
| (S)-10-Gingerol | 373.2348731 | 13.0956 | 17507.8542 |
| Codonopsine | 268.1547642 | 2.000383333 | 258584.092 |
| Ononin | 431.1337274 | 6.9596 | 53658.64084 |
| Glyasperin C | 357.1695767 | 10.57258333 | 23024.92605 |
| Licoisoflavanone | 355.1182044 | 10.89071667 | 20823.99042 |
| Gancaonin B | 369.1332263 | 10.43675 | 11995.62021 |
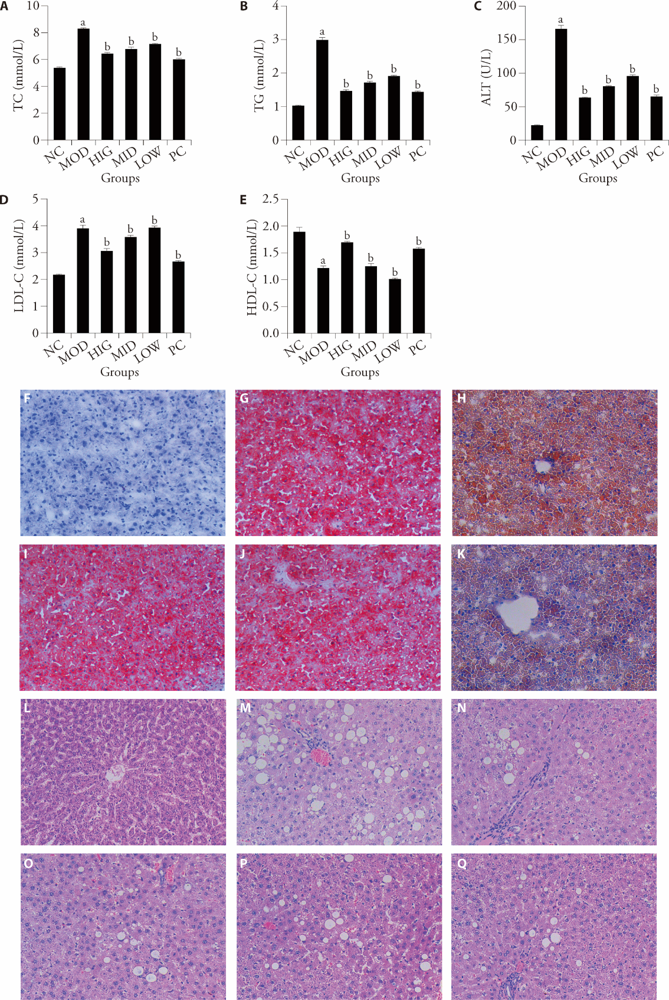
Figure 1 LZD alleviates NAFLD symptoms A: ELISA detect the levels of TC in liver tissues; B: ELISA detect the levels of TG in liver tissues; C: ELISA detect the levels of ALT in liver tissues; D: ELISA detect the levels of LDL-C in liver tissues; E: ELISA detect the levels of HDL-C in liver tissues; F-K: Oil Red O staining observes liver tissues of NC, MOD, HIG, LOW, and PC (× 200); L-Q: hematoxylin-eosin staining observes liver tissues of NC, MOD, HIG, LOW, and PC (× 200). NC group: standard chow diet for four weeks, rats treated with saline (n = 8); MOD group: high-fat diet for four weeks, rats treated with saline (n = 8); HIG group: high-fat diet for four weeks, rats treated with LZD at a daily dose of 16 g/kg (n = 8); MID group: high-fat diet for four weeks, rats treated with LZD at a daily dose of 8 g/kg (n = 8); LOW group: high-fat diet for four weeks, rats treated with LZD at a daily dose of 4 g/kg (n = 8); PC group: high-fat diet for four weeks, rats treated with vitamin E at a daily dose of 250 mg/kg (n = 8); All rats treated for four weeks. LZD: Lizhong decoction; NAFLD: non-alcoholic fatty liver disease; ELISA: enzyme-linked immunosorbent assay; NC: negative control; MOD: model control; HIG: high-dose Lizhong decoction; MID: medium-dose Lizhong decoction; LOW: low-dose Lizhong decoction; PC: positive control; TG: triglyceride; TC: total cholesterol; LDL-C: low-density lipoprotein cholesterol; HDL-C: high-density lipoprotein cholesterol; ALT: alanine aminotransferase. aP < 0.05, compared with the NC group; bP < 0.05, compared with the MOD group.
