Journal of Traditional Chinese Medicine ›› 2024, Vol. 44 ›› Issue (1): 197-204.DOI: 10.19852/j.cnki.jtcm.20231204.002
• Original articles • Previous Articles Next Articles
Efficacy and safety of Chinese herbal medicine as adjunctive therapy in sepsis patients with bloodstream infection: a propensity-matched analysis
ZHOU Xianshi1, ZHONG Minlin2, XI Xiaotu3, LI Jun4( ), TANG Guanghua1(
), TANG Guanghua1( )
)
- 1 the Second Clinical College of Guangzhou University of Chinese Medicine, Guangzhou 510120, China; Emergency Department, Guangdong Provincial Hospital of Chinese Medicine, Guangzhou 510120, China; Guangdong Provincial Key Laboratory of Research on Emergency in TCM, Guangzhou 510120, China
2 Emergency Department, Guangdong Provincial Hospital of Chinese Medicine, Guangzhou 510120, China
3 Emergency Department, Guangdong Provincial Hospital of Chinese Medicine, Guangzhou 510120, China; Guangdong Provincial Key Laboratory of Research on Emergency in TCM, Guangzhou 510120, China; Guangzhou Key Laboratory of Traditional Chinese Medicine for Prevention and Treatment of Emerging Infectious Diseases, Guangzhou 510120, China
4 Administration Department, the First Hospital of Guangzhou University of Chinese Medicine, Guangzhou 510405, China
-
Received:2022-11-11Accepted:2023-02-18Online:2024-02-15Published:2023-12-04 -
Contact:LI Jun, Administration Department, the first hospital of Guangzhou University of Chinese Medicine, Guangzhou 510405, China. junlilijun123@126.com;TANG Guanghua, the Second Clinical College of Guangzhou University of Chinese Medicine, Guangzhou 510120, China; Emergency Department, Guangdong Provincial Hospital of Chinese Medicine, Guangzhou 510120, China; Guangdong Provincial Key Laboratory of Research on Emergency in TCM, Guangzhou 510120, China. guanghuatang123@yeah.net. Telephone: +86-20-81887233 -
Supported by:Clinical Research Program of Guangdong Provincial Hospital of Chinese Medicine: Exploring the Epidemiological Characteristics and Screening Key Prognostic Indicators of Sepsis Patients with Bloodstream Infection(2019KT1317);which is a sub-project of Guangdong Provincial Key Laboratory of Research on Emergency in TCM(2017B030314176)
Cite this article
ZHOU Xianshi, ZHONG Minlin, XI Xiaotu, LI Jun, TANG Guanghua. Efficacy and safety of Chinese herbal medicine as adjunctive therapy in sepsis patients with bloodstream infection: a propensity-matched analysis[J]. Journal of Traditional Chinese Medicine, 2024, 44(1): 197-204.
share this article
| Item | Total (n = 973) | Control group (n = 93) | CHM group (n = 880) | P value |
|---|---|---|---|---|
| Age (years) | 68.0 (57.0, 80.0) | 67.0 (56.5, 79.5) | 68.0 (57.0, 80.0) | 0.894 |
| Male [n (%)] | 527 (54.2) | 49 (52.7) | 478 (54.3) | 0.764 |
| Sepsis 3.0 [n (%)] | 542 (55.7) | 67 (72.0) | 475 (54.0) | 0.001 |
| Septic shock [n (%)] | 19 (2.0) | 6 (6.5) | 13 (1.5) | 0.006 |
| Vital signs | ||||
| Temperature (celsius) | 36.7 (36.5, 37.6) | 36.9 (36.5, 38.0) | 36.7 (36.4, 37.6) | 0.035 |
| Pulse rate (beats/min) | 88.0 (78.0, 102.0) | 92.0 (80.0, 112.0) | 88.0 (78.0, 102.0) | 0.019 |
| Respiratory rate (beats/min) | 20.0 (20.0, 22.0) | 20.0 (20.0, 23.0) | 20.0 (20.0, 21.0) | 0.084 |