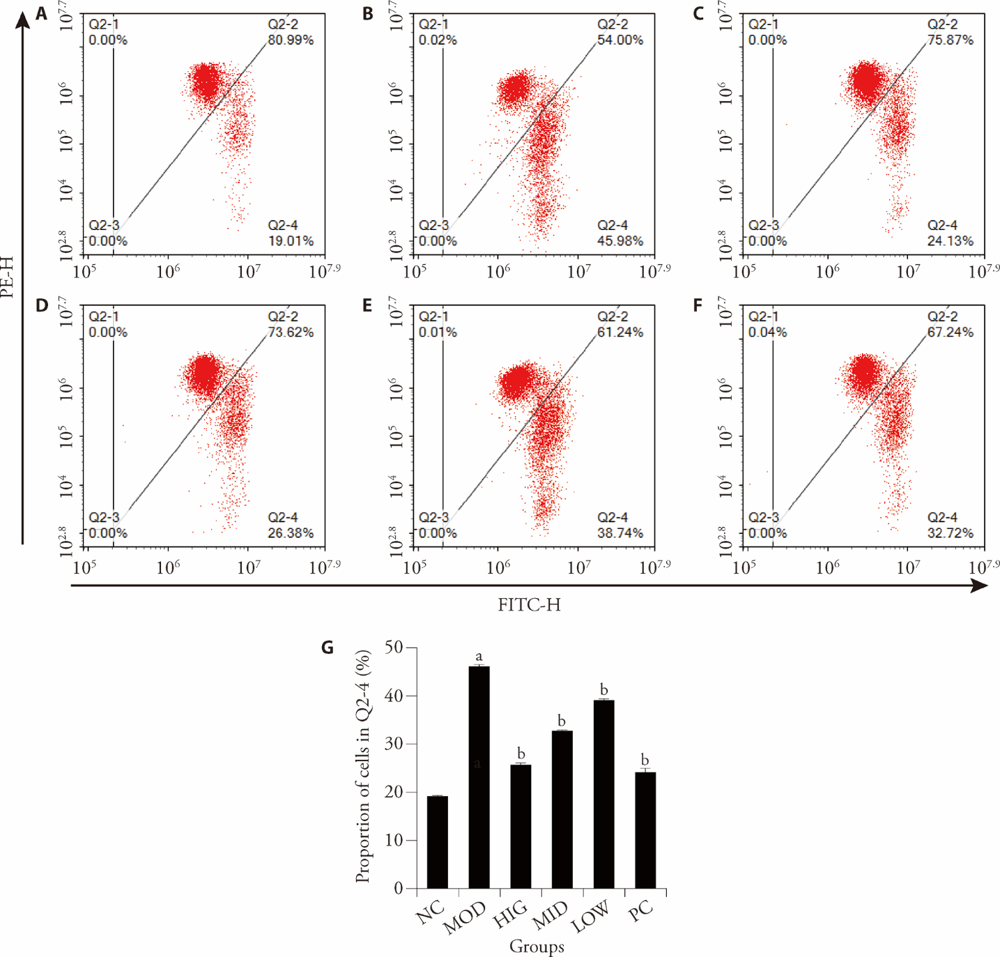
Figure 2 Effect of LZD treatment on mitochondrial function in NAFLD-induced rats A-F: flow cytometry detects green fluorescence signal of NC, MOD, HIG, LOW, and PC; G: proportion of cells in Q2-4. NC group: standard chow diet for four weeks, rats treated with saline (n = 8); MOD group: high-fat diet for four weeks, rats treated with saline (n = 8); HIG group: high-fat diet for four weeks, rats treated with LZD at a daily dose of 16 g/kg (n = 8); MID group: high-fat diet for four weeks, rats treated with LZD at a daily dose of 8 g/kg (n = 8); LOW group: high-fat diet for four weeks, rats treated with LZD at a daily dose of 4 g/kg (n = 8); PC group: high-fat diet for four weeks, rats treated with vitamin E at a daily dose of 250 mg/kg ( n = 8); All rats treated for four weeks. LZD: Lizhong decoction; NAFLD: non-alcoholic fatty liver disease; NC: negative control; MOD: model control; HIG: high-dose Lizhong decoction; MID: medium-dose Lizhong decoction; LOW: low-dose Lizhong decoction; PC: positive control. aP < 0.05, compared with the NC group. bP < 0.05, compared with the MOD group.