| SBP (mm Hg) | 127.0 (110.0, 143.0) | 126.0 (106.5, 141.5) | 127.0 (110.0, 143.0) | 0.407 |
| DBP (mm Hg) | 73.0 (63.0, 82.0) | 72.0 (59.5, 83.5) | 73.5 (63.0, 82.0) | 0.311 |
| SOFA score | 2.0 (0.0, 4.0) | 3.0 (1.0, 5.0) | 2.0 (0.0, 4.0) | < 0.001 |
| Charlson corbidity index | 6.0 (4.0, 8.0) | 6.0 (4.0, 8.0) | 6.0 (4.0, 8.0) | 0.301 |
| Underlying diseases [n (%)] | ||||
| Myocardial infarction | 60 (6.2) | 10 (10.8) | 50 (5.7) | 0.053 |
| Cerebrovascular disease | 264 (27.1) | 24 (25.8) | 240 (27.3) | 0.762 |
| Dementia | 43 (4.4) | 6 (6.5) | 37 (4.2) | 0.290 |
| COPD | 67 (6.9) | 3 (3.2) | 64 (7.3) | 0.143 |
| Diabetes mellitus | 309 (31.8) | 29 (31.2) | 280 (31.8) | 0.900 |
| Chronic kidney disease | 115 (11.8) | 13 (14.0) | 102 (11.6) | 0.498 |
| Leukemia | 47 (4.8) | 5 (5.4) | 42 (4.8) | 0.798 |
| Solid Tumor | 308 (31.7) | 23 (24.7) | 285 (32.4) | 0.131 |
| Liver cirrhosis | 83 (8.5) | 3 (3.2) | 80 (9.1) | 0.054 |
| Suspected Source of infection [n (%)] | ||||
| Respiratory tract | 504 (51.8) | 51 (54.8) | 453 (51.5) | 0.537 |
| Genitourinary tract | 340 (34.9) | 33 (35.5) | 307 (34.9) | 0.908 |
| Catheter related | 75 (7.7) | 10 (10.8) | 65 (7.4) | 0.247 |
| Liver and biliary tract | 90 (9.2) | 6 (6.5) | 84 (9.5) | 0.327 |
| GI and pancreas | 67 (6.9) | 7 (7.5) | 60 (6.8) | 0.797 |
| Skin and soft tissue | 31 (3.2) | 1 (1.1) | 30 (3.4) | 0.352 |
| Other | 36 (3.7) | 2 (2.2) | 34 (3.9) | 0.569 |
| Laboratory indexes | ||||
| WBC | 7.8 (5.7, 11.6) | 8.4 (5.8, 14.6) | 7.7 (5.7, 11.4) | 0.067 |
| Hb | 113.0 (94.0, 129.0) | 104.0 (81.5, 122.5) | 114.0 (95.0, 129.0) | 0.005 |
| PLT | 200.0 (140.0, 263.5) | 168.0 (105.5, 239.5) | 203.5 (145.0, 264.8) | 0.003 |
| CRP | 37.2 (9.9, 103.0) | 53.2 (11.2, 134.7) | 35.9 (9.8, 101.6) | 0.178 |
| PCT | 0.5 (0.1, 3.6) | 0.9 (0.2, 11.2) | 0.5 (0.1, 3.0) | 0.018 |
| ALB | 36.2 (31.1, 40.2) | 34.0 (29.1, 40.1) | 36.4 (31.4, 40.3) | 0.035 |
| ALT | 18.0 (11.8, 31.0) | 18.9 (11.0.30.3) | 17.4 (12.0, 31.0) | 0.951 |
| AST | 22.0 (17.0, 38.0) | 21.0 (17.0, 37.0) | 22.4 (16.0, 38.0) | 0.780 |
| TBIL | 10.1 (6.7, 16.6) | 10.3 (6.4, 16.9) | 10.1 (6.8, 16.6) | 0.997 |
| Cr | 85.0 (65.9, 122.0) | 93.0 (69.1, 187.0) | 84.6 (65.0, 117.0) | 0.004 |
| Pathogens | ||||
| Gram-negative bacteria [n (%)] | ||||
| Escherichia coli | 281 (28.9) | 21 (22.6) | 260 (29.5) | 0.159 |
| Klebsiella pneumoniae | 101 (10.4) | 12 (12.9) | 89 (10.1) | 0.402 |
| Pseudomonas aeruginosa | 60 (6.2) | 7 (7.5) | 53 (6.0) | 0.566 |
| Acinetobacter baumannii | 55 (5.7) | 8 (8.6) | 47 (5.3) | 0.195 |
| Proteus mirabilis | 14 (1.4) | 1 (1.1) | 13 (1.5) | 1.000 |
| Stenotrophomonas Maltophilia [n (%)] | 13 (1.3) | 1 (1.1) | 12 (1.4) | 1.000 |
| Enterobacter cloacae | 13 (1.3) | 0 (0) | 13 (1.5) | 0.626 |
| Serratia marcescens | 8 (0.8) | 0 (0) | 8 (0.9) | 1.000 |
| Salmonella species | 8 (0.8) | 1 (1.1) | 7 (0.8) | 0.554 |
| Others | 57 (5.9) | 4 (4.3) | 53 (6.0) | 0.645 |
| Gram-negative bacteria [n (%)] | ||||
| Staphylococcus aureus | 87 (8.9) | 13 (14.0) | 74 (8.4) | 0.073 |
| Streptococcus pneumoniae | 7 (0.7) | 0 (0) | 7 (0.8) | 1.000 |
| Enterococcus faecium | 22 (2.3) | 3 (3.2) | 19 (2.2) | 0.459 |
| Enterococcus faecalis | 16 (1.6) | 2 (2.2) | 14 (1.6) | 0.660 |
| Streptococcus agalactiae | 11 (1.1) | 0 (0) | 11 (1.3) | 0.613 |
| Others | 55 (5.7) | 3 (3.2) | 52 (5.9) | 0.287 |
| Fungi [n (%)] | ||||
| Candida albicans | 4 (0.4) | 1 (1.1) | 3 (0.3) | 0.331 |
| Multiple bacteria | 143 (14.7) | 15 (16.1) | 128 (14.5) | 0.682 |
Table 1 Characteristics of 973 sepsis patients with BSI before PSM
| Item | Total (n = 973) | Control group (n = 93) | CHM group (n = 880) | P value |
|---|---|---|---|---|
| Age (years) | 68.0 (57.0, 80.0) | 67.0 (56.5, 79.5) | 68.0 (57.0, 80.0) | 0.894 |
| Male [n (%)] | 527 (54.2) | 49 (52.7) | 478 (54.3) | 0.764 |
| Sepsis 3.0 [n (%)] | 542 (55.7) | 67 (72.0) | 475 (54.0) | 0.001 |
| Septic shock [n (%)] | 19 (2.0) | 6 (6.5) | 13 (1.5) | 0.006 |
| Vital signs | ||||
| Temperature (celsius) | 36.7 (36.5, 37.6) | 36.9 (36.5, 38.0) | 36.7 (36.4, 37.6) | 0.035 |
| Pulse rate (beats/min) | 88.0 (78.0, 102.0) | 92.0 (80.0, 112.0) | 88.0 (78.0, 102.0) | 0.019 |
| Respiratory rate (beats/min) | 20.0 (20.0, 22.0) | 20.0 (20.0, 23.0) | 20.0 (20.0, 21.0) | 0.084 |
| SBP (mm Hg) | 127.0 (110.0, 143.0) | 126.0 (106.5, 141.5) | 127.0 (110.0, 143.0) | 0.407 |
| DBP (mm Hg) | 73.0 (63.0, 82.0) | 72.0 (59.5, 83.5) | 73.5 (63.0, 82.0) | 0.311 |
| SOFA score | 2.0 (0.0, 4.0) | 3.0 (1.0, 5.0) | 2.0 (0.0, 4.0) | < 0.001 |
| Charlson corbidity index | 6.0 (4.0, 8.0) | 6.0 (4.0, 8.0) | 6.0 (4.0, 8.0) | 0.301 |
| Underlying diseases [n (%)] | ||||
| Myocardial infarction | 60 (6.2) | 10 (10.8) | 50 (5.7) | 0.053 |
| Cerebrovascular disease | 264 (27.1) | 24 (25.8) | 240 (27.3) | 0.762 |
| Dementia | 43 (4.4) | 6 (6.5) | 37 (4.2) | 0.290 |
| COPD | 67 (6.9) | 3 (3.2) | 64 (7.3) | 0.143 |
| Diabetes mellitus | 309 (31.8) | 29 (31.2) | 280 (31.8) | 0.900 |
| Chronic kidney disease | 115 (11.8) | 13 (14.0) | 102 (11.6) | 0.498 |
| Leukemia | 47 (4.8) | 5 (5.4) | 42 (4.8) | 0.798 |
| Solid Tumor | 308 (31.7) | 23 (24.7) | 285 (32.4) | 0.131 |
| Liver cirrhosis | 83 (8.5) | 3 (3.2) | 80 (9.1) | 0.054 |
| Suspected Source of infection [n (%)] | ||||
| Respiratory tract | 504 (51.8) | 51 (54.8) | 453 (51.5) | 0.537 |
| Genitourinary tract | 340 (34.9) | 33 (35.5) | 307 (34.9) | 0.908 |
| Catheter related | 75 (7.7) | 10 (10.8) | 65 (7.4) | 0.247 |
| Liver and biliary tract | 90 (9.2) | 6 (6.5) | 84 (9.5) | 0.327 |
| GI and pancreas | 67 (6.9) | 7 (7.5) | 60 (6.8) | 0.797 |
| Skin and soft tissue | 31 (3.2) | 1 (1.1) | 30 (3.4) | 0.352 |
| Other | 36 (3.7) | 2 (2.2) | 34 (3.9) | 0.569 |
| Laboratory indexes | ||||
| WBC | 7.8 (5.7, 11.6) | 8.4 (5.8, 14.6) | 7.7 (5.7, 11.4) | 0.067 |
| Hb | 113.0 (94.0, 129.0) | 104.0 (81.5, 122.5) | 114.0 (95.0, 129.0) | 0.005 |
| PLT | 200.0 (140.0, 263.5) | 168.0 (105.5, 239.5) | 203.5 (145.0, 264.8) | 0.003 |
| CRP | 37.2 (9.9, 103.0) | 53.2 (11.2, 134.7) | 35.9 (9.8, 101.6) | 0.178 |
| PCT | 0.5 (0.1, 3.6) | 0.9 (0.2, 11.2) | 0.5 (0.1, 3.0) | 0.018 |
| ALB | 36.2 (31.1, 40.2) | 34.0 (29.1, 40.1) | 36.4 (31.4, 40.3) | 0.035 |
| ALT | 18.0 (11.8, 31.0) | 18.9 (11.0.30.3) | 17.4 (12.0, 31.0) | 0.951 |
| AST | 22.0 (17.0, 38.0) | 21.0 (17.0, 37.0) | 22.4 (16.0, 38.0) | 0.780 |
| TBIL | 10.1 (6.7, 16.6) | 10.3 (6.4, 16.9) | 10.1 (6.8, 16.6) | 0.997 |