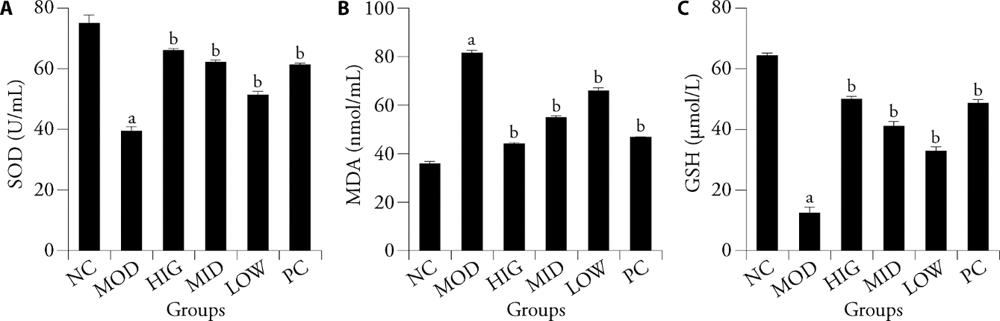
Figure 3 LZD reduces oxidative stress in liver of rats fed a high-fat diet A-C: Kit detect the levels of SOD, MDA, and GSH in liver tissues. NC group: standard chow diet for four weeks, rats treated with saline (n = 8); MOD group: high-fat diet for four weeks, rats treated with saline (n = 8); HIG group: high-fat diet for four weeks, rats treated with LZD at a daily dose of 16 g/kg (n = 8); MID group: high-fat diet for four weeks, rats treated with LZD at a daily dose of 8 g/kg (n = 8); LOW group: high-fat diet for four weeks, rats treated with LZD at a daily dose of 4 g/kg (n = 8); PC group: high-fat diet for four weeks, rats treated with vitamin E at a daily dose of 250 mg/kg (n = 8); All rats treated for four weeks. LZD: Lizhong decoction; NC: negative control; MOD: model control; HIG: high-dose Lizhong decoction; MID: medium-dose Lizhong decoction; LOW: low-dose Lizhong decoction; PC: positive control; SOD: superoxide dismutase; MDA: malondialdehyde; GSH: glutathione. aP < 0.05, compared with the NC group; bP < 0.05, compared with the MOD group.

Figure 4 LZD inhibits the inflammatory response in the livers of rats fed a high-fat diet A-C: Western blot detects the protein expression of PPAR-γ, DPP4, TNF-α, IL-1β, IL-6, and p-JNK in liver tissues; B: relative protein expression of PPAR-γ and DPP4; C: relative protein expression of TNF-α, IL-1β, IL-6, and p-JNK. NC group: standard chow diet for four weeks, rats treated with saline (n = 8); MOD group: high-fat diet for four weeks, rats treated with saline (n = 8); HIG group: high-fat diet for four weeks, rats treated with LZD at a daily dose of 16 g/kg (n = 8); MID group: high-fat diet for four weeks, rats treated with LZD at a daily dose of 8 g/kg (n = 8); LOW group: high-fat diet for four weeks, rats treated with LZD at a daily dose of 4 g/kg (n = 8); PC group: high-fat diet for four weeks, rats treated with vitamin E at a daily dose of 250 mg/kg (n = 8); All rats treated for four weeks. LZD: Lizhong decoction; NC: negative control; MOD: model control; HIG: high-dose Lizhong decoction; MID: medium-dose Lizhong decoction; LOW: low-dose Lizhong decoction; PC: positive control; PPAR-γ: peroxisome proliferator activated receptor gamma; DPP4: dipeptidyl peptidase 4; TNF-α: tumor necrosis factor α; IL-1: interleukin 1 beta; IL-6: interleukin-6; p-JNK: c-Jun N-terminal kinase. aP < 0.05, compared with the NC group; bP < 0.05, compared with the MOD group.
| 1. |
Hassan K, Bhalla V, EI Regal ME, A-Kader HH. Nonalcoholic fatty liver disease: a comprehensive review of a growing epidemic. World J Gastroenterol 2014; 20: 12082-101.
DOI URL |
| 2. |
Koppe SW. Obesity and the liver: nonalcoholic fatty liver disease. Transl Res 2014; 164: 312-22.
DOI PMID |
| 3. |
Michelotti GA, Machado MV, Diehl AM. NAFLD, NASH and liver cancer. Nat Rev Gastroenterol Hepatol 2013; 10: 656-65.
DOI PMID |
| 4. |
Baffy G, Brunt EM, Caldwell SH. Hepatocellular carcinoma in non-alcoholic fatty liver disease: an emerging menace. J Hepatol 2012; 56: 1384-91.
DOI URL |
| 5. | Mavrogiannaki AN, Migdalis IN. Nonalcoholic fatty liver disease, diabetes mellitus and cardiovascular disease: newer data. Int J Endocrinol 2013; 2013: 450639. |
| 6. |
Buzzetti E, Pinzani M, Tsochatzis EA. The multiple-hit pathogenesis of non-alcoholic fatty liver disease (NAFLD). Metabolism 2016; 65: 1038-48.
DOI URL |
| 7. |
Marzuillo P, Grandone A, Perrone L, Miraglia Del Giudice E. Understanding the pathophysiological mechanisms in the pediatric non-alcoholic fatty liver disease: the role of genetics. World J Hepatol 2015; 7: 1439-43.
DOI URL |
| 8. | Enjoji M, Yasutake K, Kohjima M, Nakamuta M. Nutrition and nonalcoholic fatty liver disease: the significance of cholesterol. Int J Hepatol 2012; 2012: 925807. |
| 9. |
Jin SH, Yang L, Fan XF, et al. Effect of divergence in residual feed intake on expression of lipid metabolism-related genes in the liver of meat-type ducks1. J Anim Sci 2019; 97: 3947-57.
DOI URL |
| 10. |
Xuan GS, Oh SW, Choi EY. Development of an electrochemical immunosensor for alanine aminotransferase. Biosens Bioelectron 2003; 19: 365-71.
DOI URL |
| 11. |
Zhou Y, Ding YL, Zhang JL, Zhang P, Wang JQ, Li ZH. Alpinetin improved high fat diet-induced non-alcoholic fatty liver disease (NAFLD) through improving oxidative stress, inflammatory response and lipid metabolism. Biomed Pharmacother 2018; 97: 1397-408.
DOI URL |
| 12. |
Ong SB, Hall AR, Hausenloy DJ. Mitochondrial dynamics in cardiovascular health and disease. Antioxid Redox Signal 2013; 19: 400-14.
DOI URL |
| 13. |
Pomara C, Neri M, Bello S, Fiore C, Riezzo I, Turillazzi E. Neurotoxicity by synthetic androgen steroids: oxidative stress, apoptosis, and neuropathology: a review. Curr Neuropharmacol 2015; 13: 132-45.
DOI URL |
| 14. |
Tahara A, Kurosaki E, Yokono M, et al. Effects of SGLT2 selective inhibitor ipragliflozin on hyperglycemia, hyperlipidemia, hepatic steatosis, oxidative stress, inflammation, and obesity in type 2 diabetic mice. Eur J Pharmacol 2013; 715: 246-55.
DOI PMID |
| 15. | Mario M, Valerio R, Marcello D, et al. Role of oxidative stress in pathophysiology of nonalcoholic fatty liver disease. Oxid Med Cell Longev 2018; 2018: 9547613. |
| 16. |
Cheng S, Yang Y, Zhou Y, Xiang W, Yao H, Ma L. Influence of different concentrations of uric acid on oxidative stress in steatosis hepatocytes. Exp Ther Med 2018; 15: 3659-65.
DOI PMID |
| 17. |
Deevska G, Sunkara M, Karakashian C, Peppers B, Morris AJ, Nikolova-Karakashian MN. Effect of Procysteine on aging-associated changes in hepatic GSH and SMase: evidence for transcriptional regulation of smpd3. J Lipid Res 2014; 55: 2041-52.
DOI URL |
| 18. |
Xu T, Zhou J, Zhu J, et al. Carnosic acid protects non-alcoholic fatty liver-induced dopaminergic neuron injury in rats. Metab Brain Dis 2017; 32: 483-91.
DOI URL |
| 19. | Duarte N, Coelho IC, Patarrão RS, Almeida JI, Penha-Gonçalves C, Macedo MP. How inflammation impinges on NAFLD: a role for kupffer cells. BioMed Res Int 2015; 2015: 984578. |
| 20. |
Liberal R, Grant CR, Mieli-Vergani G, Vergani D. Autoimmune hepatitis: a comprehensive review. J Autoimmun 2013; 41: 126-39.