| Cr | 85.0 (65.9, 122.0) | 93.0 (69.1, 187.0) | 84.6 (65.0, 117.0) | 0.004 |
| Pathogens | ||||
| Gram-negative bacteria [n (%)] | ||||
| Escherichia coli | 281 (28.9) | 21 (22.6) | 260 (29.5) | 0.159 |
| Klebsiella pneumoniae | 101 (10.4) | 12 (12.9) | 89 (10.1) | 0.402 |
| Pseudomonas aeruginosa | 60 (6.2) | 7 (7.5) | 53 (6.0) | 0.566 |
| Acinetobacter baumannii | 55 (5.7) | 8 (8.6) | 47 (5.3) | 0.195 |
| Proteus mirabilis | 14 (1.4) | 1 (1.1) | 13 (1.5) | 1.000 |
| Stenotrophomonas Maltophilia [n (%)] | 13 (1.3) | 1 (1.1) | 12 (1.4) | 1.000 |
| Enterobacter cloacae | 13 (1.3) | 0 (0) | 13 (1.5) | 0.626 |
| Serratia marcescens | 8 (0.8) | 0 (0) | 8 (0.9) | 1.000 |
| Salmonella species | 8 (0.8) | 1 (1.1) | 7 (0.8) | 0.554 |
| Others | 57 (5.9) | 4 (4.3) | 53 (6.0) | 0.645 |
| Gram-negative bacteria [n (%)] | ||||
| Staphylococcus aureus | 87 (8.9) | 13 (14.0) | 74 (8.4) | 0.073 |
| Streptococcus pneumoniae | 7 (0.7) | 0 (0) | 7 (0.8) | 1.000 |
| Enterococcus faecium | 22 (2.3) | 3 (3.2) | 19 (2.2) | 0.459 |
| Enterococcus faecalis | 16 (1.6) | 2 (2.2) | 14 (1.6) | 0.660 |
| Streptococcus agalactiae | 11 (1.1) | 0 (0) | 11 (1.3) | 0.613 |
| Others | 55 (5.7) | 3 (3.2) | 52 (5.9) | 0.287 |
| Fungi [n (%)] | ||||
| Candida albicans | 4 (0.4) | 1 (1.1) | 3 (0.3) | 0.331 |
| Multiple bacteria | 143 (14.7) | 15 (16.1) | 128 (14.5) | 0.682 |
| Item | Total group (n = 176) | Control group (n = 88) | CHM group (n = 88) | P value |
|---|---|---|---|---|
| Age (years) | 67.0 (57.3, 79.0) | 67.5 (57.3, 79.0) | 67.0 (57.3, 78.8) | 0.731 |
| Male sex [n (%)] | 84 (47.7) | 43 (48.9) | 41 (46.6) | 0.763 |
| SOFA score | 3.0 (1.0, 5.0) | 3.0 (1.0, 5.0) | 3.0 (1.0, 5.0) | 0.751 |
| CCI | 6.0 (4.0, 9.0) | 6.0 (4.0, 8.0) | 6.5 (4.0, 9.0) | 0.193 |
| Sepsis 3.0 [n (%)] | 122 (69.3) | 62 (70.5) | 60 (68.2) | 0.744 |
| Septic shock [n (%)] | 6 (3.4) | 4 (4.5) | 2 (2.3) | 0.682 |
| Temperature (℃) | 36.8 (36.5, 37.7) | 36.9 (36.5, 38.0) | 36.7 (36.4, 37.5) | 0.169 |
| Pulse rate (beats/min) | 91.0 (79.3, 110.0) | 92.0 (79.3, 111.5) | 90.5 (79.3, 109.0) | 0.932 |
| Hb (g/L) | 106.0 (82.5, 127.0) | 103.5 (80.5, 124.5) | 107.0 (84.0, 129.0) | 0.485 |
| PLT (109/L) | 187.0 (119.3, 253.5) | 171.0 (108.8, 241.8) | 220.5 (123.5, 274.0) | 0.053 |
| PCT (ng /mL) | 0.7 (0.2, 6.2) | 0.8 (0.2, 8.1) | 0.7 (0.2, 3.6) | 0.823 |
| ALB (g/L) | 34.3 (29.3, 38.8) | 34.0 (29.2, 40.4) | 34.8 (30.4, 38.7) | 0.933 |
| Cr (μmol/L) | 90.5 (67.1, 177.6) | 91.4 (68.1, 180.3) | 90.5 (63.1, 156.9) | 0.443 |
Table 2 Characteristics of 176 sepsis patients with BSI after PSM
| Item | Total group (n = 176) | Control group (n = 88) | CHM group (n = 88) | P value |
|---|---|---|---|---|
| Age (years) | 67.0 (57.3, 79.0) | 67.5 (57.3, 79.0) | 67.0 (57.3, 78.8) | 0.731 |
| Male sex [n (%)] | 84 (47.7) | 43 (48.9) | 41 (46.6) | 0.763 |
| SOFA score | 3.0 (1.0, 5.0) | 3.0 (1.0, 5.0) | 3.0 (1.0, 5.0) | 0.751 |
| CCI | 6.0 (4.0, 9.0) | 6.0 (4.0, 8.0) | 6.5 (4.0, 9.0) | 0.193 |
| Sepsis 3.0 [n (%)] | 122 (69.3) | 62 (70.5) | 60 (68.2) | 0.744 |
| Septic shock [n (%)] | 6 (3.4) | 4 (4.5) | 2 (2.3) | 0.682 |
| Temperature (℃) | 36.8 (36.5, 37.7) | 36.9 (36.5, 38.0) | 36.7 (36.4, 37.5) | 0.169 |
| Pulse rate (beats/min) | 91.0 (79.3, 110.0) | 92.0 (79.3, 111.5) | 90.5 (79.3, 109.0) | 0.932 |
| Hb (g/L) | 106.0 (82.5, 127.0) | 103.5 (80.5, 124.5) | 107.0 (84.0, 129.0) | 0.485 |
| PLT (109/L) | 187.0 (119.3, 253.5) | 171.0 (108.8, 241.8) | 220.5 (123.5, 274.0) | 0.053 |
| PCT (ng /mL) | 0.7 (0.2, 6.2) | 0.8 (0.2, 8.1) | 0.7 (0.2, 3.6) | 0.823 |
| ALB (g/L) | 34.3 (29.3, 38.8) | 34.0 (29.2, 40.4) | 34.8 (30.4, 38.7) | 0.933 |
| Cr (μmol/L) | 90.5 (67.1, 177.6) | 91.4 (68.1, 180.3) | 90.5 (63.1, 156.9) | 0.443 |
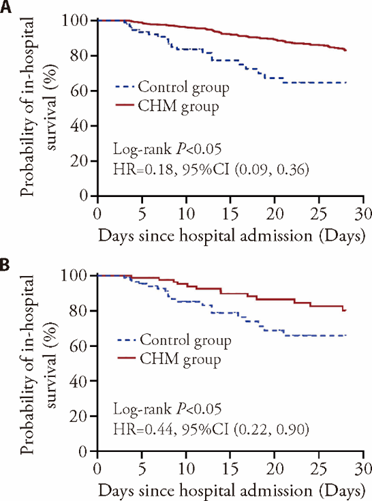
Figure 2 Srvival analysis of all-cause 28-day death in sepsis patients with BSI A: survival analysis of all-cause 28-day death in sepsis patients with BSI comparing CHM group (n = 93) and control group (n = 880) before PSM; B: survival analysis of all-cause 28-day death in sepsis patients with BSI comparing CHM group (n = 88) and control group (n = 88) after PSM. Control group was given conventional therapy, CHM group was given conventional therapy plus CHM, the categories, doses, and treatment courses of CHM prescribed were unlimited, BSI: bloodstream infection; CHM: Chinese herbal medicine. 28-day mortality was estimated by the Kaplan-Meier survival analysis and compared using the log-rank test.
| Item | Control group (n = 88) | CHM group (n = 88) | P value |
|---|---|---|---|
| 28 d mortality | 19 (21.6) | 13 (14.8) | 0.241 |
| In-hospital mortality | 23 (26.1) | 24 (27.3) | 0.865 |
| 7 d mortality | 6 (6.80) | 2 (2.3) | 0.278 |
| Noninvasive ventilation | 24 (27.3) | 27 (30.7) | 0.618 |
| Invasive ventilation | 20 (22.7) | 25 (28.4) | 0.388 |
| Vasoactive drugs | 20 (22.7) | 12 (13.6) | 0.118 |
| Cardiopulmonary resuscitation | 12 (13.6) | 12 (13.6) | 1.000 |
Table 3 Outcomes and complications of 176 sepsis patients with BSI after PSM [n (%)]
| Item | Control group (n = 88) | CHM group (n = 88) | P value |
|---|---|---|---|
| 28 d mortality | 19 (21.6) | 13 (14.8) | 0.241 |
| In-hospital mortality | 23 (26.1) | 24 (27.3) | 0.865 |
| 7 d mortality | 6 (6.80) | 2 (2.3) | 0.278 |
| Noninvasive ventilation | 24 (27.3) | 27 (30.7) | 0.618 |
| Invasive ventilation | 20 (22.7) | 25 (28.4) | 0.388 |
| Vasoactive drugs | 20 (22.7) | 12 (13.6) | 0.118 |
| Cardiopulmonary resuscitation | 12 (13.6) | 12 (13.6) | 1.000 |
| Item | Control group (n = 764) | BASEH group (n = 209) | P value |
|---|---|---|---|
| 28 d mortality | 106 (13.9) | 15 (7.2) | 0.009 |
| In-hospital mortality | 163 (21.3) | 31 (14.8) | 0.037 |
| 7 d mortality | 27 (3.5) | 1 (0.5) | 0.019 |
| Noninvasive ventilation | 202 (26.4) | 44 (21.1) | 0.112 |
| Invasive ventilation | 168 (22.0) | 51 (24.4) | 0.459 |
| Vasoactive drugs | 115 (15.1) | 21 (10.0) | 0.064 |
| Cardiopulmonary resuscitation | 85 (11.1) | 12 (5.7) | 0.021 |
Table 4 Outcomes and complications of 973 sepsis patients with BSI prescribed with BASED or without [n (%)]
| Item | Control group (n = 764) | BASEH group (n = 209) | P value |
|---|---|---|---|
| 28 d mortality | 106 (13.9) | 15 (7.2) | 0.009 |
| In-hospital mortality | 163 (21.3) | 31 (14.8) | 0.037 |
| 7 d mortality | 27 (3.5) | 1 (0.5) | 0.019 |
| Noninvasive ventilation | 202 (26.4) | 44 (21.1) | 0.112 |