DOI URL |
| 21. |
Malhi H, Brook SF, Werneburg NW, Gores GJ. Free fatty acids induce JNK-dependent hepatocyte lipoapoptosis. J Biol Chem 2006; 281: 12093-101.
DOI URL |
| 22. |
Celinski K, Dworzanski T, Fornal R, et al. Comparison of anti-inflammatory properties of peroxisome proliferator-activated receptor gamma agonists rosiglitazone and troglitazone in prophylactic treatment of experimental colitis. J Physiol Pharmacol 2013; 64: 587-95.
PMID |
| 23. |
Baumeier C, Schlüter L, Saussenthaler S, et al. Elevated hepatic DPP4 activity promotes insulin resistance and non-alcoholic fatty liver disease. Mol Metab 2017; 6: 1254-63.
DOI URL |
| [1] | YANG Shaojun, MA Yanhua, BAI Zhouxia, YU Ye, FANG Buwu, ZHANG Li, WANG Li. Intervention effect of Cigu Xiaozhi prescription (慈菇消脂方) on ceramide lipoapoptosis in non-alcoholic fatty liver disease [J]. Journal of Traditional Chinese Medicine, 2024, 44(1): 63-69. |
| [2] | YIN Yixiao, TANG Hao, FANG Yi, LIU Wei, WANG Jun, HU Yiyang, PENG Jinghua. Hepatic transcriptome delineates the therapeutic effects of Sanren Tang (三仁汤) on high-fat diet-induced non-alcoholic fatty liver disease [J]. Journal of Traditional Chinese Medicine, 2023, 43(6): 1092-1102. |
| [3] | ZHANG Chengfei, QIN Lingling, WANG Haiyan, SUN Boju, ZHAO Dan, ZHANG Qiue, ZHONG Fengying, WU Lili, LIU Tonghua. Efficacy of aqueous extract of flower of Edgeworthia gardneri (Wall.) Meisn on glucose and lipid metabolism in KK/Upj-Ay/J mice [J]. Journal of Traditional Chinese Medicine, 2022, 42(2): 187-193. |
| [4] | MA Yanhua, HAN Tao, YANG Shaojun, YU Chengzu, SHI Xia, WU Yan. Efficacy of Cigu Xiaozhi pill(慈菇消脂丸) on non-alcoholic steatohepatitis-associated lipoapoptosis through stress-activated c-Jun N-terminal kinase signalling pathway [J]. Journal of Traditional Chinese Medicine, 2021, 41(1): 79-88. |
| [5] | Wang Jianxing, Yu Xiaohan, Jiang Yan, Wang Yan, Li Ying, Han Shuying. Effects of a fermented buckwheat flower and leaf extract on the blood glucose and lipid profile of type 2 diabetic db/db mice [J]. Journal of Traditional Chinese Medicine, 2020, 40(2): 197-203. |
| [6] | Xiao Huanming, Jiang Junmin, Xie Yubao, Shi Meijie, Tian Guangjun, Zhao Pengtao, Zhang Chaozhen, Chen Huijun, Xu Chanyuan, Chi Xiaoling. Colon hydrotherapy plus Traditional Chinese Medicine to treat non-alcoholic fatty liver disease: a pilot study [J]. Journal of Traditional Chinese Medicine, 2017, 37(03): 393-396. |
| [7] | Wang Yan, Wang Xiaozhong, Zeng Binfang, Guo Feng, He Yongquan, He Jiaying, Liu Bin. Association between peroxisome proliferator-activated receptor γ gene polymorphism and susceptibility to northwest dryness syndrome [J]. Journal of Traditional Chinese Medicine, 2017, 37(02): 201-206. |
| [8] | Liang Huiqing, Yang Jiaen, Tang Jinmo, Wu Chuncheng, Li Hongshan, Chen Shaodong. Optimization of dosage ratio of chlorogenic acid and gardenia glycosides in the treatment of rats with fatty liver disease induced by high-fat feed [J]. Journal of Traditional Chinese Medicine, 2016, 36(05): 683-688. |
| [9] | Shaodong Chen, Haihong Zhou, Manting Lin, Ran Mi, Long Li. Decoction vs extracts-mixed solution: effect of Yiqihuoxue formula on non-alcoholic fatty liver disease in rats [J]. Journal of Traditional Chinese Medicine, 2013, 33(04): 513-517. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||