| Invasive ventilation | 168 (22.0) | 51 (24.4) | 0.459 |
| Vasoactive drugs | 115 (15.1) | 21 (10.0) | 0.064 |
| Cardiopulmonary resuscitation | 85 (11.1) | 12 (5.7) | 0.021 |
| 1. |
Singer M, Deutschman CS, Seymour CW, et al. The third international consensus definitions for sepsis and septic shock (Sepsis-3). JAMA 2016; 315: 801-10.
DOI PMID |
| 2. |
Levy MM, Fink MP, Marshall JC, et al. 2001 SCCM/ESICM/ACCP/ATS/SIS international sepsis definitions conference. Intensive Care Med 2003; 29: 530-8.
DOI URL |
| 3. |
Evans L, Rhodes A, Alhazzani W, et al. Surviving sepsis campaign: international guidelines for management of sepsis and septic shock 2021. Intensive Care Med 2021; 47: 1181-247.
DOI PMID |
| 4. |
Fleischmann C, Scherag A, Adhikari NK, et al. Assessment of global incidence and mortality of hospital-treated sepsis. Current estimates and limitations. Am J Respir Crit Care Med 2016; 193: 259-72.
DOI URL |
| 5. |
Biwersi C, Hepping N, Bode U, et al. Bloodstream infections in a German paediatric oncology unit: prolongation of inpatient treatment and additional costs. Int J Hyg Environ Health 2009; 212: 541-6.
DOI URL |
| 6. |
Mehl A, Åsvold BO, Lydersen S, et al. Burden of bloodstream infection in an area of Mid-Norway 2002-2013: a prospective population-based observational study. BMC Infect Dis 2017; 17: 205.
DOI PMID |
| 7. | Ababneh MA, Rababa'h AM, Almomani BA, Ayoub AM, Al-Azzam SI. A ten-year surveillance of P aeruginosa bloodstream infections in a tertiary care hospital: trends and risk factors for mortality. Int J Clin Pract 2021; 75: e14409. |
| 8. |
Amanati A, Sajedianfard S, Khajeh S, et al. Bloodstream infections in adult patients with malignancy, epidemiology, microbiology, and risk factors associated with mortality and multi-drug resistance. BMC Infect Dis 2021; 21: 636.
DOI PMID |
| 9. |
Laupland KB, Davies HD, Church DL, et al. Bloodstream infection-associated sepsis and septic shock in critically ill adults: a population-based study. Infection 2004; 32: 59-64.
DOI PMID |
| 10. |
Rodríguez-Baño J, de Cueto M, Retamar P, Gálvez-Acebal J. Current management of bloodstream infections. Expert Rev Anti Infect Ther 2010; 8: 815-29.
DOI PMID |
| 11. |
Liu QQ. Based on the four segments and treatment by syndrome differentiation to lower the mortality of sepsis. Chin J Integr Med 2009; 15: 16-8.
DOI URL |
| 12. | Lai F, Zhang Y, Xie DP, et al. A systematic review of Rhubarb (a Traditional Chinese Medicine) used for the treatment of experimental sepsis. Evid Based Complement Alternat Med 2015; 2015: 131283. |
| 13. |
Wang Z, Chen W, Li Y, et al. Reduning injection and its effective constituent luteoloside protect against sepsis partly via inhibition of HMGB1/TLR4/NF-κB/MAPKs signaling pathways. J Ethnopharmacol 2021; 270: 113783.
DOI URL |
| 14. |
Fan TT, Cheng BL, Fang XM, Chen YC, Su F. Application of Chinese medicine in the management of critical conditions: a review on sepsis. Am J Chin Med 2020; 48: 1315-30.
DOI URL |
| 15. |
Zhao GZ, Chen RB, Li B, et al. Clinical practice guideline on Traditional Chinese Medicine therapy alone or combined with antibiotics for sepsis. Ann Transl Med 2019; 7: 122.
DOI URL |
| 16. |
Vincent JL, Moreno R, Takala J, et al. The SOFA (sepsis-related organ failure assessment) score to describe organ dysfunction/failure. On behalf of the working group on sepsis-related problems of the European society of intensive care medicine. Intensive Care Med 1996; 22: 707-10.
DOI URL |
| 17. |
Fried L, Bernardini J, Piraino B. Charlson comorbidity index as a predictor of outcomes in incident peritoneal dialysis patients. Am J Kidney Dis 2001; 37: 337-42.
DOI PMID |
| 18. |
Al Mohajer M, Darouiche RO. Sepsis syndrome, bloodstream infections, and device-related infections. Med Clin North Am 2012; 96: 1203-23.
DOI URL |
| 19. |
Lelubre C, Vincent JL. Mechanisms and treatment of organ failure in sepsis. Nat Rev Nephrol 2018; 14: 417-27.
DOI PMID |
| 20. | Gotts JE, Matthay MA. Sepsis: pathophysiology and clinical management. BMJ 2016; 353: i1585. |
| 21. | Yin J, Yu Z, Hou C, Peng Y, Xiao J, Jiang J. Protective Effect of Zuojin Fang on lung injury induced by sepsis through downregulating the JAK1/STAT3 signaling pathway. Biomed Res Int 2021; 2021: 1419631. |
| 22. |
Ma H, Kou J, Zhu D, Yan Y, Yu B. Liu-Shen-Wan, a Traditional Chinese Medicine, improves survival in sepsis induced by cecal ligation and puncture via reducing TNF-alpha levels, MDA content and enhancing macrophage phagocytosis. Int Immunopharmacol 2006; 6: 1355-62.
DOI URL |
| 23. |
Liu J, Wang Z, Lin J, et al. Xuebijing injection in septic rats mitigates kidney injury, reduces cortical microcirculatory disorders, and suppresses activation of local inflammation. J Ethnopharmacol 2021; 276: 114199.
DOI URL |
| 24. |
Gao M, Ou H, Jiang Y, et al. Tanshinone ⅡA attenuates sepsis-induced immunosuppression and improves survival rate in a mice peritonitis model. Biomed Pharmacother 2019; 112: 108609.
DOI URL |
| 25. |
Xing X, Zhi Y, Lu J, et al. Traditional Chinese Medicine bundle therapy for septic acute gastrointestinal injury: a multicenter randomized controlled trial. Complement Ther Med 2019; 47: 102194.
DOI URL |
| 26. |
Li C, Wang P, Zhang L, et al. Efficacy and safety of Xuebijing injection (a Chinese patent) for sepsis: a Meta-analysis of randomized controlled trials. J Ethnopharmacol 2018; 224: 512-21.
DOI PMID |
| 27. |
Li MQ, Pan CG, Wang XM, et al. Effect of the Shenfu injection combined with early goal-directed therapy on organ functions and outcomes of septic shock patients. Cell Biochem Biophys 2015; 72: 807-12.
DOI URL |
| 28. |
Liang X, Zhou M, Ge XY, et al. Efficacy of Traditional Chinese Medicine on sepsis: a systematic review and Meta-analysis. Int J Clin Exp Med 2015; 8: 20024-34.
PMID |
| 29. |
Zhang Y, Du M, Chang Y, Chen LA, Zhang Q. Incidence, clinical characteristics, and outcomes of nosocomial enterococcus spp. bloodstream infections in a tertiary-care hospital in Beijing, China: a four-year retrospective study. Antimicrob Resist Infect Control 2017; 6: 73.
DOI URL |
| 30. |
Raghunathan K, Shaw A, Nathanson B, et al. Association between the choice of IV crystalloid and in-hospital mortality among critically ill adults with sepsis. Crit Care Med 2014; 42: 1585-91.
DOI PMID |
| 31. |
Iba T, Umemura Y, Wada H, Levy JH. Roles of coagulation abnormalities and microthrombosis in sepsis: pathophysiology, diagnosis, and treatment. Arch Med Res 2021; 52: 788-97.
DOI URL |
| 32. |
Giustozzi M, Ehrlinder H, Bongiovanni D, et al. Coagulopathy and sepsis: pathophysiology, clinical manifestations and treatment. Blood Rev 2021; 50: 100864.
DOI URL |
| 33. |
Tsao CM, Ho ST, Wu CC. Coagulation abnormalities in sepsis. Acta Anaesthesiol Taiwan 2015; 53: 16-22.
DOI URL |
| 34. |
Ying J, Wu J, Zhang Y, et al. Ligustrazine suppresses renal NMDAR1 and caspase-3 expressions in a mouse model of sepsis-associated acute kidney injury. Mol Cell Biochem 2020; 464: 73-81.
DOI PMID |
| 35. | Meng ZJ, Wang C, Meng LT, Bao BH, Wu JH, Hu YQ. Sodium tanshinone ⅡA sulfonate attenuates cardiac dysfunction and improves survival of rats with cecal ligation and puncture-induced sepsis. Chin J Nat Med 2018; 16: 846-55. |
| 36. |
Zhu W, Lu Q, Wan L, Feng J, Chen HW. Sodium tanshinone Ⅱ A sulfonate ameliorates microcirculatory disturbance of small intestine by attenuating the production of reactie oxygen species in rats with sepsis. Chin J Integr Med 2016; 22: 745-51.
DOI URL |
| [1] | WANG Lili, FENG Ju, ZHAN Daqian, WANG Junshuai, ZHOU Daixing. Protective effects of tanshinone ⅡA on sepsis-induced multiple organ dysfunction: a literature review [J]. Journal of Traditional Chinese Medicine, 2023, 43(5): 1040-1046. |
| [2] | LIN Yi, LI Xun, WANG Zi, ZHENG Xiaoran, HANG Haiyan, LI Lingling. Efficacy and safety of external application of Chinese herbal medicine for psoriasis vulgaris: a systematic review of randomized controlled trials [J]. Journal of Traditional Chinese Medicine, 2022, 42(4): 493-504. |
| [3] | YAN Lizhao, MAO Fuwei, CAO Yinghao, XIE Mao. Clinical effects of the combination of Traditional Chinese and Western Medicines on coronavirus disease 2019: a systematic review and Meta-analysis [J]. Journal of Traditional Chinese Medicine, 2021, 41(4): 499-506. |
| [4] | CHEN Jiayang, FENG Li. Traditional Chinese Medicine reverses resistance to epidermal growth factor receptor tyrosine kinase inhibitors in advanced non-small cell lung cancer: a narrative review [J]. Journal of Traditional Chinese Medicine, 2021, 41(4): 650-656. |
| [5] | Emel Akta?, Hilal Yildiran. Antioxidant and ntiinflammatory efficacy of curcumin on lung tissue in rats with sepsis [J]. Journal of Traditional Chinese Medicine, 2020, 40(5): 820-826. |
| [6] | Zhang Jinchao, Hu Jing, He Xiujuan, Meng Yujiao, Chen Guangkun, Chen Zhaoxia, Lü Jingjing, Li Ping. Effectiveness of Chinese herbal medicine for primary Raynaud's phenomenon: a systematic review and Meta-analysis of randomized controlled trials [J]. Journal of Traditional Chinese Medicine, 2020, 40(4): 509-517. |
| [7] | Liu Jin, Liu Fusheng, Liang Tengxiao, Cao Po, Li Jing, Zhang Yin, Liu Yang. Efficacy of Shenfu decoction on sepsis in rats with condition induced by cecal ligation and puncture [J]. Journal of Traditional Chinese Medicine, 2020, 40(4): 621-628. |
| [8] | Bumjung Kim, Cheolmin Jo, Somin Lee, Hanna Choi, Kwang-Woo Kim, Inhye Ham, Ho-Young Choi, Kyungjin Lee. Vasorelaxant effects of 50 commonly used traditional herbal prescriptions on isolated rat aortic rings [J]. Journal of Traditional Chinese Medicine, 2020, 40(4): 629-639. |
| [9] | Hou Yi, Wang Tieshan, Guo Xiangyu, Sun Wen, Guo Xuan, Wu Lili, Qin Lingling, Zhang Chengfei, Liu Tonghua. Protective effects of Jiayan Kangtai granules on autoimmune thyroiditis in a rat model by modulating Th17/Treg cell balance [J]. Journal of Traditional Chinese Medicine, 2018, 38(03): 380-390. |
| [10] | Li Jing, Zheng Chunquan, Lin Hai, Yang Chen, Gu Siyuan, Wang Yi, Duan Honggang. Effect of Zhu-yuan decoction in patients with chronic rhinosinusitis after functional endoscopic sinus surgery [J]. Journal of Traditional Chinese Medicine, 2018, 38(01): 83-88. |
| [11] | Zhang Hongwei, Wei Liyou, Zhao Gang, Liu Shuzheng, Zhang Zhenyu, Zhang Jing, Yang Yajing. Protective effect of Xuebijing injection on myocardial injury in patients with sepsis: a randomized clinical trial [J]. Journal of Traditional Chinese Medicine, 2016, 36(06): 706-710. |
| [12] | Sun Yanni, Sun Lijing, Liu Shuqing, Song Juan, Cheng Jiejing, Liu Jun. Effect of emodin on Aquaporin 5 expression in rats with sepsis-induced acute lung injury [J]. Journal of Traditional Chinese Medicine, 2015, 35(06): 679-684. |
| [13] | Hongwei Zhang, Liyou Wei, Zhenyu Zhang, Shuzheng Liu, Gang Zhao, Jing Zhang, Yanling Hu. Protective effect of periplaneta americana extract on intestinal mucosal barrier function in patients with sepsis [J]. Journal of Traditional Chinese Medicine, 2013, 33(01): 70-73. |
| Viewed | ||||||
|
Full text |
|
|||||
|
Abstract |
|
|||||


